GABAergic MOA - The Brain's Brakes
-
GABA (γ-aminobutyric acid): The main inhibitory CNS neurotransmitter. It binds to GABA-A receptors, opening Cl⁻ channels to hyperpolarize neurons and ↓ firing.
-
Mechanism Classes:
- Allosteric Modulators (GABA-A Receptor):
- Benzodiazepines (e.g., Diazepam): ↑ Frequency of Cl⁻ channel opening.
- Barbiturates (e.g., Phenobarbital): ↑ Duration of Cl⁻ channel opening.
- Reuptake Inhibitor:
- Tiagabine: Blocks GABA transporter (GAT-1), ↑ synaptic GABA.
- Metabolism Inhibitor:
- Vigabatrin: Irreversibly inhibits GABA transaminase, ↑ GABA levels.
- Allosteric Modulators (GABA-A Receptor):
⭐ Benzodiazepines increase channel opening frequency; Barbiturates increase its duration. This difference underlies the higher toxicity risk of barbiturates.
📌 Mnemonic: Benzos = More Zipping open (Frequency). Barbiturates = Prolonged Duration.
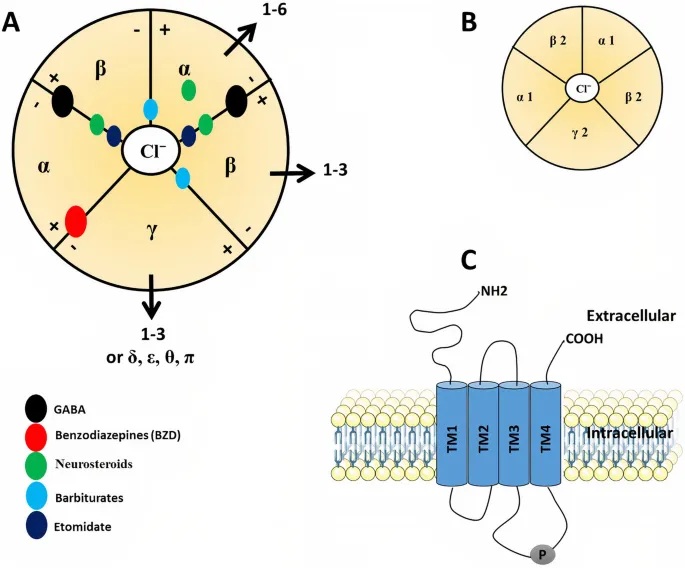
Benzodiazepines & Barbiturates - Frequency vs. Duration
- Mechanism: Both potentiate GABA-A receptor activity, leading to ↑ Cl⁻ influx and neuronal hyperpolarization.
- Benzodiazepines (e.g., Diazepam, Lorazepam)
- Increase the frequency of Cl⁻ channel opening.
- Safer profile as they require GABA to be present.
- Antidote: Flumazenil.
- Barbiturates (e.g., Phenobarbital, Thiopental)
- Increase the duration of Cl⁻ channel opening.
- Can directly open the channel at high doses (GABA-mimetic).
- Higher risk of toxicity and respiratory depression; no antidote.
📌 Mnemonic: Frenzo-diazepines for Frequency; Barbi-dur-ates for Duration.
⭐ At high doses, barbiturates can act as direct GABA-A agonists, opening the Cl⁻ channel even without GABA. This mechanism underlies their severe toxicity and narrow therapeutic window.
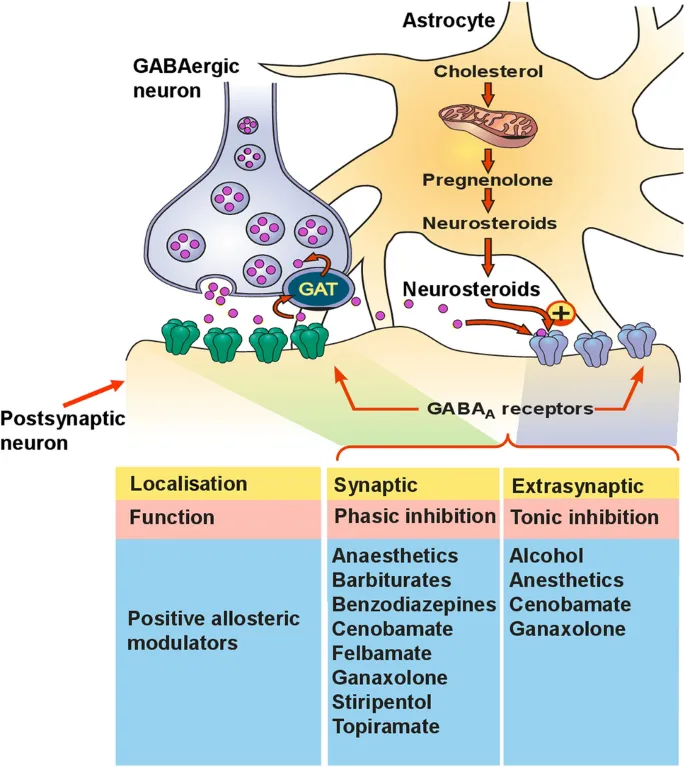
Newer GABAergics - The Niche Modulators
-
Vigabatrin
- MOA: Irreversibly inhibits GABA transaminase (GABA-T) → ↑GABA levels at the synapse.
- Use: Reserved for refractory complex partial seizures and infantile spasms.
- Adverse: ⚠️ BLACK BOX WARNING for permanent bilateral concentric visual field loss.
-
Tiagabine
- MOA: Inhibits GABA reuptake transporter (GAT-1) → ↓GABA reuptake from the synapse.
- Use: Adjunctive treatment for partial-onset seizures.
- Adverse: Dizziness, somnolence; can induce seizures in non-epileptic patients.
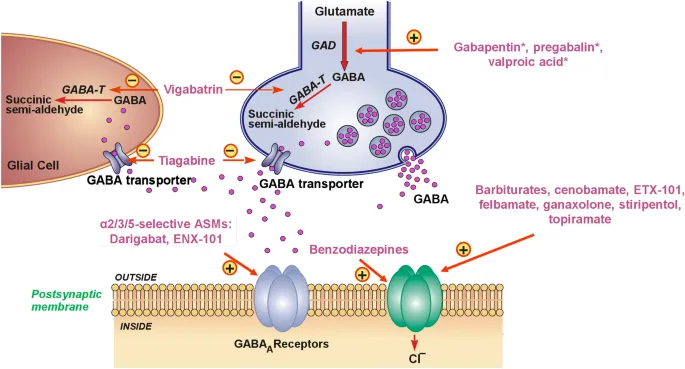
⭐ Vigabatrin is a last-resort agent due to its unique mechanism and severe, irreversible ocular toxicity. Regular visual field testing is mandatory during therapy.
Clinical Use & Toxicity - Handle With Care
-
Clinical Use
- Benzodiazepines (Lorazepam, Diazepam): First-line for acute status epilepticus; eclampsia seizures.
- Barbiturates (Phenobarbital): Neonatal seizures; refractory status epilepticus. Use limited by side effect profile.
- Vigabatrin: Infantile spasms (📌 Viga**"baby"**trin), refractory complex partial seizures.
- Tiagabine: Adjunctive therapy for partial seizures.
-
Toxicity & Side Effects
- All: Sedation, ataxia, tolerance, dependence. ⚠️ CNS & respiratory depression potentiated by alcohol/opioids.
- Vigabatrin: ⚠️ Permanent bilateral visual field loss in >30% of patients.
- Tiagabine: May paradoxically induce seizures/stupor.
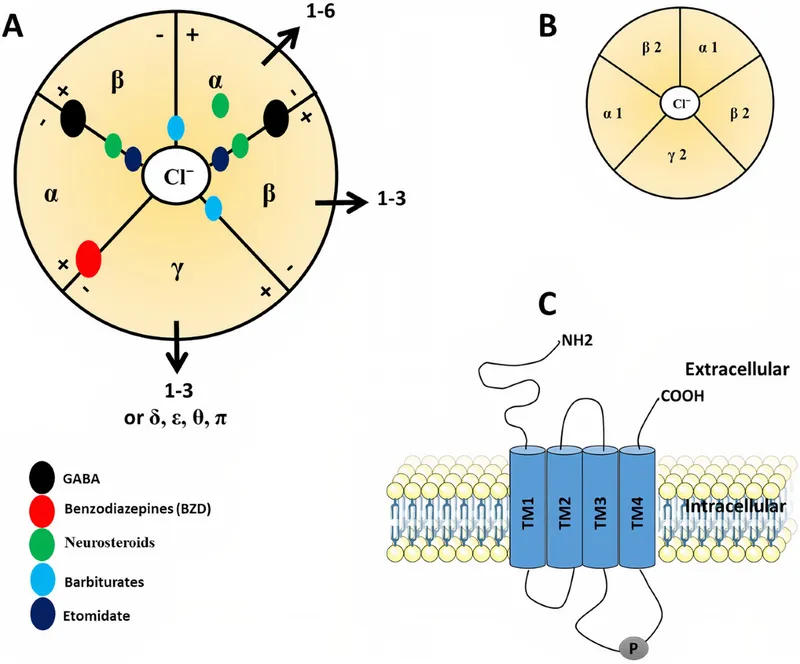
⭐ While barbiturates directly open $Cl^-$ channels, benzodiazepines only increase the frequency of channel opening in the presence of GABA, giving them a better safety profile in overdose (when taken alone).
High‑Yield Points - ⚡ Biggest Takeaways
- Benzodiazepines and barbiturates enhance GABAa receptors; benzos ↑ frequency of channel opening, while barbiturates ↑ duration.
- Vigabatrin irreversibly inhibits GABA transaminase, which increases presynaptic GABA levels.
- Tiagabine inhibits GABA reuptake (GAT-1), thereby increasing synaptic GABA concentration.
- Valproate and Topiramate have multiple mechanisms, including the potentiation of GABAergic activity.
- Common side effects include sedation, ataxia, and dizziness due to CNS depression.
- Abrupt cessation can precipitate withdrawal seizures.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

