Cholinergic Receptors - The Body's Light Switches
-
Two main types: Muscarinic (G-protein coupled) & Nicotinic (ligand-gated ion channels).
-
Muscarinic (M) Receptors:
- M1 (Gq): CNS, enteric nervous system.
- M2 (Gi): Heart (↓ heart rate, ↓ contractility).
- M3 (Gq): Glands (↑ secretion), smooth muscle (contraction), endothelium (↑NO → vasodilation).
- 📌 Mnemonic (G-protein type): "QIQ" for M1, M2, M3.
-
Nicotinic (N) Receptors:
- Nn (neuronal): Autonomic ganglia, adrenal medulla.
- Nm (muscle): Neuromuscular junction → skeletal muscle contraction.
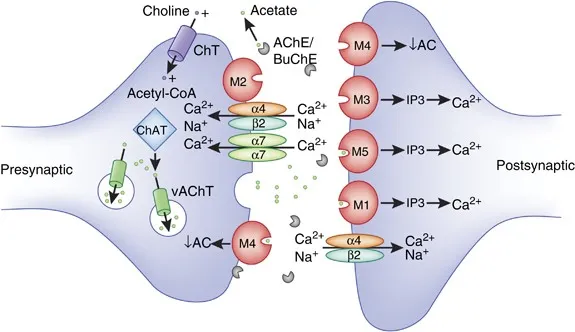
⭐ High-Yield: Atropine is a muscarinic antagonist. Low doses preferentially block presynaptic M1 receptors that inhibit ACh release, leading to a paradoxical transient bradycardia before the expected tachycardia from postsynaptic M2 blockade dominates.
Direct Agonists - The Master Keys
- Directly bind & activate cholinergic (muscarinic/nicotinic) receptors, mimicking acetylcholine (ACh).
- Types:
- Choline Esters: Bethanechol, Carbachol, Methacholine.
- Alkaloids: Pilocarpine (tertiary amine, can cross CNS).
| Drug | Receptor Target (M/N) | Key Clinical Use |
|---|---|---|
| Bethanechol | M > N | Post-op ileus, urinary retention |
| Carbachol | M, N | Glaucoma, miosis induction |
| Pilocarpine | M > N | Sjögren's (dry mouth), glaucoma |
| Methacholine | M > N | Bronchial challenge test for asthma |
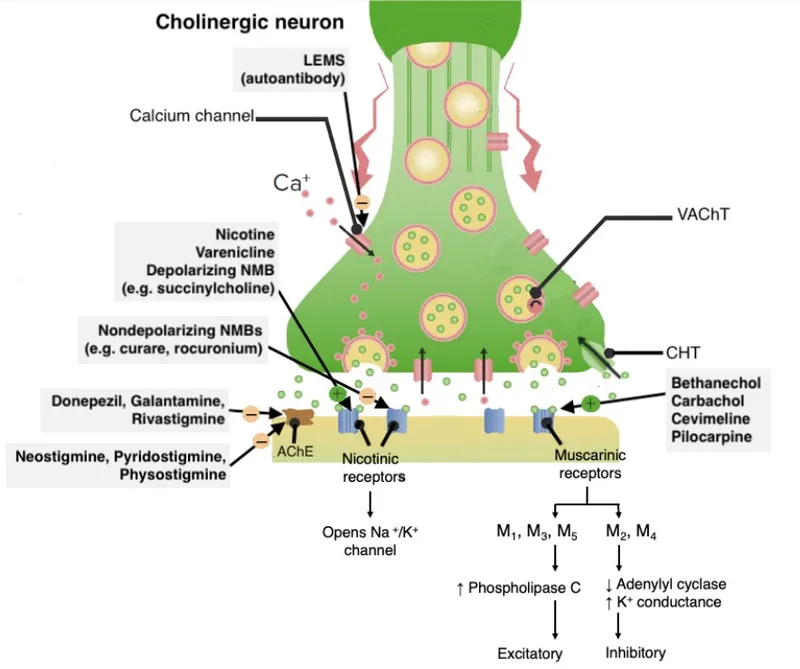
Indirect Agonists - The Volume Knobs
These drugs boost acetylcholine (ACh) concentration in the synaptic cleft by inhibiting acetylcholinesterase (AChE), the enzyme responsible for ACh breakdown. This effectively "turns up the volume" on existing cholinergic signals.
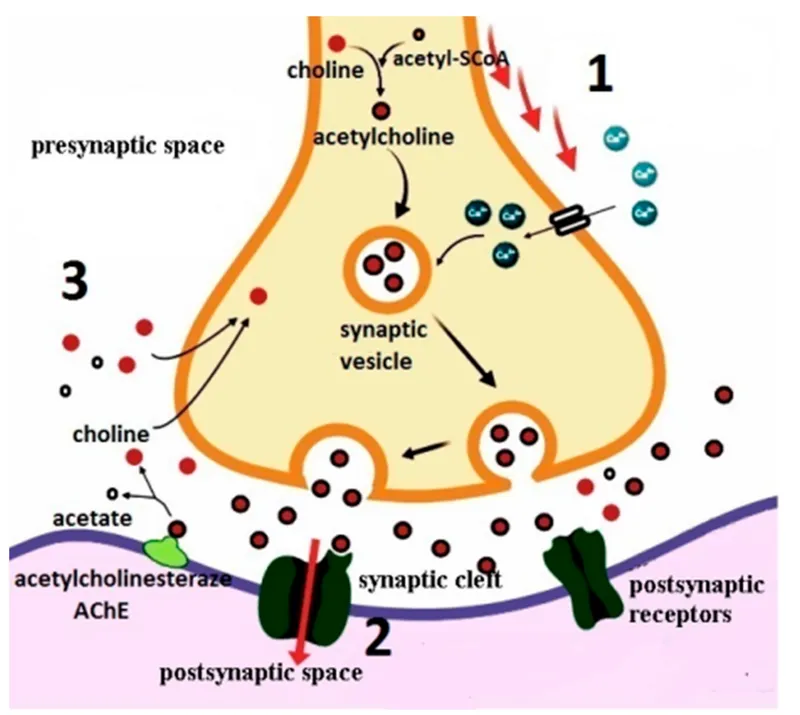
-
Reversible Inhibitors
- -stigmines: Neostigmine, Pyridostigmine (Myasthenia Gravis), Physostigmine (Atropine OD).
- Alzheimer's Disease: Donepezil, Rivastigmine, Galantamine (CNS-acting).
-
Irreversible Inhibitors (Organophosphates)
- Toxic agents (e.g., parathion, sarin gas).
- Cause cholinergic crisis (overstimulation).
- 📌 DUMBBELSS: Diarrhea, Urination, Miosis, Bronchospasm, Bradycardia, Emesis, Lacrimation, Salivation, Sweating.
⭐ Pralidoxime (2-PAM) regenerates AChE after organophosphate poisoning but must be given before the enzyme-inhibitor complex "ages." It does not cross the BBB and primarily treats nicotinic (e.g., muscle weakness) effects, while atropine manages muscarinic symptoms.
Cholinergic Crisis - DUMBBELSS Overload
- Results from excess acetylcholine (ACh), typically due to organophosphate poisoning which irreversibly inhibits acetylcholinesterase (AChE).
- 📌 DUMBBELSS Mnemonic for muscarinic effects:
- Diaphoresis / Diarrhea
- Urination
- Miosis (pinpoint pupils)
- Bronchospasm / Bradycardia
- Emesis
- Lacrimation
- Salivation / Sweating
⭐ Pralidoxime regenerates AChE to reverse muscle paralysis but does not cross the BBB; Atropine is required to reverse central and peripheral muscarinic symptoms.
High-Yield Points - ⚡ Biggest Takeaways
- Direct agonists like Bethanechol treat non-obstructive urinary retention, while Pilocarpine manages glaucoma and Sjögren's syndrome.
- Indirect agonists (-stigmines) are mainstays for Myasthenia Gravis; Donepezil is used for Alzheimer's disease.
- Organophosphate poisoning causes a cholinergic crisis (DUMBBELSS), a classic toxidrome.
- The antidote for organophosphate toxicity is Atropine (muscarinic antagonist) plus Pralidoxime (regenerates AChE).
- Edrophonium is a short-acting agent historically used in the Tensilon test to diagnose Myasthenia Gravis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

