Resistance Fundamentals - Viral Escape Artists
- High Mutation Rate: Driven by an error-prone reverse transcriptase enzyme that lacks proofreading capability. This leads to frequent nucleotide misincorporations.
- Rapid Replication Cycle: HIV produces billions of virions daily, providing ample opportunity for mutations to arise.
- Viral Quasispecies: The combination of high mutation rates and rapid replication creates a diverse population of genetically distinct but related viral variants within a single patient.
- Selective Pressure: Antiretroviral therapy (ART) eliminates susceptible viruses, allowing pre-existing or newly mutated resistant strains to survive and become the dominant variant.
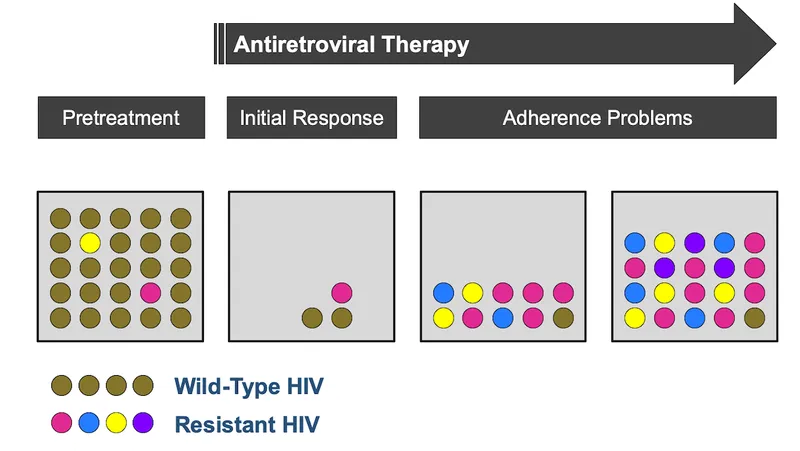
⭐ The M184V mutation, selected by lamivudine (3TC) or emtricitabine (FTC), confers high-level resistance to these NRTIs. However, it also impairs viral fitness and can paradoxically increase susceptibility to other agents like tenofovir (TDF) and zidovudine (AZT).
Mechanisms of Resistance - How They Dodge
Viral evasion occurs via genetic mutations in HIV genes, primarily pol, which codes for reverse transcriptase, protease, and integrase. Drug pressure selects for these resistant variants.
- Target Site Modification: The primary mechanism.
- NRTIs & NNRTIs: Mutations in the reverse transcriptase (RT) enzyme alter the drug binding site.
- NRTIs: Resistance requires accumulation of several mutations (e.g., Thymidine Analog Mutations - TAMs).
- NNRTIs: A single point mutation (e.g., K103N) can cause high-level resistance.
- Protease Inhibitors (PIs): Stepwise accumulation of mutations in the protease enzyme.
- Integrase Inhibitors (INSTIs): Mutations in the integrase enzyme.
- NRTIs & NNRTIs: Mutations in the reverse transcriptase (RT) enzyme alter the drug binding site.
⭐ High-Yield Fact: The K103N mutation is a classic non-nucleoside reverse transcriptase inhibitor (NNRTI) resistance mutation. It confers high-level resistance to first-generation NNRTIs like efavirenz and nevirapine, often from a single nucleotide change.
Resistance Testing - Reading the Resistance
- Two main types: Genotypic and Phenotypic assays.
- Genotypic Assays:
- Detects drug-resistance mutations in viral genes (e.g., pol gene).
- Faster, less expensive, and more commonly used for routine testing.
- Interpretation relies on databases correlating mutations with drug resistance.
- May not detect resistance from complex or novel mutation patterns.
- Phenotypic Assays:
- Measures viral growth in varying drug concentrations.
- Reports fold-change in drug concentration needed to inhibit viral replication by 50% ($IC_{50}$) vs. wild-type.
- Directly measures drug susceptibility but is slower and more expensive.
⭐ Perform resistance testing at entry into care (baseline) and at virologic failure to guide selection of a new, effective regimen.
Clinical Management - Switching the Strategy
When virologic failure occurs (HIV RNA > 200 copies/mL), a new antiretroviral (ART) regimen is required. The goal is re-suppression of viral load.
- First Step: Always perform genotypic resistance testing while the patient is on the failing regimen to identify mutations.
- Regimen Selection:
- Aim for at least two, preferably three, fully active drugs.
- Utilize drugs from a new class to which the virus is susceptible.
- Boosted protease inhibitors (PIs) and second-generation integrase inhibitors (INSTIs) often retain activity.
⭐ Core Principle: Never add a single active agent to a failing regimen. This practice encourages the development of further resistance, a concept known as sequential monotherapy.
High‑Yield Points - ⚡ Biggest Takeaways
- Antiretroviral resistance is a primary cause of treatment failure, driven by HIV's high mutation rate via error-prone reverse transcriptase.
- Poor adherence and suboptimal drug levels are the strongest predictors of resistance development.
- Key mutations include M184V (NRTIs like lamivudine), K103N (NNRTIs like efavirenz), and L90M (Protease Inhibitors).
- Genotypic resistance testing is crucial before starting therapy and after treatment failure to guide regimen selection.
- Combination ART (cART) is the cornerstone of prevention, creating a high genetic barrier to resistance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

