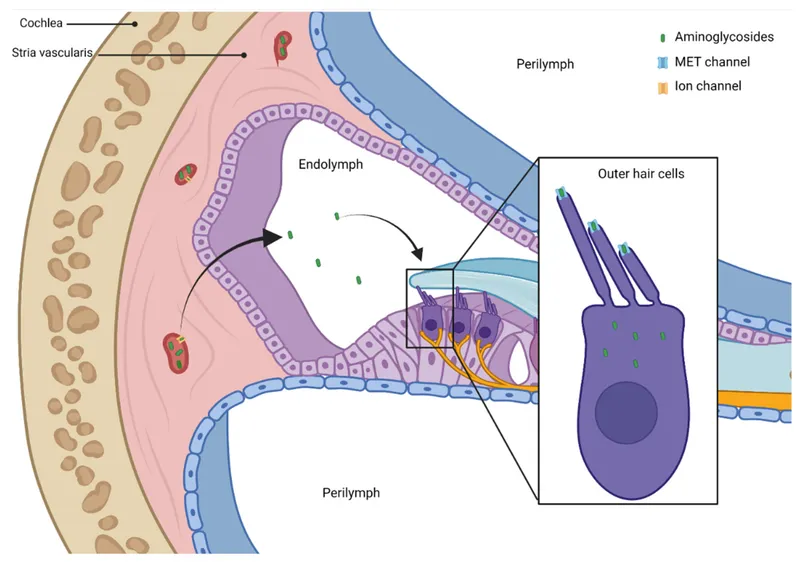
Nephro & Ototoxicity - Kidneys & Ears Under Siege
- Aminoglycosides (e.g., Gentamicin, Amikacin)
- Nephrotoxicity: Acute Tubular Necrosis (ATN). Usually reversible.
- Ototoxicity: Auditory (cochlear) & vestibular damage. Often irreversible. Monitor peak/trough levels.
- Vancomycin
- Nephrotoxicity: ATN, interstitial nephritis. Monitor trough levels (15-20 mg/L for severe infections).
- Ototoxicity: Rare, but risk ↑ with high doses or renal impairment.
- Amphotericin B
- Nephrotoxicity: Severe vasoconstriction & direct tubular damage (Distal RTA), leading to ↓K⁺, ↓Mg²⁺.
- Polymyxins (Colistin, Polymyxin B)
- Nephrotoxicity: Dose-dependent ATN.
⭐ Synergistic Toxicity: Risk of ototoxicity ↑ when aminoglycosides are co-administered with loop diuretics (e.g., furosemide). Nephrotoxicity risk ↑ with concurrent use of vancomycin, amphotericin B, or cyclosporine.
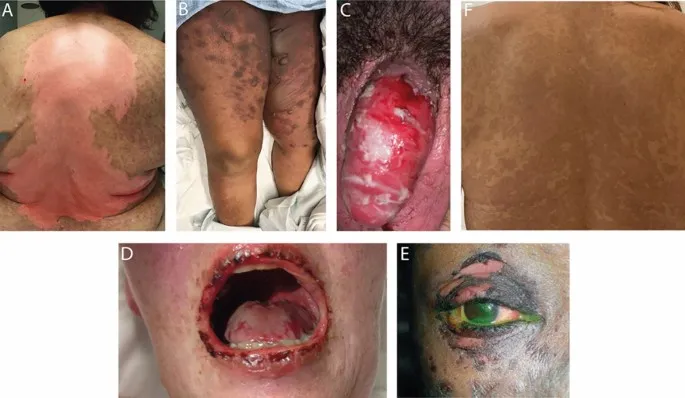
Systemic & Skin Reactions - The Great Rash
- Stevens-Johnson Syndrome (SJS) / Toxic Epidermal Necrolysis (TEN):
- Severe, blistering mucocutaneous reactions. Common triggers: Sulfa drugs, Allopurinol, Lamotrigine, Penicillins.
- Defined by % Body Surface Area (BSA) detachment: SJS <10%, SJS/TEN overlap 10-30%, TEN >30%.
- Positive Nikolsky's sign (skin sloughing with gentle pressure).
- DRESS Syndrome (Drug Reaction with Eosinophilia and Systemic Symptoms):
- Features: Fever, rash, facial edema, eosinophilia, atypical lymphocytes, internal organ (liver, kidney) involvement.
- Common culprits: Allopurinol, anticonvulsants.
⭐ DRESS syndrome has a characteristic long latency period, typically appearing 2-8 weeks after starting the offending drug.
Neuro & MSK Mayhem - Nerves, Bones & Groans
- Aminoglycosides: Ototoxicity (vestibular & cochlear damage), neuromuscular blockade.
- Fluoroquinolones: Tendon rupture (Achilles), cartilage damage. 📌 "FluoroquinoLONES hurt attachments to your BONES."
- Isoniazid (INH): Peripheral neuropathy (give with Vitamin B6/pyridoxine to prevent), seizures.
- Daptomycin: Myopathy, ↑ CPK levels (monitor weekly).
- Linezolid: Peripheral & optic neuropathy, serotonin syndrome.
- Metronidazole: Peripheral neuropathy, disulfiram-like reaction.
⭐ Fluoroquinolones have a black box warning for tendon rupture. The risk is highest in patients over 60, on corticosteroids, or with renal failure.
Heme & Hepatic Hits - Blood, Guts & Gall
-
Hematologic Toxicity:
- Chloramphenicol: Dose-related suppression (reversible); aplastic anemia (irreversible).
- Sulfonamides (TMP-SMX): Megaloblastic anemia, hemolysis in G6PD deficiency.
- Linezolid: Thrombocytopenia, pancytopenia with prolonged use.
- Zidovudine (NRTI): Myelosuppression → macrocytic anemia.
-
Hepatotoxicity:
- Isoniazid (INH): Age-dependent hepatitis. 📌 INH = Injures Neurons & Hepatocytes.
- Macrolides (Erythromycin): Acute cholestatic hepatitis.
- Antifungals (-azoles): General hepatotoxicity (monitor LFTs).
- Valproic Acid: Fatal hepatotoxicity (esp. in children).
⭐ Gray Baby Syndrome: Chloramphenicol toxicity in newborns lacking UDP-glucuronosyltransferase, leading to accumulation, shock, and death.
High‑Yield Points - ⚡ Biggest Takeaways
- Aminoglycosides (Gentamicin, Tobramycin) are notorious for nephrotoxicity and ototoxicity.
- Vancomycin infusion can cause Red Man Syndrome (a histamine-release reaction) and is also nephrotoxic.
- Daptomycin is associated with myopathy; monitor creatine phosphokinase (CPK) levels.
- Linezolid may cause bone marrow suppression (especially thrombocytopenia) and serotonin syndrome.
- Fluoroquinolones carry a risk of tendon rupture and cartilage damage.
- Clindamycin has a strong association with Clostridioides difficile colitis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

