Mechanism of Action - The Calcium Gatekeepers
- Primary Target: Inhibit voltage-gated L-type calcium channels in vascular smooth muscle and cardiac cells.
- Vascular Effect: ↓ intracellular $Ca^{2+}$ → smooth muscle relaxation → peripheral vasodilation → ↓ afterload.
- Cardiac Effect: ↓ intracellular $Ca^{2+}$ → ↓ myocardial contractility (negative inotropy) & ↓ sinoatrial/atrioventricular node activity (negative chronotropy/dromotropy).
⭐ Dihydropyridines (e.g., amlodipine) are more selective for vascular smooth muscle, while non-dihydropyridines (verapamil, diltiazem) also exert significant effects on the heart.
Classification - Two Sides of the Channel
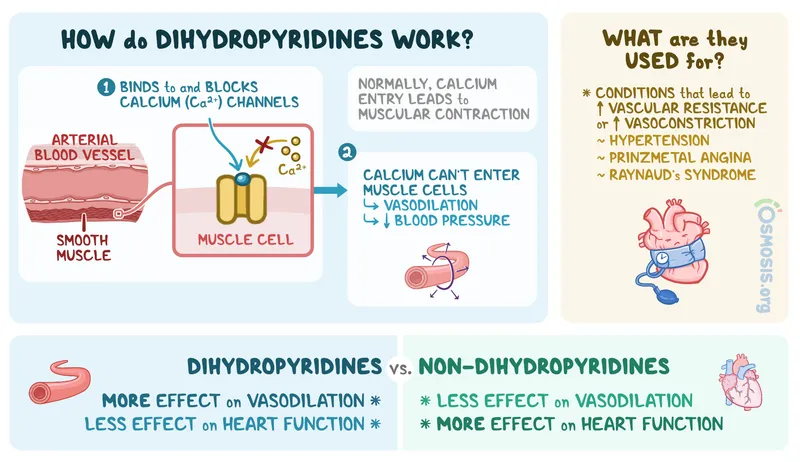
Calcium Channel Blockers (CCBs) are split into two major classes based on their primary site of action and chemical structure. This dictates their clinical use.
-
Dihydropyridines (DHPs):
- Act predominantly on arterial vascular smooth muscle.
- Potent vasodilators, leading to ↓ blood pressure.
- 📌 All generic names end in "-dipine".
-
Non-dihydropyridines (Non-DHPs):
- Greater effect on the myocardium.
- Act as negative inotropes (↓ contractility) and chronotropes (↓ heart rate).
- Verapamil has the strongest cardiac effect; Diltiazem is intermediate.
⭐ Because DHPs are potent vasodilators with minimal direct cardiac effect, they can cause a reflex tachycardia. This is a key physiological distinction from the bradycardic effect of non-DHPs.
Adverse Effects - The Unwanted Reactions
-
Dihydropyridines (Amlodipine, Nifedipine): Effects from potent vasodilation.
- Peripheral edema (ankles, pretibial)
- Flushing, headache, dizziness
- Reflex tachycardia
- Gingival hyperplasia
-
Non-Dihydropyridines (Verapamil, Diltiazem): Effects from cardiac suppression.
- Bradycardia & AV block (↑ PR interval)
- Worsening systolic heart failure (negative inotropy)
- Constipation (esp. Verapamil)
- Gingival hyperplasia
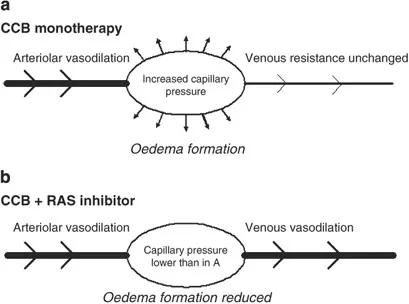
⭐ Dihydropyridine-induced edema results from precapillary arteriolar dilation, not fluid retention, and thus does not respond to diuretics.
Clinical Use - Choosing Your Blocker
-
Dihydropyridines (e.g., Amlodipine, Nifedipine): Primarily potent peripheral vasodilators.
- Ideal for: Isolated hypertension, Prinzmetal angina.
- Key side effects: Peripheral edema, reflex tachycardia, flushing.
-
Non-dihydropyridines (e.g., Verapamil, Diltiazem): Act on heart and blood vessels.
- Ideal for: Hypertension with co-existing atrial fibrillation (rate control), angina pectoris, migraine prophylaxis (Verapamil).
- ⚠️ Avoid in: HFrEF (Heart Failure with reduced Ejection Fraction) and AV block due to negative inotropic/chronotropic effects.
⭐ Nimodipine is a DHP that is highly lipid-soluble, crosses the blood-brain barrier, and is specifically used to prevent cerebral vasospasm after a subarachnoid hemorrhage.
High‑Yield Points - ⚡ Biggest Takeaways
- Dihydropyridines (e.g., amlodipine) are potent arterial vasodilators, mainly for hypertension; watch for peripheral edema and reflex tachycardia.
- Non-dihydropyridines (verapamil, diltiazem) act on the heart and blood vessels, treating hypertension, angina, and atrial fibrillation.
- Verapamil has the strongest cardiac depressant effect (negative inotropy/chronotropy).
- Key non-DHP side effects include constipation (especially verapamil), bradycardia, and AV block.
- Gingival hyperplasia is a classic side effect for all CCBs.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

