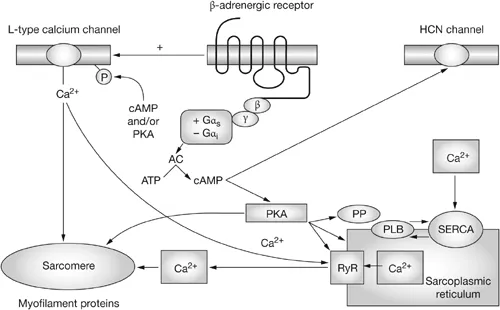
Mechanism of Action - The Beta Block Party
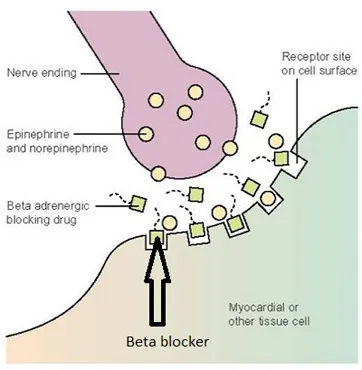
📌 By blocking β-adrenergic receptors, these drugs turn down the sympathetic nervous system's effects.
- Cardiac (β1): ↓ Heart rate (chronotropy), contractility (inotropy), and AV conduction (dromotropy) → ↓ Cardiac Output & O₂ demand.
- Renal (β1): ↓ Renin release from juxtaglomerular cells → ↓ RAAS activity.
⭐ Beta-blockers are proven to decrease mortality in patients post-myocardial infarction and in chronic heart failure with reduced ejection fraction (HFrEF).
Classification - The Selective Service
- Cardioselective (β1 Blockers): Primarily target β1 receptors in cardiac tissue, minimizing effects on the lungs (β2).
- Safer choice for patients with concomitant asthma or COPD.
- Drugs: Acebutolol, Atenolol, Betaxolol, Bisoprolol, Esmolol, Metoprolol, Nebivolol.
- 📌 Mnemonic: "A All Big Bulls Eat Meat Now."
- Non-selective (β1 & β2 Blockers): Block both receptor subtypes, affecting the heart, lungs, and other tissues.
- Drugs: Propranolol, Nadolol, Timolol, Pindolol.
- 📌 Mnemonic: "Please No Talking Please."
⭐ Acebutolol and Pindolol possess Intrinsic Sympathomimetic Activity (ISA), acting as partial agonists. This results in a smaller reduction in resting heart rate and cardiac output compared to other beta-blockers.
Indications - The Heart's Bodyguards
- Cardiovascular Shield:
- Ischemic Heart Disease: Stable angina, acute coronary syndrome (MI).
- Heart Failure: Stable, chronic systolic HF (HFrEF).
- Hypertension: Especially with compelling indications like IHD or HF.
- Tachyarrhythmias: Atrial fibrillation/flutter (rate control), SVTs.
- Beyond the Heart:
- Glaucoma (topical, e.g., Timolol).
- Hyperthyroidism (symptomatic relief).
- Essential Tremor & Migraine Prophylaxis.
⭐ In post-MI and HFrEF patients, beta-blockers (Carvedilol, Metoprolol Succinate, Bisoprolol) are proven to decrease mortality.
Adverse Effects & Contraindications - The Party Poopers
- Common AEs: Bradycardia, fatigue, depression, sexual dysfunction.
- Non-selective β-blockers: Can cause bronchospasm (β2 blockade).
- Contraindications: 📌 ABC
- Asthma & COPD (use β1-selective with caution)
- Bradycardia (<50 bpm) & Heart Block (2nd/3rd degree)
- Cocaine use & Cardiogenic shock (decompensated HF)
⭐ Non-selective β-blockers mask adrenergic symptoms of hypoglycemia (tachycardia, tremors), leaving only sweating. This is a critical consideration for diabetic patients on insulin or sulfonylureas.
Special Agents - Alpha/Beta & ISA
- Combined α/β-Blockers:
- Labetalol, Carvedilol: Provide non-selective β-blockade plus α1-blockade.
- This dual action adds peripheral vasodilation to standard beta-blocker effects.
- Uses: Labetalol for hypertensive emergencies; Carvedilol for chronic heart failure.
- Intrinsic Sympathomimetic Activity (ISA):
- Pindolol, Acebutolol are partial β-agonists.
- Cause less bradycardia and have milder metabolic side effects.
- ⚠️ Avoid in post-MI or angina patients.
⭐ Carvedilol is proven to reduce mortality in chronic HFrEF, partly due to its additional antioxidant and anti-inflammatory properties.
High‑Yield Points - ⚡ Biggest Takeaways
- Beta-blockers lower blood pressure by decreasing cardiac output, contractility, and renin release.
- Cardioselective (β1) blockers (e.g., Atenolol, Metoprolol) are preferred in patients with COPD/asthma.
- Non-selective (β1/β2) blockers (e.g., Propranolol) are contraindicated in asthma due to bronchoconstriction risk.
- Key side effects: bradycardia, AV block, fatigue, and masking hypoglycemia awareness.
- Labetalol and carvedilol have additional alpha-blocking properties, useful in hypertensive emergencies.
- Glucagon is the antidote for beta-blocker overdose.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

