Mechanisms of Action - How They Fight Fungi
Topical antifungals primarily disrupt the fungal cell membrane by targeting ergosterol, a key component absent in human cells.
-
Azoles (e.g., Miconazole, Clotrimazole):
- Inhibit lanosterol 14-α-demethylase, blocking the conversion of lanosterol to ergosterol.
-
Allylamines (Terbinafine) & Benzylamines (Butenafine):
- Inhibit squalene epoxidase, leading to the toxic accumulation of squalene.
-
Polyenes (Nystatin):
- Bind directly to ergosterol, forming pores in the membrane, causing leakage and cell death.
-
Other Mechanisms:
- Ciclopirox: Chelates trivalent cations (e.g., $Fe^{3+}$), inhibiting essential enzymes.
- Tavaborole: Inhibits leucyl-tRNA synthetase, blocking fungal protein synthesis.
⭐ While azoles are typically fungistatic (inhibit growth), allylamines and polyenes are generally fungicidal (kill fungi), a key difference for clinical application.
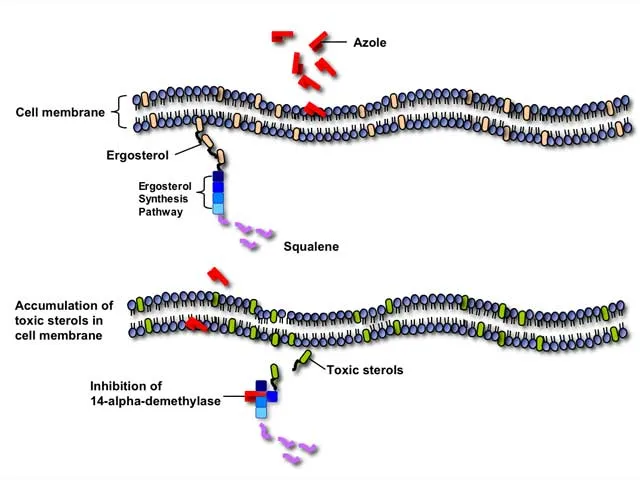
The Antifungal Arsenal - Key Drug Classes
-
Azoles (Imidazoles): Inhibit fungal P450 enzyme 14-α-demethylase, blocking ergosterol synthesis.
- Examples: Clotrimazole, Miconazole for tinea and cutaneous candidiasis. Ketoconazole for seborrheic dermatitis.
-
Polyenes: Bind directly to ergosterol, creating pores in the fungal cell membrane, leading to cell lysis.
- Example: Nystatin, primarily for Candida species.
-
Allylamines: Inhibit squalene epoxidase, a key enzyme in the ergosterol pathway, leading to toxic squalene accumulation.
- Examples: Terbinafine, Naftifine. Highly effective against dermatophytes.
⭐ Nystatin is not absorbed from the GI tract, making it ideal and safe for treating oral and esophageal candidiasis ("swish and swallow/spit").
Clinical Use - Matching Drug to Bug
- Dermatophytes (Trichophyton, Microsporum, Epidermophyton)
- Clinical: Tinea corporis (ringworm), tinea pedis (athlete's foot), tinea cruris (jock itch).
- Agents: Allylamines (Terbinafine, Naftifine) are highly effective. Azoles (Clotrimazole, Miconazole) are also common first-line choices. Butenafine is another option.
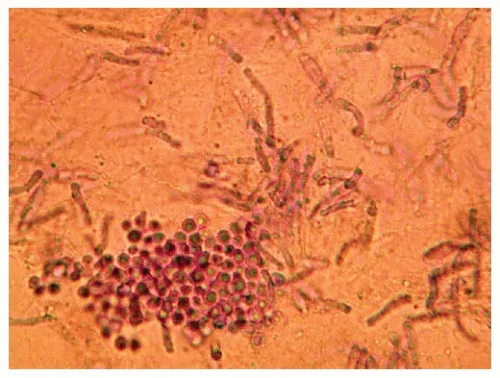
- Candida albicans
- Clinical: Intertrigo (skin folds), diaper dermatitis, mild oropharyngeal candidiasis (thrush).
- Agents: Nystatin suspension/cream (a polyene, specific for Candida). Topical Azoles are also effective.
- Malassezia spp. (formerly Pityrosporum)
- Clinical: Tinea versicolor (hypo/hyperpigmented macules), seborrheic dermatitis.
- Agents: Selenium sulfide, Ketoconazole shampoo, zinc pyrithione.
⭐ Terbinafine is fungicidal (inhibits squalene epoxidase), while azoles are fungistatic (inhibit 14-α-demethylase). This mechanistic difference is a classic, high-yield exam question.
Adverse Effects - The Not-So-Fun Side
- Common (Local): Generally well-tolerated.
- Irritation, burning, or stinging
- Erythema (redness)
- Pruritus (itching)
- Less Common:
- Allergic contact dermatitis: A true hypersensitivity requiring cessation.
- Hypopigmentation with azoles.
⭐ Tinea Incognito: Be cautious with combination creams containing corticosteroids; they can mask inflammation and alter the appearance of a fungal infection, leading to a delayed or incorrect diagnosis.
- Topical antifungals primarily treat superficial dermatophyte (tinea) and Candida infections.
- Azoles (clotrimazole, miconazole) inhibit ergosterol synthesis by blocking the enzyme 14-alpha-demethylase.
- Terbinafine, an allylamine, is fungicidal against dermatophytes by inhibiting squalene epoxidase.
- Nystatin, a polyene, binds to ergosterol to form pores in the fungal cell membrane; it is only effective against Candida.
- Ketoconazole shampoo is uniquely used for seborrheic dermatitis and tinea versicolor.
- Adverse effects are generally mild and limited to local skin irritation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

