Resistance Mechanisms - Fungi Fight Back
- Target Modification: The most common mechanism.
- Azoles: Point mutations in the ERG11 gene alter the target enzyme, 14-α-demethylase, reducing drug binding.
- Echinocandins: Mutations in FKS1/FKS2 genes change the structure of β-(1,3)-D-glucan synthase.
- Polyenes: Alterations in ERG genes reduce ergosterol in the cell membrane, decreasing Amphotericin B binding sites.
- Efflux Pumps: Overexpression of genes for ABC or MFS transporters actively pumps azoles out of the cell.
- Reduced Drug Access/Metabolism:
- Flucytosine: Impaired uptake (cytosine permease mutation) or decreased conversion to its active form (cytosine deaminase mutation).
⭐ Cross-resistance is a major clinical issue; a mutation conferring resistance to one azole often applies to others in the class.
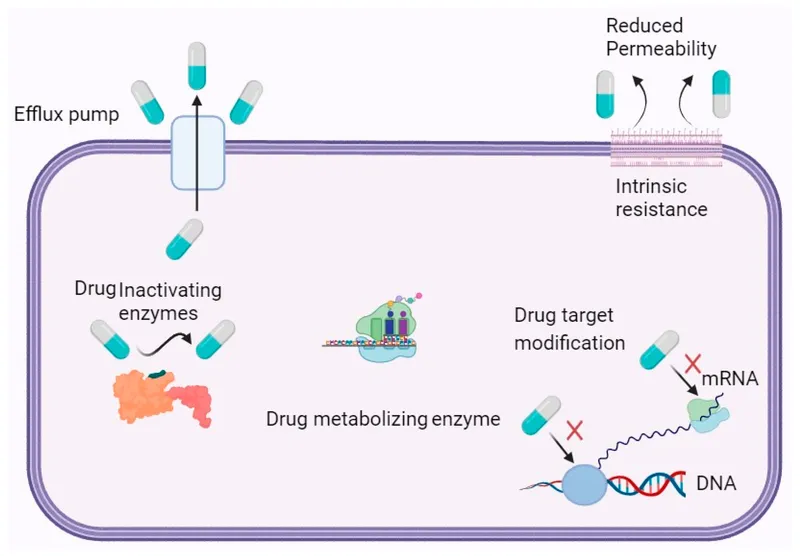
Target Alterations - Changing the Locks
Fungi evolve by modifying the drug's molecular target, akin to changing a lock. This prevents the drug "key" from fitting, rendering it ineffective. This is a primary resistance mechanism for several major antifungal classes, driven by specific genetic mutations.
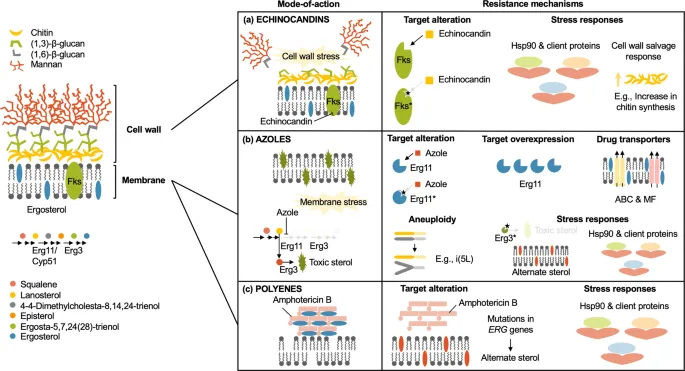
| Drug Class | Molecular Target | Resistance Gene(s) & Mechanism |
|---|---|---|
| Azoles | Lanosterol 14α-demethylase | Point mutations in ERG11 gene reduce drug binding. |
| Polyenes | Ergosterol | Altered membrane sterol composition (↓ ergosterol). |
| Echinocandins | β-(1,3)-D-glucan synthase | Mutations in FKS1 or FKS2 "hot spot" regions. |
| Flucytosine | Cytosine deaminase | Mutations in FCY1 gene cause loss of enzyme function. |
Drug Transport - Pump It or Block It
-
Efflux Pumps (Azoles): A primary mechanism of azole resistance.
- Transporter proteins actively expel drugs, preventing accumulation at the target enzyme, Erg11p.
- Key superfamilies: ATP-binding cassette (ABC) and Major Facilitator Superfamily (MFS).
- Caused by overexpression of genes like CDR1, CDR2 (ABC) and MDR1 (MFS).
- 📌 Mnemonic: ABC/MFS pumps Actively Boot Chemicals/Molecules From Site.
-
Decreased Drug Uptake (Flucytosine):
- Resistance to flucytosine ($5-FC$) often involves impaired drug entry.
- Mutations in the cytosine permease enzyme reduce $5-FC$ transport into the cell.
- This limits conversion to active toxic metabolites like 5-fluorouracil.
⭐ Upregulation of efflux pumps is a key reason Candida auris exhibits high-level, multidrug resistance, particularly to azoles.
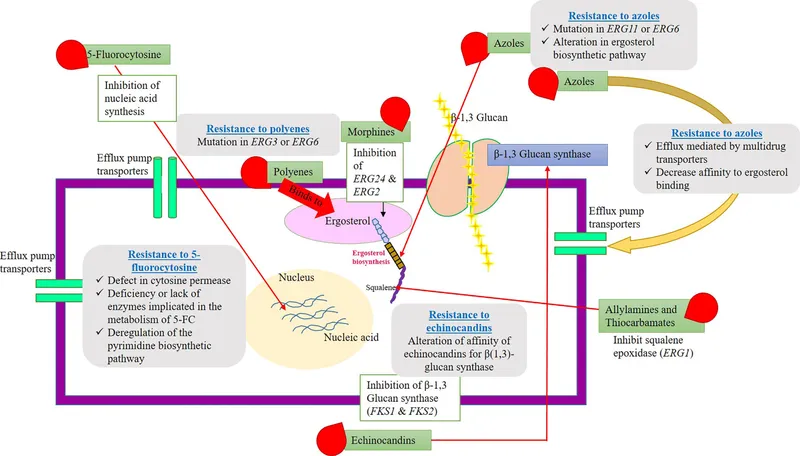
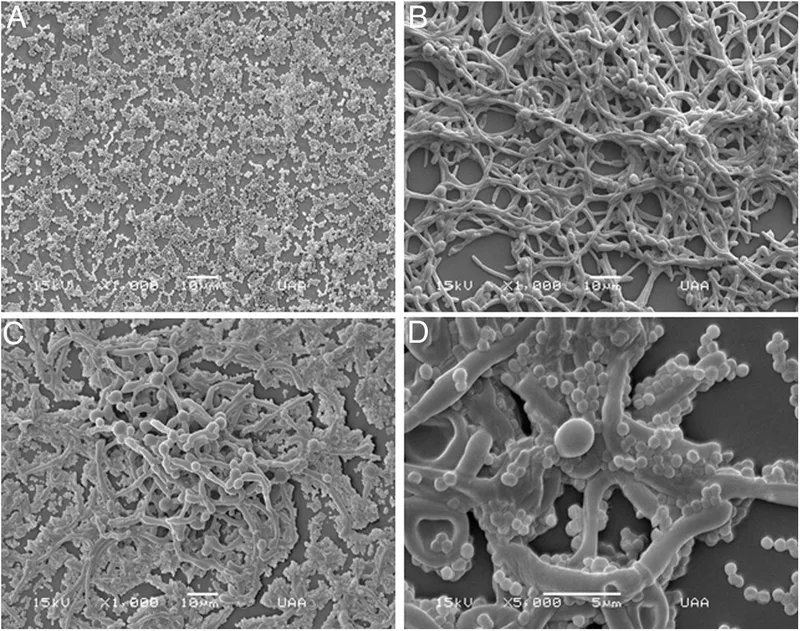
Biofilm Formation - Slime Shield Stronghold
- Fungi, especially Candida species, form biofilms on surfaces like catheters and implants.
- This creates a physical barrier composed of an extracellular matrix (ECM), rich in polysaccharides like β-glucan.
- The dense ECM physically traps antifungal agents, preventing them from reaching fungal cells.
- It also creates a protected, low-nutrient, and low-oxygen environment.
- Cells within the biofilm's deeper layers are often metabolically quiescent (persister cells), reducing the efficacy of drugs targeting active processes.
⭐ Biofilms significantly upregulate efflux pump expression, actively expelling any antifungal that penetrates the matrix, contributing to multi-drug resistance.
High-Yield Points - ⚡ Biggest Takeaways
- Azole resistance most often involves mutations in the ERG11 gene or the upregulation of drug efflux pumps.
- Polyene (Amphotericin B) resistance is linked to altered cell membrane ergosterol composition, which reduces drug binding.
- Echinocandin resistance typically results from mutations in the FKS1 gene, modifying the target enzyme β-(1,3)-D-glucan synthase.
- Flucytosine resistance occurs via decreased activity of cytosine permease or cytosine deaminase.
- Biofilm formation acts as a physical barrier, limiting drug penetration.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

