Indications for Prophylaxis - Fungal Gatekeepers
-
Hematologic Malignancy & HSCT
- Acute Myeloid Leukemia (AML) / Myelodysplastic Syndrome (MDS) induction chemotherapy.
- Allogeneic Hematopoietic Stem Cell Transplant (HSCT) with Graft-vs-Host Disease (GVHD).
- Prolonged neutropenia (ANC <500/mm³ for >7 days).
- Target: Candida, Aspergillus.
-
Solid Organ Transplant (SOT)
- High-risk liver, lung, or small bowel transplants.
- Risk factors: re-transplantation, surgical leaks, high immunosuppression.
- Target: Candida, Aspergillus.
-
HIV/AIDS
- Pneumocystis jirovecii (PJP): CD4 <200/mm³.
- Cryptococcus neoformans (secondary prophylaxis): CD4 <100/mm³.
⭐ In AML/MDS patients receiving induction chemotherapy, posaconazole prophylaxis has shown superior efficacy in preventing invasive fungal infections, particularly aspergillosis, compared to fluconazole or itraconazole.
The Antifungal Arsenal - Meet the Players
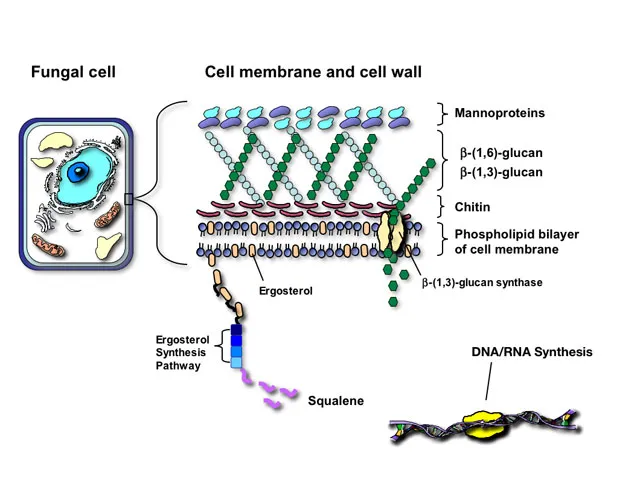
-
Polyenes (Amphotericin B, Nystatin)
- Mechanism: Binds to ergosterol → forms pores → cell lysis.
- Use: Broadest spectrum; severe, systemic mycoses.
- ⚠️ Toxicity: Nephrotoxicity, infusion reactions ("shake and bake").
-
Azoles (-conazoles)
- Mechanism: Inhibit fungal CYP450 (14-α-demethylase) → ↓ ergosterol synthesis.
- Use: Broad; Voriconazole for Aspergillus, Fluconazole for Candida.
-
Echinocandins (-fungins)
- Mechanism: Inhibit β-(1,3)-D-glucan synthesis → disrupt cell wall.
- Use: Invasive candidiasis (incl. azole-resistant), Aspergillus.
-
Flucytosine (5-FC)
- Mechanism: Converted to 5-FU → inhibits DNA/RNA synthesis.
- Use: Synergy with Ampho B for cryptococcal meningitis.
- ⚠️ Toxicity: Myelosuppression.
⭐ High-Yield: Azoles are potent inhibitors of human cytochrome P450 enzymes, increasing levels of drugs like warfarin and statins.
Prophylaxis Playbook - The Right Drug, Right Patient
- Goal: Prevent invasive fungal infections (IFIs) in high-risk patients.
- Selection depends on: patient's immune status, local epidemiology, and expected fungal pathogens.
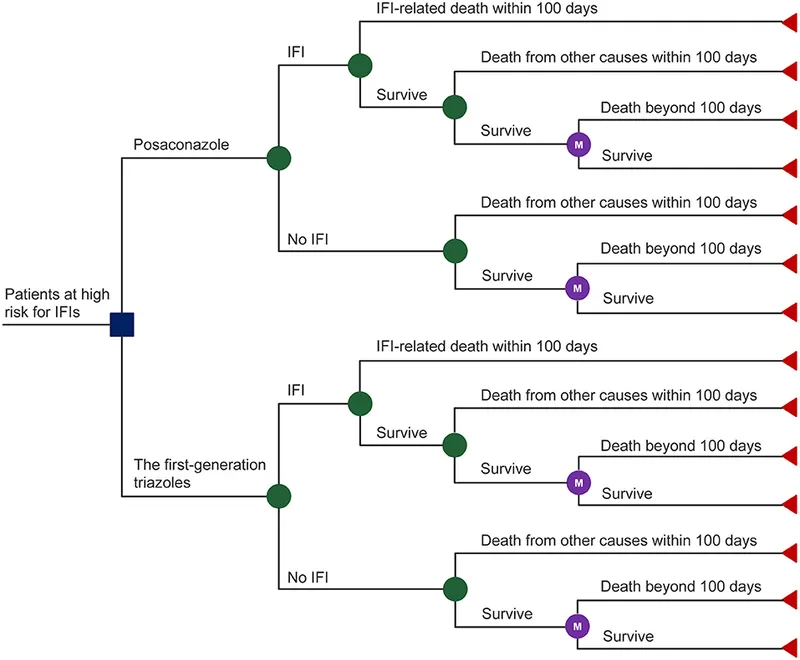
⭐ Exam Favorite: Posaconazole is the preferred agent for prophylaxis in patients with prolonged neutropenia and for allogeneic hematopoietic stem cell transplant (HSCT) recipients with graft-versus-host disease (GVHD) due to its superior activity against molds like Aspergillus.
High‑Yield Points - ⚡ Biggest Takeaways
- Neutropenic patients often receive fluconazole or an echinocandin (e.g., caspofungin).
- HIV/AIDS patients with CD4 < 100 require fluconazole for Cryptococcus prophylaxis.
- Transplant recipients (stem cell, solid organ) need broad coverage, often with posaconazole or voriconazole.
- Candida prophylaxis with fluconazole is crucial for high-risk ICU patients.
- Remember PJP/PCP prophylaxis (CD4 < 200) is TMP-SMX, not a primary antifungal.
- Azoles exhibit significant drug-drug interactions via CYP450 inhibition.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

