Etiology & Risks - The Usual Suspects
- Primary Culprit: Uropathogenic E. coli (UPEC) causes >85% of cases.
- Other Pathogens: Klebsiella, Proteus (↑ urine pH, stones), Enterococcus, S. saprophyticus (adolescent girls).
- Key Risk Factors:
- Anatomic: Vesicoureteral Reflux (VUR), Posterior Urethral Valves (PUV), phimosis in uncircumcised boys <1 yr.
- Functional: Bladder & Bowel Dysfunction (BBD), constipation.
⭐ In children with recurrent febrile UTIs, the prevalence of Vesicoureteral Reflux (VUR) can be as high as 30-40%.
Clinical Clues - Age is Key
- Neonates (<1 mo): Non-specific signs rule. Presents like sepsis: fever/hypothermia, jaundice, poor feeding, lethargy.
- Infants (1-24 mo): Fever is often the only sign. Suspect with irritability, vomiting, poor weight gain.
- Toddlers/Preschool (2-5 yrs): More specific symptoms appear. Abdominal pain, dysuria, frequency, foul-smelling urine.
- School-Aged (>5 yrs): Classic adult-like picture. Dysuria, frequency, urgency, suprapubic pain. Flank pain suggests pyelonephritis.
⭐ In children < 2 years, any fever without a clear source warrants a urine examination to rule out UTI.
Diagnosis - Confirm the Culprit
-
Urine Sample Collection: Method depends on age & toilet-training status.
- Gold Standard (Most sterile): Suprapubic Aspiration (SPA).
- Best practical method: Urethral Catheterization.
- Toilet-trained children: Mid-stream clean-catch urine (MSU).
- Screening ONLY: Urine bag. High contamination rate; a negative result is useful, but a positive result requires confirmation with a better sample.
-
Urinalysis:
- Dipstick: Positive Leukocyte Esterase (LE) for pyuria & Nitrites for Enterobacteriaceae.
- Microscopy: Pyuria (>5 WBCs/hpf) & Bacteriuria.
⭐ A combination of positive Leukocyte Esterase AND Nitrites on dipstick is highly suggestive of UTI.
- Urine Culture & Sensitivity: Gold standard for diagnosis.
Management & Imaging - The Action Plan
-
Initial Management (Empiric): Based on age & severity.
- < 3 months: Hospitalize & give IV antibiotics (Ceftriaxone or Cefotaxime + Amikacin).
- > 3 months (Toxic): Hospitalize & IV antibiotics.
- > 3 months (Non-toxic): Oral antibiotics (Cefixime, Amoxiclav) for 7-14 days.
-
Imaging Protocol: To detect renal scarring & VUR.
- Ultrasound (USG): For ALL children with their first febrile UTI.
- MCU (VCUG): If USG is abnormal, atypical UTI, or recurrent UTI.
- DMSA Scan: Gold standard for renal cortical defects (scarring). Done 4-6 months after acute infection.
⭐ High-Yield: A DMSA scan is the most sensitive imaging modality for detecting acute pyelonephritis and subsequent renal scarring. It should be performed 4-6 months after the UTI episode to differentiate acute changes from permanent scars.
High‑Yield Points - ⚡ Biggest Takeaways
- E. coli is the most common causative organism in pediatric UTIs.
- The gold standard for diagnosis is a urine culture; suprapubic aspiration is the most accurate collection method in infants.
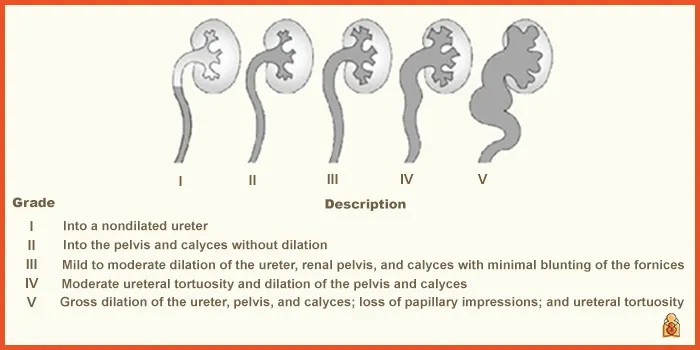
- MCU/VCUG is the investigation of choice to detect Vesicoureteral Reflux (VUR), the most common predisposing factor.
- A DMSA scan, performed 4-6 months post-infection, is the best test for identifying renal scarring.
- Infants < 2 months with a febrile UTI require hospitalization and IV antibiotics.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

