Transmission & PPTCT - The Unwanted Inheritance
- Vertical Transmission: Accounts for >90% of pediatric cases.
- In-utero (placental): ~25-35% of transmission.
- Intra-partum (delivery): ~60-70%; highest risk.
- Post-partum (breastfeeding): ~10-15% risk.
- Major Risk Factor: High maternal plasma viral load (>1000 copies/mL).
⭐ The majority of mother-to-child HIV transmission occurs during the intra-partum period (delivery).
Diagnosis - Spotting the Stowaway
-
Antibody Tests (ELISA/Western Blot): Unreliable for diagnosis in infants < 18 months. Transplacental maternal IgG antibodies persist, causing false-positive results. An antibody test at 18 months helps confirm final HIV-negative status.
-
Virological Assays (Gold Standard): HIV DNA PCR is the definitive method. It detects proviral DNA within the infant's own cells, enabling Early Infant Diagnosis (EID).
⭐ A single positive virological test is insufficient for diagnosis. A confirmatory repeat test on a new blood sample is mandatory to finalize the diagnosis of HIV infection.
- Diagnostic Algorithm:
Clinical Features & Staging - The Symptom Medley
- WHO Clinical Staging: A progressive spectrum from mild to severe.
- Stage 1: Asymptomatic or Persistent Generalized Lymphadenopathy (PGL).
- Stage 2: Unexplained hepatosplenomegaly, papular pruritic eruptions, recurrent URIs.
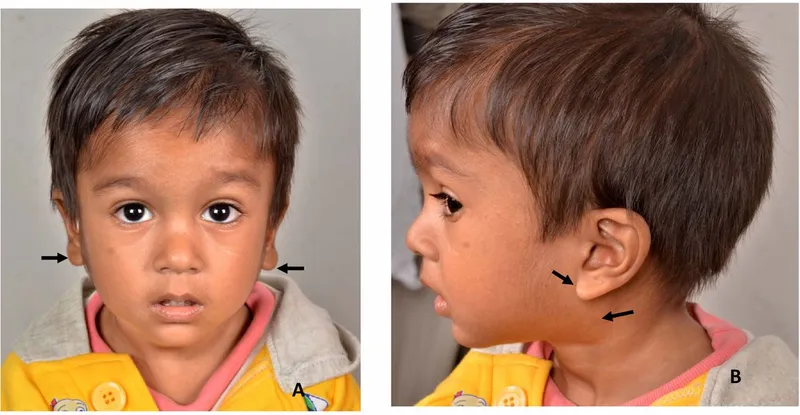
⭐ Painless, bilateral parotid gland enlargement is a highly characteristic early sign.
- Stage 3: Moderate malnutrition, oral hairy leukoplakia, Lymphoid Interstitial Pneumonitis (LIP), pulmonary TB.
- Stage 4 (AIDS-defining): Severe wasting/stunting, Pneumocystis jirovecii pneumonia (PJP), recurrent severe bacterial infections (≥2/year), CMV retinitis.
Management & ART - Fighting Back Early
-
Goals: Suppress viral replication (↓VL), restore immune function (↑CD4), reduce morbidity & mortality.
-
Initiation (NACO): Treat All! Initiate ART for all children with HIV, regardless of WHO stage or CD4 count.
-
First-Line ART Regimens:
- < 3 years: Abacavir (ABC) + Lamivudine (3TC) + Lopinavir/r (LPV/r).
- > 3 years: ABC + 3TC + Dolutegravir (DTG).
- > 10 years (>35kg): Tenofovir (TDF) + 3TC + DTG.
-
Second-Line ART: Guided by resistance testing after first-line failure. Involves switching to a new drug class.
-
PJP Prophylaxis (Co-trimoxazole):
- Start for ALL HIV-exposed infants at 4-6 weeks of age.
- Continue until HIV infection is reliably excluded.
⭐ All infants born to HIV+ mothers receive ART prophylaxis at birth (e.g., Nevirapine) and MUST start Co-trimoxazole prophylaxis at 6 weeks of age.
High‑Yield Points - ⚡ Biggest Takeaways
- Vertical transmission is the most common route of infection in children.
- HIV DNA PCR is the diagnostic test of choice for infants <18 months.
- CD4 counts are physiologically higher in children; use age-specific percentages for staging.
- PJP prophylaxis with Cotrimoxazole is critical, started at 4-6 weeks of age.
- Lifelong ART is recommended for all HIV-infected children, irrespective of clinical or immunological stage.
- Live vaccines (MMR, Varicella) can be given if the child has a CD4 count >15%.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

