Definition & Cutoffs - Sizing Up the Situation
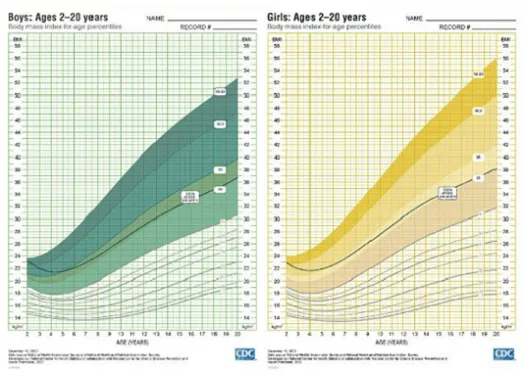
- Core Metric: Body Mass Index (BMI) for age and sex, plotted on appropriate growth charts.
- IAP / CDC Percentile Cutoffs:
- Underweight: < 5th percentile
- Normal Weight: 5th to < 85th percentile
- Overweight: 85th to < 95th percentile
- Obesity: ≥ 95th percentile
- Severe Obesity: ≥ 120% of the 95th percentile or BMI ≥ 35 kg/m².
- WHO Z-Score Cutoffs (< 5 years):
- Overweight: Weight-for-height > +2 SD
- Obesity: Weight-for-height > +3 SD
⭐ A child with obesity at age 6 has a >50% chance of being obese as an adult, rising to 80% for an obese adolescent.
Etiology & Risks - The Why Behind the Weight
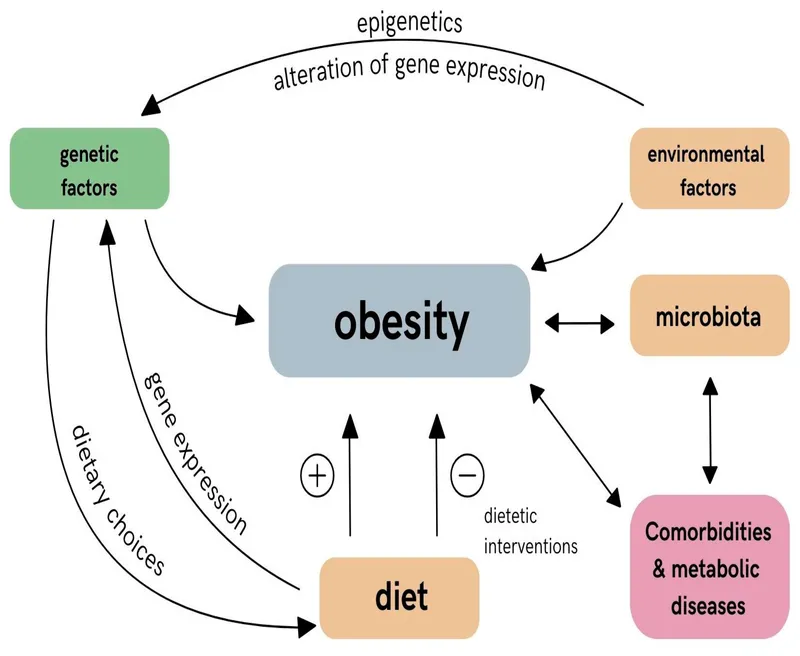
- Polygenic & Syndromic:
- Strong genetic predisposition; risk is >80% if both parents are obese.
- Syndromes: Prader-Willi, Bardet-Biedl, Cohen syndrome.
- Lifestyle & Environment:
- Diet: ↑ intake of energy-dense foods, sugary beverages (SSBs).
- Activity: ↓ physical activity, ↑ sedentary time (screen time >2 hrs/day).
- Perinatal Factors:
- Maternal obesity, Gestational Diabetes (GDM).
- High birth weight (>4 kg), rapid infant weight gain.
⭐ A child with one obese parent has a 40% risk of obesity; this jumps to 80% if both parents are obese.
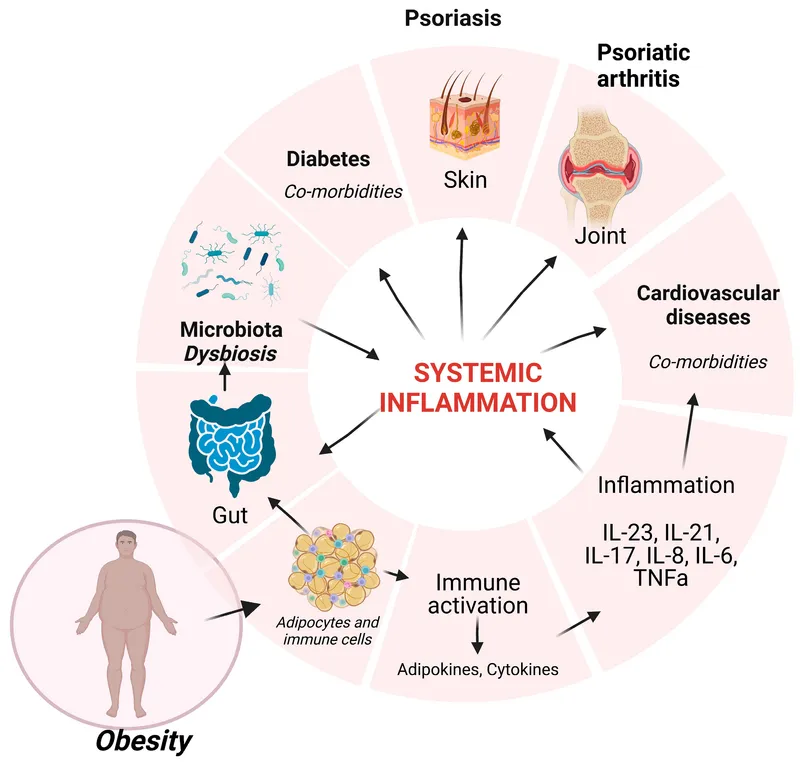
Complications - The Health Toll
- Metabolic/Endocrine
- Insulin Resistance → Type 2 Diabetes Mellitus
- Dyslipidemia (↑ Triglycerides, ↓ HDL)
- Precocious puberty, Polycystic Ovary Syndrome (PCOS) in girls
- Gastrointestinal
- Non-alcoholic fatty liver disease (NAFLD) → NASH → Cirrhosis
- Cholelithiasis (gallstones)
- Musculoskeletal
- Slipped Capital Femoral Epiphysis (SCFE)
- Blount's Disease (Tibia vara)
- Flat feet, musculoskeletal pain
- Cardio-Respiratory
- Hypertension
- Obstructive Sleep Apnea (OSA)
- Asthma exacerbation
- Neurological
- Idiopathic Intracranial Hypertension (Pseudotumor cerebri)
- Psychological
- Depression, anxiety, low self-esteem & social isolation
⭐ Childhood obesity is the most significant predictor of adult obesity, with >80% of obese adolescents becoming obese adults, carrying forward all associated health risks.
Management - The Action Plan
Management follows a staged, escalating process focused on family-centered behavioral changes. The primary goal is not rapid weight loss but achieving healthy eating and activity patterns, allowing the child to "grow into" a healthy weight over time.
📌 Mnemonic: 5-2-1-0 Rule for Healthy Habits
- 5 servings of fruits & vegetables daily
- 2 hours or less of screen time
- 1 hour or more of physical activity
- 0 sugary drinks
⭐ Pharmacotherapy (e.g., Orlistat for >12 yrs) is considered for BMI >95th percentile if lifestyle changes fail after 6-12 months. Bariatric surgery is reserved for severe adolescent obesity (BMI >40 or >35 with comorbidities).
High‑Yield Points - ⚡ Biggest Takeaways
- Childhood obesity is defined as a BMI ≥ 95th percentile for age and sex; overweight is BMI ≥ 85th percentile.
- Universal screening is recommended starting from 2 years of age.
- The most common cause is exogenous obesity (simple obesity) from caloric imbalance.
- Key complications include Type 2 Diabetes, hypertension, dyslipidemia, NAFLD, and slipped capital femoral epiphysis (SCFE).
- Consider syndromic causes like Prader-Willi or Bardet-Biedl syndrome with associated features.
- Lifestyle modification is the cornerstone of management.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

