Initial Clues - Spotting the Suspects
- History is Key: Unexplained & persistent symptoms are red flags.
- Bone pain (especially nocturnal), persistent headaches (worse in AM, with vomiting), limp.
- Easy bruising, recurrent infections.
- Clinical Examination Findings:
- General: Pallor, petechiae, purpura (suggests bone marrow infiltration).
- Abdomen: Palpable mass (Wilms', Neuroblastoma).
- Nodes: Firm, non-tender, matted lymphadenopathy.
- Neuro: Cranial nerve palsies, ataxia.
- Constitutional "B" Symptoms:
- Unexplained fever >38°C, drenching night sweats, unexplained weight loss >10% in 6 months.
⭐ Neuroblastoma can present with opsoclonus-myoclonus syndrome (“dancing eyes, dancing feet”), a paraneoplastic syndrome.
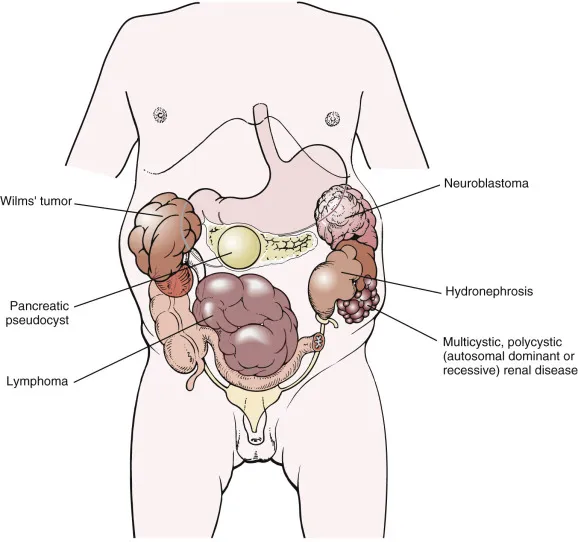
Lab Sleuthing - Blood & Marrow
- Complete Blood Count (CBC) & Peripheral Smear:
- Initial screen revealing potential cytopenias (anemia, thrombocytopenia) or leukocytosis with blasts.
- Serum Tumor Markers:
- LDH & Uric Acid: ↑ in high cell turnover (leukemia, lymphoma).
- VMA/HVA (urine): ↑ in Neuroblastoma.
- AFP / β-hCG: ↑ in Germ Cell Tumors, Hepatoblastoma.
- Bone Marrow Aspiration & Biopsy:
- Cornerstone for leukemia diagnosis; also used for staging lymphoma and neuroblastoma.
- A "dry tap" on aspiration suggests marrow packing (leukemia, fibrosis) or aplasia.
⭐ WHO Diagnosis: Presence of >20% blasts in bone marrow or peripheral blood confirms Acute Leukemia.
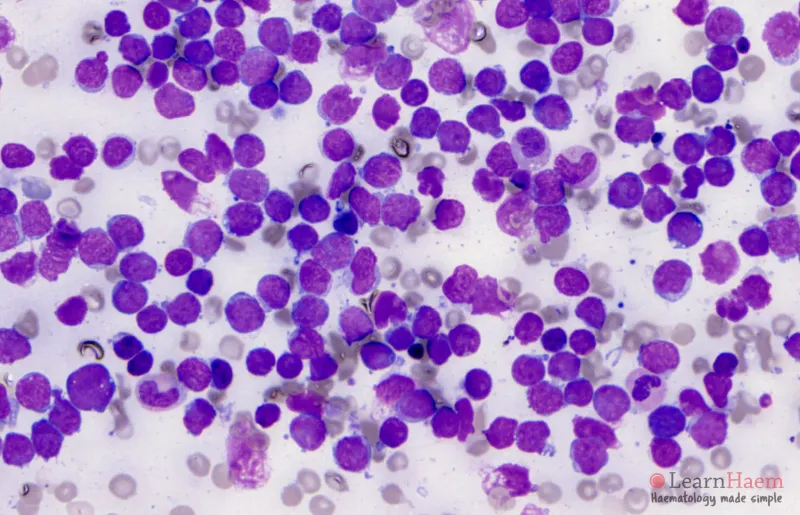
Imaging - The Inner View
-
First-Line Imaging:
- X-ray: Initial step for bone tumors (e.g., sunburst in osteosarcoma, onion-peel in Ewing's) and chest masses.
- Ultrasound: Differentiates solid vs. cystic lesions. Primary tool for abdominal masses like Wilms' tumor and neuroblastoma.
-
Advanced Cross-Sectional Imaging:
- CT Scan: Details chest, abdomen, pelvis for staging lymphomas & neuroblastomas. Balance diagnostic yield with radiation risk.
- MRI: Modality of choice for CNS tumors and soft-tissue sarcomas due to superior contrast and no radiation.
-
Functional/Metabolic Imaging:
- FDG-PET/CT: For staging, assessing treatment response, and detecting recurrence in lymphomas & sarcomas.
- MIBG Scan: Highly specific for neuroblastoma.
⭐ MIBG (metaiodobenzylguanidine) scan is the investigation of choice for staging neuroblastoma, showing uptake in over 90% of tumors.
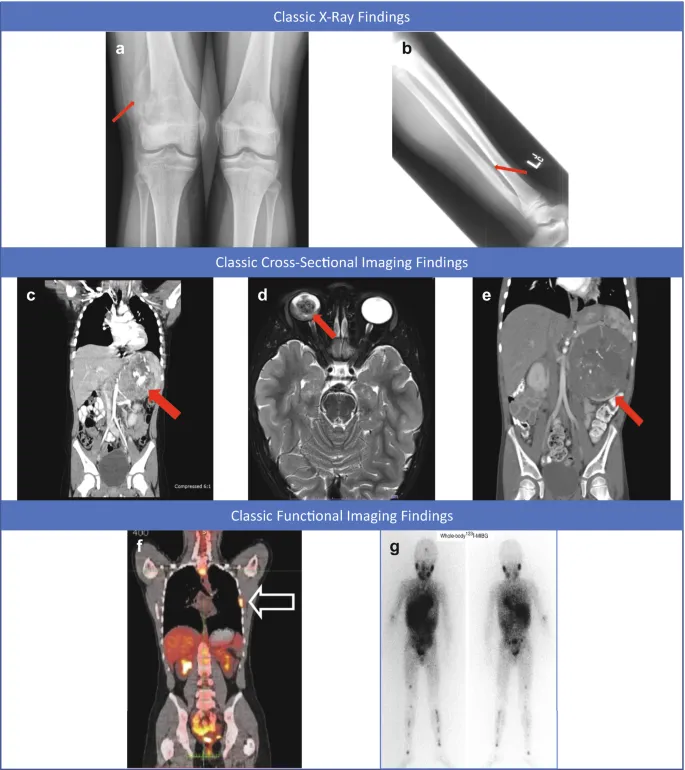
Tissue is the Issue - Biopsy & Markers
-
Biopsy: The Gold Standard
- Provides definitive histologic diagnosis, grading, and tissue for molecular/genetic analysis.
- Types: Excisional (small, accessible tumors), Incisional/Core Needle (large masses), Bone Marrow Aspirate & Biopsy (leukemia/lymphoma/staging).
-
Key Tumor Markers & Immunohistochemistry (IHC)
- Neuroblastoma: ↑ Urine VMA/HVA, serum NSE, Ferritin. IHC: Synaptophysin, Chromogranin A.
- Wilms' Tumor: IHC: WT1.
- Ewing Sarcoma: IHC: CD99, FLI1.
- Rhabdomyosarcoma: IHC: Desmin, Myogenin.
- Hepatoblastoma: ↑ AFP.
- Germ Cell Tumors: ↑ AFP, β-hCG.
⭐ Small Round Blue Cell Tumors (SRBCTs) have significant overlap. A panel of markers is crucial. Ewing Sarcoma is classically CD99 positive, while Rhabdomyosarcoma is Myogenin/Desmin positive.
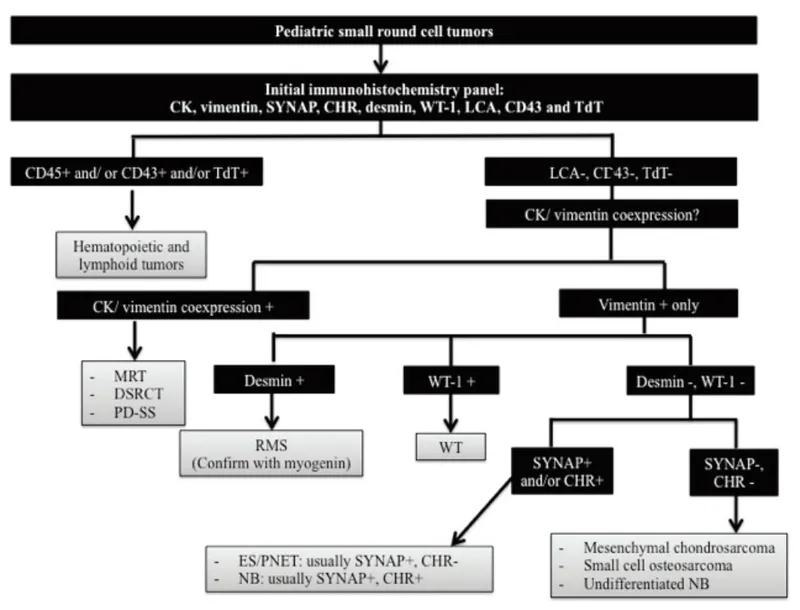
High‑Yield Points - ⚡ Biggest Takeaways
- Histopathology (HPE) & Immunohistochemistry (IHC) are the gold standard for diagnosis.
- Key tumor markers: AFP (yolk sac), β-hCG (germ cell tumors), and urinary VMA/HVA (neuroblastoma).
- MRI is preferred for CNS and soft tissue tumors; PET-CT is crucial for staging.
- Bone marrow aspiration & biopsy are mandatory for suspected leukemia and lymphoma.
- Molecular markers like N-myc amplification in neuroblastoma are critical for prognosis.
- Always consider age: Neuroblastoma in infants, Wilms' tumor in toddlers, sarcomas in adolescents.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

