Pain Assessment - Gauging the Hurt
- Core Principle: Pain is subjective; always believe the patient's self-report.
- Standard Tools:
- Numeric Rating Scale (NRS): Patient rates pain 0-10. Preferred for verbal adults.
- Wong-Baker FACES Pain Rating Scale: For children or adults with communication barriers.
- PAINAD Scale: For advanced dementia (assesses Breathing, Vocalization, Facial Expression, Body Language, Consolability).

⭐ High-Yield: In non-verbal patients, look for grimacing, moaning, restlessness, or guarding. Family input is crucial for establishing a baseline.
Pharmacologic Principles - The Right Tools
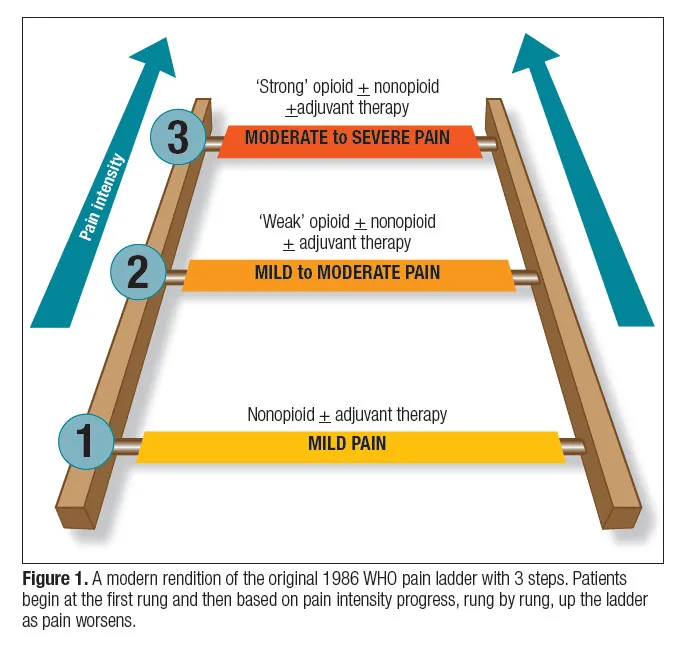
- Foundation: Utilize the WHO 3-step analgesic ladder for a structured approach to pain management.
- Opioid Selection:
- Morphine: Gold standard for severe pain; multiple formulations available.
- Fentanyl: Safe in renal failure; transdermal patch for stable, chronic pain.
- Hydromorphone: Potent, effective alternative to morphine.
- Adjuvant Analgesics:
- Neuropathic pain: Gabapentin, pregabalin, TCAs.
- Bone pain: Corticosteroids, NSAIDs.
- Side Effect Management:
- 📌 Mush & Push: Always prescribe a stimulant laxative (senna) + stool softener (docusate) for opioid-induced constipation.
⭐ The Principle of Double Effect ethically permits using high-dose opioids to relieve suffering, even if the medication unintentionally hastens death. The clinician's primary intent is crucial.
Opioid Management - The Heavy Lifters
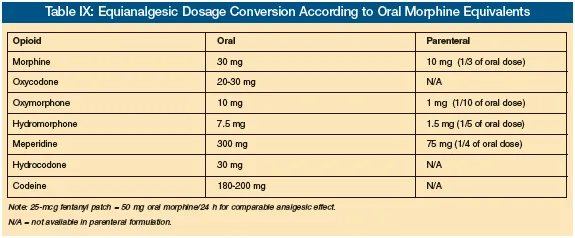
- Initiation: Start with short-acting opioids (e.g., morphine, hydromorphone).
- Opioid-naïve: Morphine 2.5-5 mg PO q4h.
- Adjust based on prior opioid use and comorbidities (renal/hepatic).
- Titration: For persistent pain, ↑ total daily dose by 25-50% until pain is controlled.
- Breakthrough Pain: Offer a rescue dose of 10-15% of the total 24-hour baseline opioid dose, q1-2h PRN.
- Side Effect Prophylaxis:
- Constipation: Universal. Start stimulant laxative (Senna) + stool softener. 📌 "Mush and Push."
- Nausea/Vomiting: Often transient. Consider antiemetics (e.g., haloperidol, metoclopramide).
- Sedation/Delirium: Usually resolves. If persistent, consider dose reduction or opioid rotation.
⭐ Principle of Double Effect: It is ethically permissible to use high-dose opioids to relieve pain, even if it may unintentionally hasten death, as the primary intention is palliation.
Adjuvant Analgesics - The Helpful Sidekicks
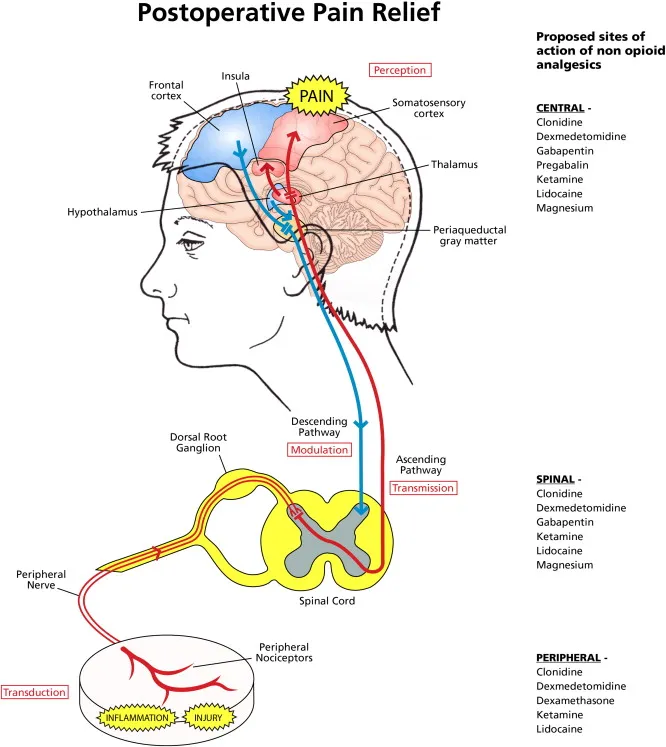
- Purpose: Enhance opioid analgesia, manage specific pain types (e.g., neuropathic), and reduce opioid-related side effects.
- Neuropathic Pain:
- First-line: Gabapentinoids (Gabapentin, Pregabalin), TCAs (Amitriptyline), or SNRIs (Duloxetine).
- Consider patient comorbidities and side effect profiles.
- Bone Pain / Nerve Compression:
- Corticosteroids (Dexamethasone) are effective for inflammatory or compressive pain.
- Refractory Pain:
- Ketamine (NMDA antagonist) for severe, opioid-resistant pain under specialist supervision.
⭐ For neuropathic pain, gabapentinoids are often preferred over TCAs in older adults due to a more favorable side-effect profile (less anticholinergic, sedative, and cardiac effects).
Ethical Considerations - Doctrine of Double Effect
- A principle that permits an action with both a good effect (intended) and a bad effect (foreseen but unintended).
- Justifies aggressive pain management (e.g., high-dose opioids) at the end of life, even if it may hasten death.
- Key Conditions:
- Intent is to alleviate pain, not to cause death.
- The good effect (analgesia) outweighs the bad effect (potential respiratory depression).
⭐ The doctrine of double effect is ethically and legally distinct from euthanasia, where the primary intention is to end the patient's life.
- Pain is subjective and what the patient says it is; use a validated pain scale.
- Opioids are first-line for moderate-to-severe pain; morphine is the gold standard.
- There is no ceiling dose for opioids in end-of-life care; titrate to pain relief.
- Always prophylax for constipation with a stimulant laxative.
- The Doctrine of Double Effect ethically justifies providing high-dose opioids for pain relief.
- Consider adjuvant analgesics like corticosteroids for bone pain or gabapentin for neuropathic pain.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

