Glomerular Anatomy - The Kidney's Sieve
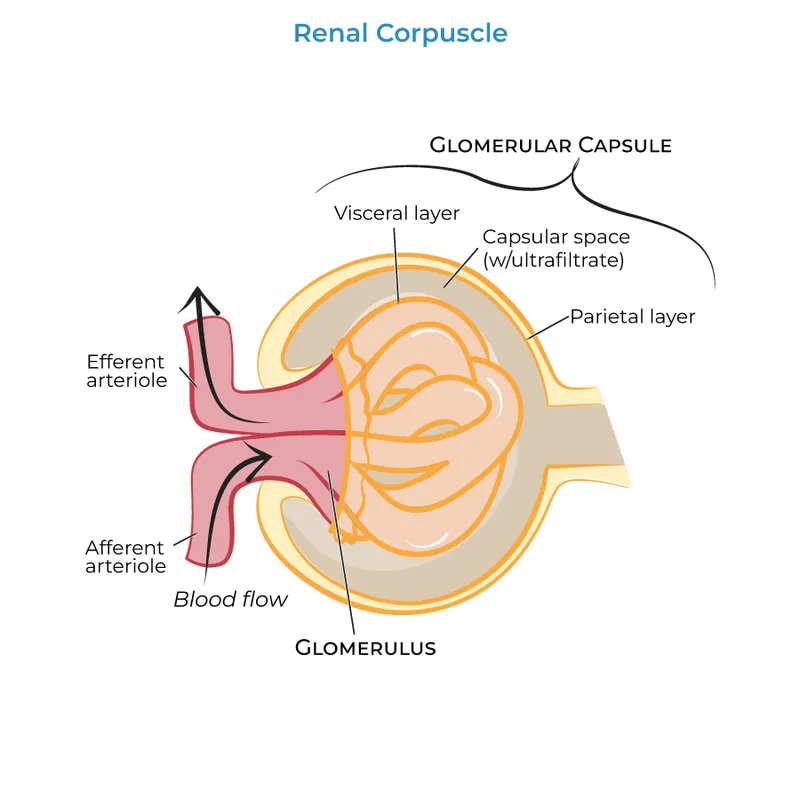
- Glomerular Filtration Barrier (GFB): A three-layered sieve controlling passage from blood to urine.
- 1. Fenestrated Capillary Endothelium: First layer; blocks cells but allows plasma through.
- 2. Glomerular Basement Membrane (GBM): Middle layer; with Type IV collagen and negatively charged heparan sulfate.
- 3. Podocyte Foot Processes: Outer layer with slit diaphragms between them.
- Selective Permeability:
- Size Barrier: Prevents passage of molecules > 70 kDa.
- Charge Barrier: Anionic heparan sulfate in the GBM repels negatively charged molecules like albumin.
⭐ High-Yield Fact: Podocyte effacement (flattening of foot processes) is the characteristic finding in Minimal Change Disease, leading to selective albuminuria.
Nephritic vs. Nephrotic - A Clinical Duel
-
Nephritic Syndrome: "Inflammation"
- Pathophysiology: Immune complex deposition → glomerular inflammation (hypercellularity).
- Hallmarks: Hematuria (dysmorphic RBCs, RBC casts) & Azotemia (↑ BUN/Cr).
- Clinical: Abrupt onset of oliguria, hypertension, and mild periorbital edema from salt/water retention.
- Proteinuria: Mild to moderate, always < 3.5 g/day.
-
Nephrotic Syndrome: "Podocyte Damage"
- Pathophysiology: Podocyte effacement → loss of negative charge barrier → massive protein leak.
- Hallmarks: Heavy proteinuria (> 3.5 g/day) & severe hypoalbuminemia (< 3.0 g/dL).
- Clinical: Insidious onset of anasarca (pitting edema, ascites), hyperlipidemia (fatty casts, oval fat bodies), and frothy urine.
- 📌 PALE Mnemonic: Proteinuria, HypoAlbuminemia, HyperLipidemia, Edema.
⭐ Loss of antithrombin III in nephrotic syndrome urine creates a hypercoagulable state, predisposing patients to thrombosis, particularly renal vein thrombosis.
Pathology Parade - Rogues' Gallery
- Nephrotic Syndrome: Massive proteinuria (>3.5 g/day), hypoalbuminemia, edema, hyperlipidemia/uria.
- 📌 PALE: Proteinuria, Albuminemia (hypo), Lipidemia (hyper), Edema.
- Minimal Change (MCD): #1 in kids. LM normal; EM shows podocyte effacement.
- FSGS: #1 in adults (esp. Black). LM shows sclerosis; EM effacement.
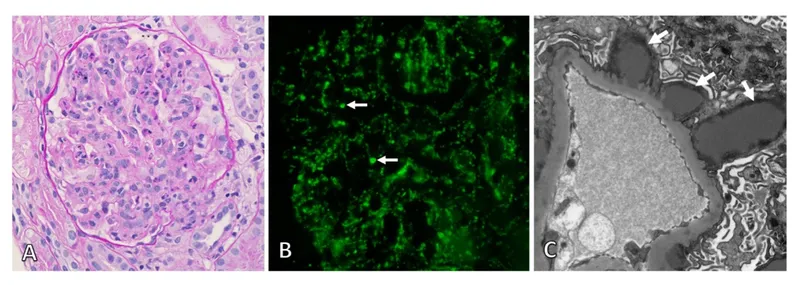
- Membranous Nephropathy: #2 in adults. LM thick GBM; IF granular; EM "spike & dome."
- Nephritic Syndrome: Inflammation. Hematuria (RBC casts), HTN, oliguria, azotemia.
- Post-strep (PSGN): LM hypercellular glomeruli; IF "starry sky"; EM subepithelial humps.
- IgA Nephropathy (Berger): Most common cause worldwide. Episodic hematuria post-URI/GI infection.
- RPGN: Crescents on LM. Poor prognosis.
⭐ Subepithelial "humps" on EM are characteristic of PSGN, representing immune complex deposition.
High‑Yield Points - ⚡ Biggest Takeaways
- Nephritic syndrome: Inflammatory process causing hematuria (RBC casts), oliguria, and hypertension.
- Nephrotic syndrome: Massive proteinuria (>3.5 g/day), hypoalbuminemia, edema, and hyperlipidemia.
- Linear IF is pathognomonic for Goodpasture syndrome; most others are granular.
- Podocyte effacement on EM is the hallmark of Minimal Change Disease.
- Look for "spike and dome" in Membranous Nephropathy and "tram-tracks" in MPGN.
- FSGS is the most common cause of nephrotic syndrome in adults.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

