Pulmonary Embolism - The Clot Thickens
- Pathophysiology: Occlusion of pulmonary artery → ↑ pulmonary vascular resistance → RV strain. Creates ventilation/perfusion (V/Q) mismatch (ventilated, not perfused).
- Origin: >95% from deep vein thrombosis (DVT) in lower extremities.
- Risk Factors (Virchow's Triad): Stasis, hypercoagulability, endothelial injury.
- Clinical Features: Sudden-onset dyspnea, pleuritic chest pain, tachypnea, tachycardia. May have hemoptysis.
⭐ V/Q Scan: Shows perfusion defects with normal ventilation. The "gold standard" if CTPA is contraindicated (e.g., renal failure, contrast allergy).
- Management: Anticoagulation (heparin, DOACs). Thrombolysis or embolectomy if hemodynamically unstable (massive PE).
- Non-Thrombotic Emboli: 📌 FAT BAT: Fat, Air, Thrombus, Bacteria, Amniotic fluid, Tumor.
Pulmonary Hypertension - Pressure Overload
- Definition: Mean pulmonary arterial pressure (mPAP) > 20 mmHg at rest.
- Pathophysiology: Endothelial dysfunction → ↑ vasoconstrictors (e.g., endothelin) & ↓ vasodilators (e.g., NO, prostacyclin) → vascular remodeling, smooth muscle hypertrophy, & intimal fibrosis.
- WHO Classification Groups:
- 1: Pulmonary Arterial Hypertension (PAH) (idiopathic, heritable, drugs)
- 2: Due to left heart disease (e.g., mitral stenosis)
- 3: Due to chronic lung disease/hypoxia (e.g., COPD, OSA)
- 4: Chronic thromboembolic (CTEPH)
- 5: Multifactorial
- Presentation: Exertional dyspnea, fatigue, syncope on exertion. Loud P2, right ventricular heave.
- Diagnosis: Echocardiogram (screening) → Right Heart Catheterization (gold standard).
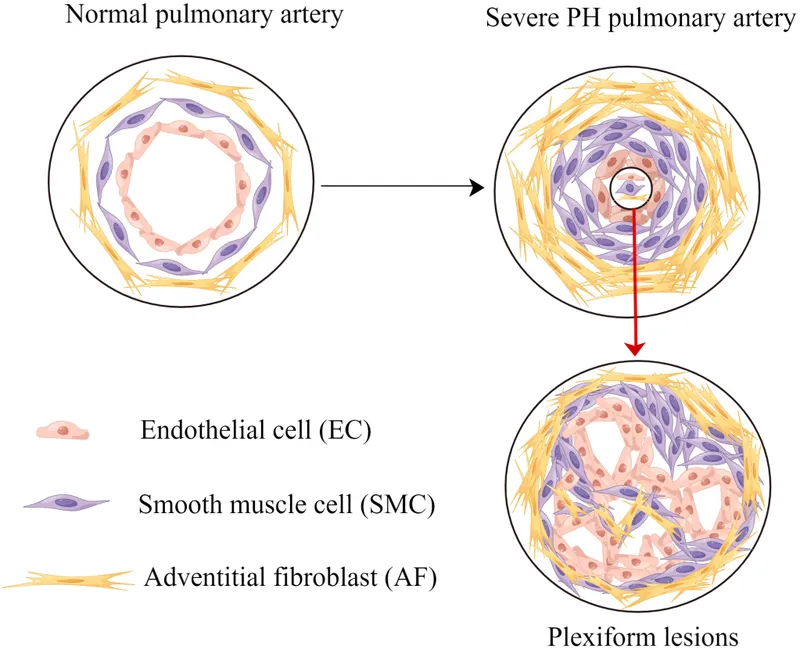
⭐ Plexiform lesions, representing tufts of capillary formations, are pathognomonic for severe, long-standing Group 1 PAH (idiopathic/heritable).
Other Emboli - Unwanted Guests
-
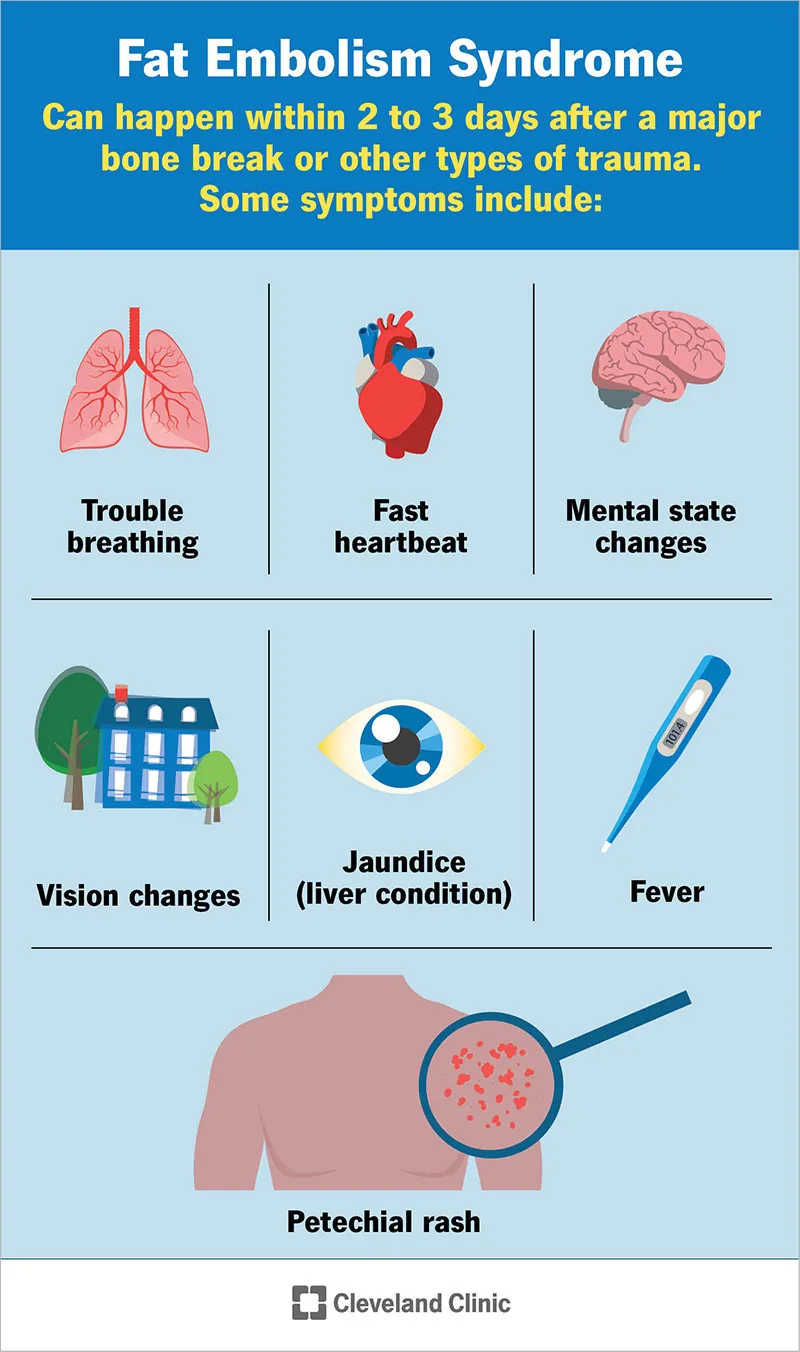
Fat Embolism Syndrome (FES):
- Cause: Long bone fractures (femur), orthopedic surgery, liposuction.
- Pathophysiology: Mechanical obstruction & inflammatory response to free fatty acids.
- Classic Triad:
- Hypoxemia
- Neurologic dysfunction (e.g., confusion)
- Petechial rash (axilla/chest) - often delayed.
- Diagnosis: Clinical; fat in urine/sputum.
-
Air Embolism:
- Cause: Iatrogenic (central lines), trauma, barotrauma (diving).
- Effect: Obstructs RV outflow tract → acute right heart failure.
- Management: Left lateral decubitus position.
-
Amniotic Fluid Embolism:
- Pathophysiology: Fetal material enters maternal circulation.
- Presentation: Abrupt cardiogenic shock, respiratory failure, & DIC during/after labor.
⭐ High-Yield: Amniotic fluid embolism is a clinical diagnosis of exclusion, often presenting with sudden cardiovascular collapse and coagulopathy during or shortly after childbirth. It carries a very high mortality rate.
- Pulmonary embolism (PE) most commonly originates from deep vein thrombosis (DVT).
- Suspect PE with sudden-onset dyspnea, pleuritic chest pain, and tachypnea.
- CT pulmonary angiography is the gold standard for PE diagnosis; use V/Q scan if contraindicated.
- Pulmonary hypertension (mean PAP >20 mmHg) leads to cor pulmonale (RV hypertrophy and failure).
- Idiopathic pulmonary arterial hypertension is classically linked to a BMPR2 gene mutation.
- Fat embolism syndrome triad (post-long bone fracture): neurologic changes, petechial rash, and respiratory distress.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

