Serous & Fibrinous - Leaky & Sticky
-
Serous Inflammation: "Leaky"
- Fluid: Thin, watery, cell-poor exudate.
- Mechanism: Mild ↑ vascular permeability allows plasma ultrafiltrate to escape.
- Examples: Skin blister (burn), viral pleuritis, joint effusion.
- Outcome: Usually resolves without sequelae.
-
Fibrinous Inflammation: "Sticky"
- Fluid: Exudate rich in plasma proteins, especially fibrinogen.
- Mechanism: Greater ↑ in vascular permeability allows large molecules to leak; fibrinogen polymerizes to fibrin.
- Appearance: "Bread and butter" on serosal surfaces.
- Examples: Uremic pericarditis, rheumatic carditis, pneumococcal pneumonia.
- Outcomes: Resolution (fibrinolysis) or organization (scarring).
⭐ A classic friction rub is auscultated in fibrinous pericarditis due to rough surfaces rubbing.
Suppurative (Purulent) - The Pus Parade
- Hallmark: Characterized by the production of pus (purulent exudate).
- Composition: Primarily a viscous liquid of neutrophils (living, dying, and necrotic), cellular debris from liquefactive necrosis, and edema fluid.
- Causative Agents: Typically initiated by pyogenic (pus-forming) bacteria.
- Classic culprit: Staphylococcus aureus.
- Mechanism: Potent chemoattractants lead to a massive influx of neutrophils. These cells release lysosomal enzymes that digest and liquefy tissue, forming pus.
- Clinical Forms:
- Abscess: A localized collection of pus confined within tissue.
- Empyema: Pus accumulation in a pre-existing body cavity (e.g., pleura).
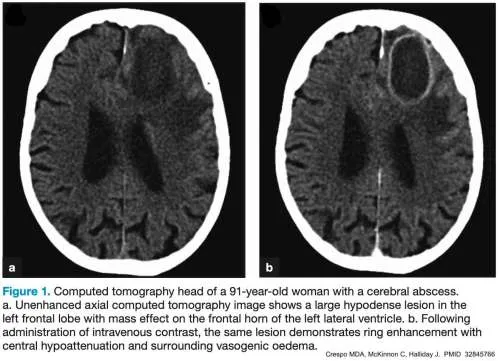
⭐ An abscess represents a battlefield: a central core of liquefactive necrosis is surrounded by a wall of viable neutrophils, which is in turn encircled by a fibroblastic capsule as a sign of attempted repair.
Ulcerative Inflammation - Surface Breaches
- Definition: A local defect or excavation on the surface of an organ or tissue, caused by the shedding of inflamed necrotic tissue.
- Pathogenesis: Involves a breach of the epithelial barrier, extending into the underlying submucosa or deeper, often with an acute and chronic inflammatory response in the base.
- Key Examples:
- GI Tract: Peptic ulcers (stomach, duodenum), ulcerative colitis.
- Oral Cavity: Aphthous ulcers.
- Lower Extremities: Diabetic foot ulcers.
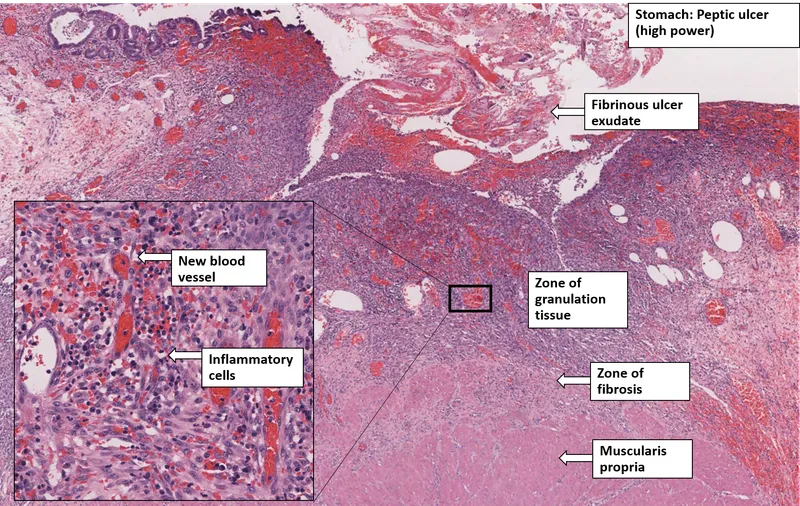
⭐ A true ulcer penetrates the muscularis mucosae, whereas an erosion is a superficial breach of the epithelium. This distinction is crucial for GI pathology.
Granulomatous Inflammation - Walled-Off Warriors
- A distinct chronic inflammatory pattern; a collection of activated, "walled-off" macrophages (epithelioid histiocytes) trying to contain a persistent stimulus.
- Key Components:
- Epithelioid histiocytes: Activated macrophages with abundant pink cytoplasm.
- Giant cells: Fused macrophages (e.g., Langhans type in TB).
- Lymphocytic cuff: Rim of T-cells, primarily Th1.

- Major Types:
- Caseating: Features central necrosis. Seen in Tuberculosis, systemic fungi.
- Non-caseating: Lacks central necrosis. Seen in Sarcoidosis, Crohn's disease, foreign body reactions.
⭐ TNF-α is critical for forming and maintaining granulomas. Patients on TNF-α inhibitors (e.g., infliximab) are at high risk for reactivating latent TB.
High‑Yield Points - ⚡ Biggest Takeaways
- Serous inflammation is characterized by thin, watery fluid (effusion), like in a skin blister.
- Fibrinous inflammation involves fibrin deposition from leaky vessels, classic in pericarditis.
- Suppurative inflammation features pus (neutrophils, debris), typically from pyogenic bacteria; an abscess is a localized collection.
- Ulcers are surface defects from the sloughing of inflamed necrotic tissue.
- Granulomatous inflammation uses activated macrophages to wall off persistent agents like TB.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

