Primary Immunodeficiencies - The Body's Defense Gaps
- B-cell: X-Linked Agammaglobulinemia (Bruton): ↓ Ig of all classes. Defect in BTK.
- T-cell: DiGeorge Syndrome: 22q11 deletion. Thymic aplasia. ↓ T-cells.
- Combined: SCID: Defective T-cells; B-cell dysfunction is secondary. Multiple gene defects (e.g., IL-2R gamma chain, ADA).
- Phagocytic: Chronic Granulomatous Disease (CGD): Defect in NADPH oxidase.
⭐ Absent thymic shadow on newborn chest X-ray is a classic sign of SCID.
B-Cell Blues - Antibody Production Problems
- X-Linked Agammaglobulinemia (Bruton's):
- BTK gene defect → no B-cell maturation.
- Recurrent encapsulated bacterial infections after 6 months.
- Labs: ↓ all Igs, absent CD19+ B cells.
- Anatomy: Scanty tonsils/lymph nodes.
- Selective IgA Deficiency:
- Most common primary immunodeficiency; isolated ↓ IgA.
- Mostly asymptomatic; may have sinopulmonary/GI infections, atopy.
- ⚠️ Anaphylaxis risk with blood products.
- Common Variable Immunodeficiency (CVID):
- Defective B-cell differentiation; late onset (20s-40s).
- Labs: ↓ plasma cells, ↓ IgG & ↓ IgA/IgM.
- ↑ risk of autoimmune disease & lymphoma.
⭐ Patients with Selective IgA Deficiency can develop severe anaphylaxis when transfused with blood containing IgA, as their immune system recognizes it as foreign.
T-Cell Troubles - Cellular Immunity Collapse
-
Thymic Aplasia (DiGeorge Syndrome)
- 22q11.2 deletion → failed 3rd/4th pharyngeal pouch development.
- 📌 CATCH-22: Cardiac defects, Abnormal facies, Thymic hypoplasia, Cleft palate, Hypocalcemia.
- Labs: ↓ T-cells, ↓ PTH, ↓ Ca²⁺. Absent thymic shadow on CXR.
-
IL-12 Receptor Deficiency
- ↓ Th1 response → disseminated mycobacterial & fungal infections; ↓ IFN-γ.
-
Hyper-IgE Syndrome (Job Syndrome)
- STAT3 mutation → impaired Th17 cells.
- 📌 FATED: coarse Facies, cold staph Abscesses, retained primary Teeth, ↑ IgE, Dermatologic (eczema).
⭐ Patients with DiGeorge syndrome often present with congenital heart defects like Tetralogy of Fallot or truncus arteriosus.
Combined Chaos - When B & T Cells Fail
-
Severe Combined Immunodeficiency (SCID)
- Most severe form; multiple genetic defects (e.g., IL-2R gamma chain, ADA deficiency).
- Presents with failure to thrive, chronic diarrhea, and severe recurrent infections.
- Key finding: Absent thymic shadow on chest X-ray.

-
Ataxia-Telangiectasia
- Defect in ATM gene; failure to repair DNA double-strand breaks.
- Triad: Ataxia, Angiomas (telangiectasias), IgA deficiency.
- Lab finding: ↑ alpha-fetoprotein.
-
Wiskott-Aldrich Syndrome (WAS)
- X-linked recessive; defect in WASp gene.
- 📌 WATER mnemonic: Wiskott-Aldrich: Thrombocytopenia, Eczema, Recurrent infections.
⭐ In Ataxia-Telangiectasia, the DNA repair defect leads to an increased risk of lymphoma and leukemia.
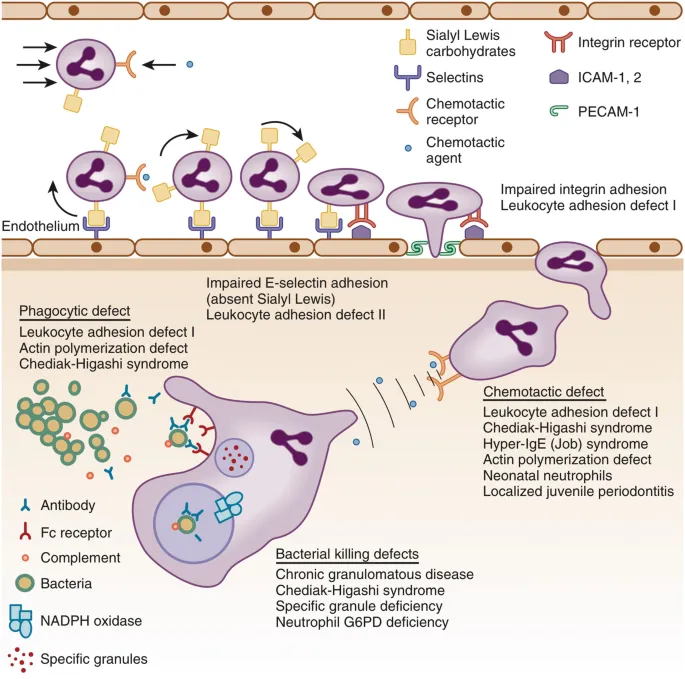
Phagocyte Phails - Cleanup Crew on Strike
- Chronic Granulomatous Disease (CGD): Defect in NADPH oxidase → impaired respiratory burst.
- Recurrent infections by catalase-positive organisms (e.g., S. aureus, Aspergillus).
- Diagnosis: ↓ Dihydrorhodamine (DHR) flow cytometry test.
- Leukocyte Adhesion Deficiency (LAD-1): Defective CD18 (LFA-1 integrin) → impaired leukocyte adhesion & migration.
- Presents with delayed umbilical cord separation, recurrent skin infections without pus.
- Chédiak-Higashi Syndrome: LYST gene defect → impaired phagosome-lysosome fusion.
- Features: Recurrent pyogenic infections, partial albinism, peripheral neuropathy.
⭐ In Leukocyte Adhesion Deficiency (LAD), infections are notably non-purulent (lack pus) because neutrophils can't extravasate to the site of inflammation.
- X-linked agammaglobulinemia (XLA) features a BTK gene defect, leading to no B-cell maturation and recurrent bacterial infections after 6 months.
- DiGeorge syndrome (22q11.2 deletion) causes T-cell deficiency from thymic aplasia, plus hypocalcemia and cardiac defects.
- Severe Combined Immunodeficiency (SCID) shows absent T and B-cell function, requiring an urgent bone marrow transplant.
- Wiskott-Aldrich syndrome is an X-linked disorder with a triad of thrombocytopenia, eczema, and recurrent infections.
- IgA deficiency is the most common PID, often asymptomatic but with a risk of anaphylaxis to blood products.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

