Overview & Types - Outpouching Problems
- Diverticulosis: Uninflamed, asymptomatic outpouchings (pseudodiverticula).
- Diverticulitis: Inflammation of diverticula, causing LLQ pain, fever.
- True vs. False Diverticula:
- False (e.g., Colonic): Herniation of mucosa & submucosa through the muscularis propria. Most common.
- True (e.g., Meckel's): Includes all three gut wall layers.
- Location: Sigmoid colon is the most common site due to high intraluminal pressure.
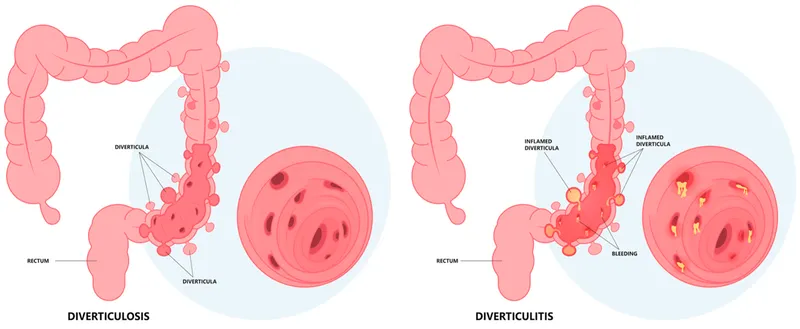
⭐ Diverticular bleeding is the most common cause of acute lower GI bleeding in adults.
Pathophysiology - Pressure Cooker Colon
- Etiology: Chronic constipation, often from a low-fiber diet, leads to increased straining and segmented colonic contractions.
- Mechanism: Results in ↑ intraluminal pressure, forcing the herniation (pulsion) of mucosa and submucosa.
- Herniation occurs through natural weak points in the muscularis propria, specifically where the vasa recta (nutrient arteries) penetrate.
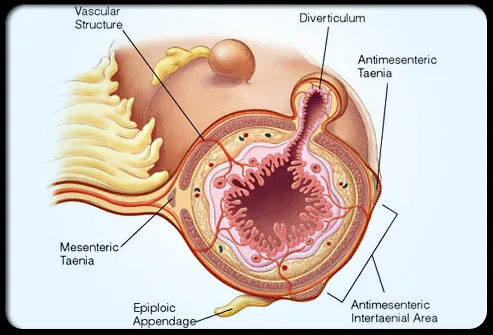
⭐ Sigmoid Colon Predilection: The sigmoid is the most common site (>90%). According to the Law of Laplace ($P \propto 1/r$), its narrower diameter generates the highest intraluminal pressure.
Clinical Presentation - Belly Aches & Bleeds
- Diverticulosis: Often asymptomatic. The hallmark is painless hematochezia-sudden, massive, maroon-colored rectal bleeding that typically stops spontaneously. May have mild, intermittent cramping.
- Diverticulitis: Presents as a steady, deep LLQ abdominal pain, fever, anorexia, nausea, and vomiting. Altered bowel habits (constipation or diarrhea) are common. On exam, find localized LLQ tenderness.
⭐ Exam Tip: While inflammation (-itis) is most common in the left-sided sigmoid colon, significant bleeding (-osis) more frequently originates from right-sided colonic diverticula.
Diagnosis - Seeing the Sacs
- Diverticulosis: Typically an incidental finding on screening colonoscopy, revealing multiple colonic outpouchings (diverticula).
- Acute Diverticulitis:
- Abdominal/pelvic CT with contrast is the best initial and most accurate test.
- Key findings: Localized bowel wall thickening (>4 mm), pericolic fat stranding, abscess, or extraluminal air/fluid.
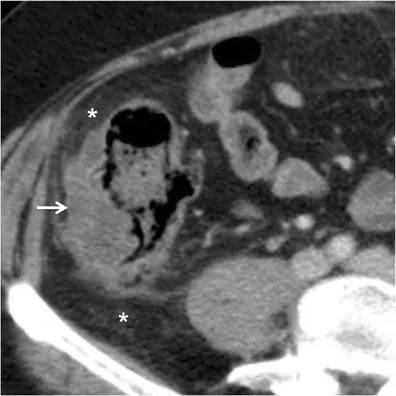
⭐ ⚠️ In acute diverticulitis, avoid colonoscopy and barium enema. They are contraindicated due to the high risk of perforation.
Management & Complications - Fixing the Flaws
- Complications: 📌 FOPA
- Fistula (Colovesical → pneumaturia)
- Obstruction
- Perforation (→ peritonitis)
- Abscess (most common)
⭐ Recurrent uncomplicated diverticulitis or a single complicated episode often prompts consideration for elective sigmoid colectomy to prevent future attacks and severe complications.
High‑Yield Points - ⚡ Biggest Takeaways
- Diverticulosis is typically asymptomatic and linked to a low-fiber diet; diverticulitis presents with LLQ pain and fever.
- The sigmoid colon is the most common site due to high intraluminal pressure.
- These are false (pulsion) diverticula, occurring at weak points where vasa recta penetrate the muscularis propria.
- Painless rectal bleeding is a complication of diverticulosis, not diverticulitis.
- CT scan with contrast is the best test for acute diverticulitis; avoid colonoscopy in the acute setting due to perforation risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

