Parathyroid Physiology - Calcium's Command Center
- Primary function: Regulate serum calcium via Parathyroid Hormone (PTH).
- PTH actions:
- Bone: ↑ Ca²⁺ & PO₄³⁻ resorption.
- Kidney: ↑ Ca²⁺ reabsorption, ↓ PO₄³⁻ reabsorption.
- Gut (indirectly): ↑ Vitamin D (calcitriol) activation → ↑ Ca²⁺ absorption.
- 📌 Mnemonic: PTH = Phosphate Trashing Hormone.
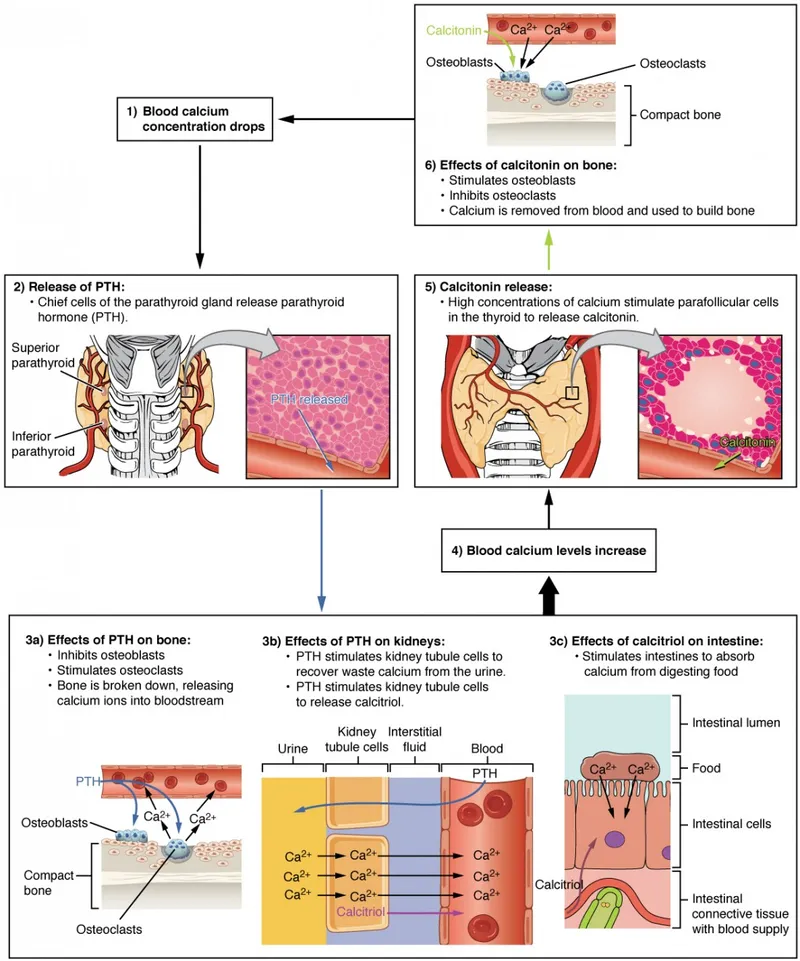
⭐ PTH stimulates the enzyme 1-alpha-hydroxylase in the proximal convoluted tubules of the kidney, converting calcidiol to the active form, calcitriol (1,25-dihydroxyvitamin D).
Hyperparathyroidism - Calcium Overload Chaos
-
Primary: Unregulated PTH secretion, most often from a parathyroid adenoma (>80%).
- Labs: ↑ PTH, ↑ Ca²⁺, ↓ PO₄³⁻, ↑ urinary cAMP, ↑ alkaline phosphatase.
- Clinical: 📌 "Stones, bones, groans, psychiatric overtones."
- Stones: Recurrent calcium nephrolithiasis.
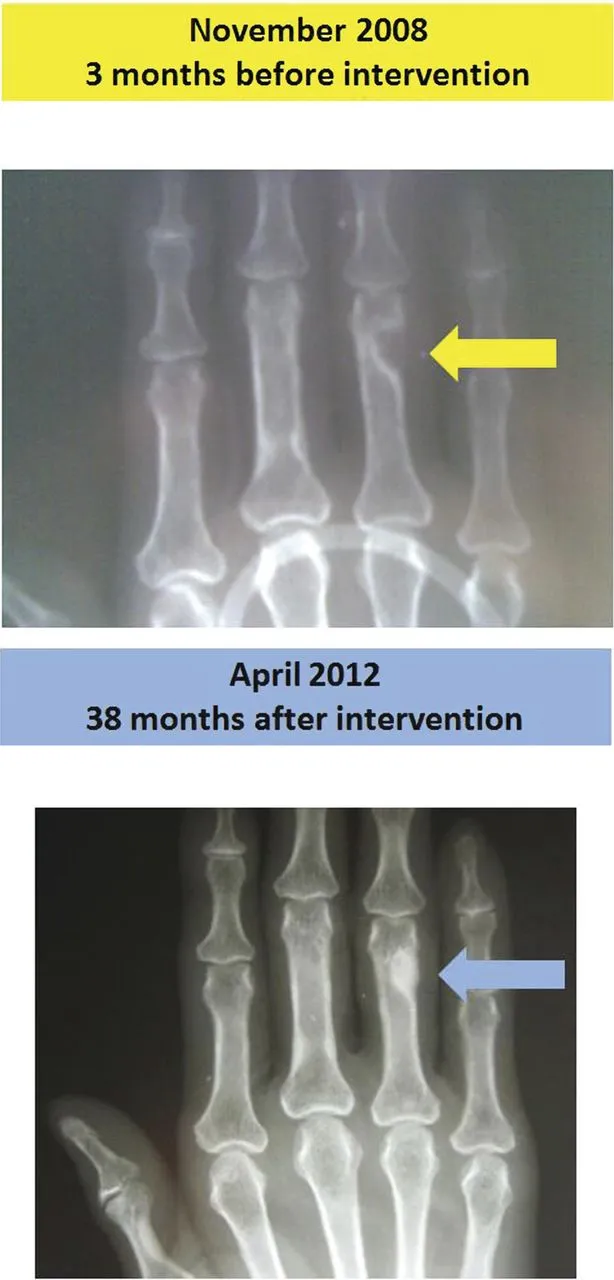
- Bones: Osteitis fibrosa cystica ("brown tumors").
- Groans: Constipation, pancreatitis, peptic ulcers.
- Psychiatric: Fatigue, depression, confusion.
-
Secondary: Compensatory PTH secretion from chronic hypocalcemia.
- Cause: Chronic kidney disease is the most common cause (↓ 1,25-dihydroxyvitamin D, ↑ PO₄³⁻).
- Labs: ↑ PTH, but ↓ or normal Ca²⁺.
-
Tertiary: Autonomous PTH secretion following long-standing secondary hyperparathyroidism. Labs show ↑ PTH and ↑ Ca²⁺.
⭐ Differentiate primary hyperparathyroidism from Familial Hypocalciuric Hypercalcemia (FHH), which presents with low urinary calcium excretion due to a CASR gene mutation.
Hypoparathyroidism - The Calcium Crash
- Etiology: Most commonly iatrogenic (post-thyroidectomy). Also, autoimmune disease, DiGeorge syndrome (22q11 deletion), severe hypomagnesemia.
- Pathophysiology: ↓PTH leads to ↓Ca²⁺ and ↑PO₄³⁻.
- ↓Renal Ca²⁺ reabsorption & ↓bone resorption.
- ↓1α-hydroxylase activity → ↓calcitriol → ↓GI Ca²⁺ absorption.
- Clinical: Neuromuscular excitability from hypocalcemia.
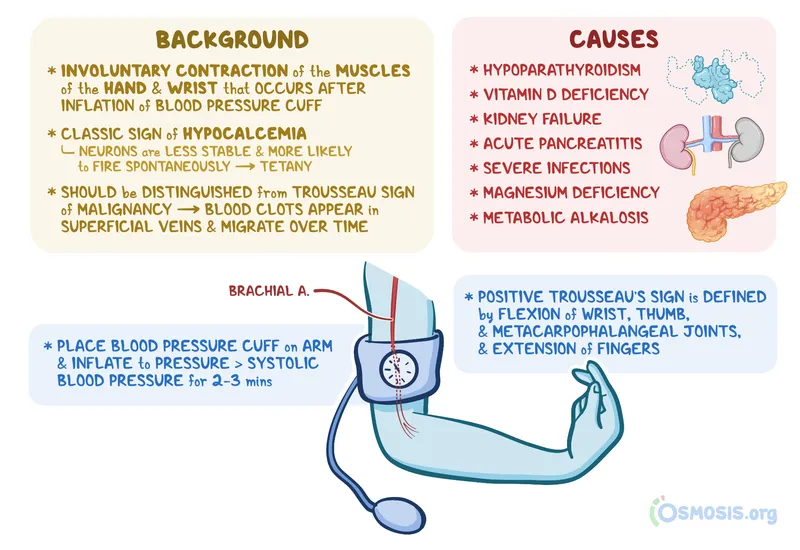
- Tetany: Chvostek's sign (facial tap), Trousseau's sign (carpal spasm with BP cuff).
- Paresthesias (perioral, digital), seizures.
- ECG: Prolonged QT interval.
- Labs: ↓Ca²⁺, ↑PO₄³⁻, ↓PTH.
⭐ Trousseau's sign (carpopedal spasm induced by ischemia) is more specific for hypocalcemia than Chvostek's sign.
📌 CATS: Convulsions, Arrhythmias, Tetany, Spasms/Stridor.
PTH Pretenders - Mimics & Variants
- Familial Hypocalciuric Hypercalcemia (FHH):
- Autosomal dominant defect in the Ca²⁺-sensing receptor (CASR) gene.
- Results in asymptomatic hypercalcemia, normal or mildly ↑PTH, and low urine calcium excretion.
- Benign; parathyroidectomy is not indicated.
⭐ Differentiate FHH from primary hyperparathyroidism via the calcium/creatinine clearance ratio (CCCR). A ratio <0.01 strongly suggests FHH.
-
Pseudohypoparathyroidism (PHP):
- End-organ resistance to PTH → hypocalcemia, hyperphosphatemia, despite ↑PTH levels.
- Type 1a: Maternal GNAS1 mutation. Associated with Albright's Hereditary Osteodystrophy (AHO) phenotype: short stature, obesity, shortened 4th/5th metacarpals.
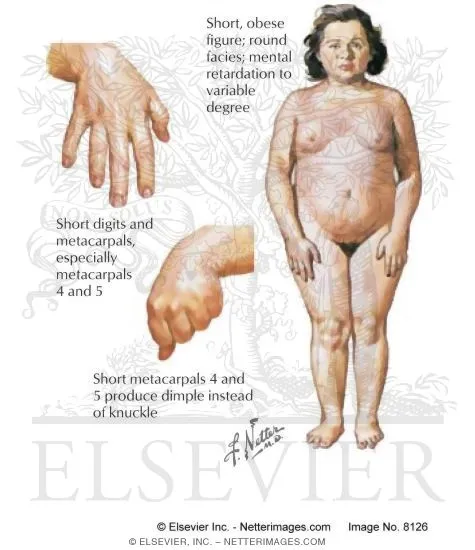
-
Pseudopseudohypoparathyroidism (PPHP):
- Paternal GNAS1 mutation. Patient has the AHO phenotype but with normal biochemistry (Ca²⁺, PO₄³⁻, PTH).
High‑Yield Points - ⚡ Biggest Takeaways
- Primary hyperparathyroidism, most often from a parathyroid adenoma, causes symptomatic hypercalcemia ("stones, bones, groans").
- Secondary hyperparathyroidism is a physiologic response to hypocalcemia, typically from chronic kidney disease.
- Tertiary hyperparathyroidism is autonomous PTH secretion after chronic secondary disease, causing marked hypercalcemia.
- Hypoparathyroidism, commonly post-thyroidectomy, presents with hypocalcemic tetany (Chvostek/Trousseau signs).
- Pseudohypoparathyroidism involves end-organ PTH resistance, leading to hypocalcemia despite high PTH.
- Familial Hypocalciuric Hypercalcemia (FHH) causes asymptomatic hypercalcemia with low urine calcium.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

