Adrenal Medulla - Catecholamine HQ
- Core Function: Central hub for catecholamine synthesis and secretion (Epinephrine > Norepinephrine). Regulated by preganglionic sympathetic fibers.
- Histology: Composed of chromaffin cells, which are modified postganglionic sympathetic neurons derived from the neural crest.
- Synthesis Pathway:
⭐ The enzyme converting norepinephrine to epinephrine, PNMT (Phenylethanolamine-N-methyltransferase), is upregulated by high local cortisol levels from the adrenal cortex. This unique vascular connection ensures maximal epinephrine production during stress.
Pheochromocytoma - The Great Masquerader
- Tumor of chromaffin cells in the adrenal medulla; secretes catecholamines.
- Rule of 10s: 10% extra-adrenal, 10% bilateral, 10% malignant, 10% calcify, 10% in children.
- Clinical: Episodic hypertension, headaches, palpitations, and sweating.
- 📌 5 P's: Pressure (HTN), Pain (headache), Perspiration, Palpitations, Pallor.
- Diagnosis: ↑ 24-hr urinary metanephrines and vanillylmandelic acid (VMA). Plasma-free metanephrines are also highly sensitive. CT/MRI to localize.
- Treatment: Surgical resection is definitive.
- Pre-op: irreversible α-blocker (phenoxybenzamine) followed by β-blockers.
⭐ Exam Favorite: Always administer alpha-blockade before beta-blockade to prevent unopposed alpha-adrenergic receptor stimulation, which can lead to a hypertensive crisis.
Pheochromocytoma: Dx & Rx - Taming the Tumor
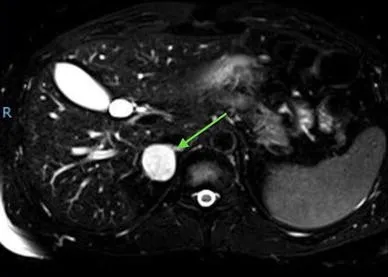
-
Diagnosis: Rule of 10s 📌
- 10% extra-adrenal, 10% bilateral, 10% malignant.
- Biochemical: ↑ plasma free metanephrines (best sensitivity) or 24-hr urinary fractionated metanephrines & catecholamines.
- Imaging: CT or MRI to localize tumor; MIBG scan for extra-adrenal or metastatic disease.
-
Treatment: "α then β"
⭐ Giving β-blockers before adequate α-blockade can precipitate a hypertensive crisis due to unopposed α-receptor stimulation.
Neuroblastoma - Childhood Adrenal Foe
- Most common extracranial solid tumor of childhood; median age at diagnosis is 1-2 years.
- Origin: Arises from neural crest cells of the adrenal medulla (~40%) or sympathetic ganglia.
- Clinical Features:
- Presents as a firm, irregular abdominal mass that can cross the midline.
- Opsoclonus-myoclonus-ataxia syndrome ("dancing eyes, dancing feet").
- Periorbital ecchymoses ("raccoon eyes") from orbital metastases.
- Blueberry muffin rash (subcutaneous nodules).
- Diagnosis:
- ↑ urinary catecholamine metabolites: vanillylmandelic acid (VMA) and homovanillic acid (HVA).
- Biopsy: Small, round blue cells forming Homer-Wright rosettes.
- Bombesin and neuron-specific enolase (NSE) positive.
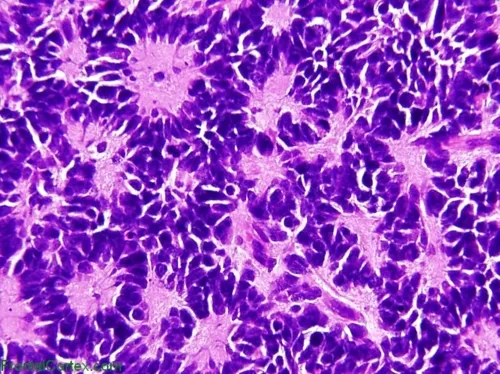
⭐ N-myc gene amplification is a key prognostic marker indicating a poor prognosis. However, spontaneous regression is common in infants < 1 year old.
High‑Yield Points - ⚡ Biggest Takeaways
- Pheochromocytoma, a tumor of chromaffin cells, follows the rule of 10s and presents with episodic hypertension, palpitations, and headaches.
- Diagnose with elevated urine/plasma metanephrines and VMA.
- Pre-operative treatment is crucial: alpha-blockade (e.g., phenoxybenzamine) before beta-blockade.
- Associated with MEN 2A/2B, VHL, and NF1.
- Neuroblastoma is the most common extracranial solid childhood tumor, often presenting as an abdominal mass.
- Look for opsoclonus-myoclonus syndrome and elevated urine HVA/VMA.
- N-myc amplification signifies a poor prognosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

