Pain Relief Roadmap - Setting the Stage
- Goal: Balance maternal comfort with fetal/maternal safety and labor progress. Choice is guided by maternal preference, contraindications, and labor stage.
- Two primary pathways exist for managing labor pain:
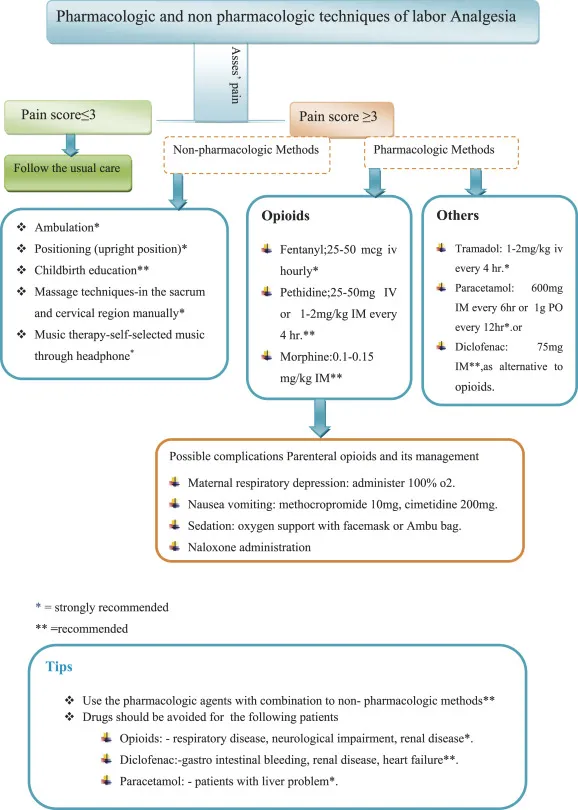
- Non-Pharmacologic: Often first-line.
- Techniques: Breathing, hydrotherapy, massage, position changes.
- Benefits: Minimal side effects, increased maternal sense of control.
- Pharmacologic: For moderate-to-severe pain.
- Routes: Systemic (IV) or neuraxial (spinal/epidural).
Natural Comfort - The Drug-Free Zone
- Psychoprophylaxis (e.g., Lamaze): Utilizes controlled breathing, relaxation, and a support person (doula) to manage contractions. Aims to break the fear-tension-pain cycle.
- Hydrotherapy: Warm water immersion in a tub or shower can decrease anxiety and perception of pain.
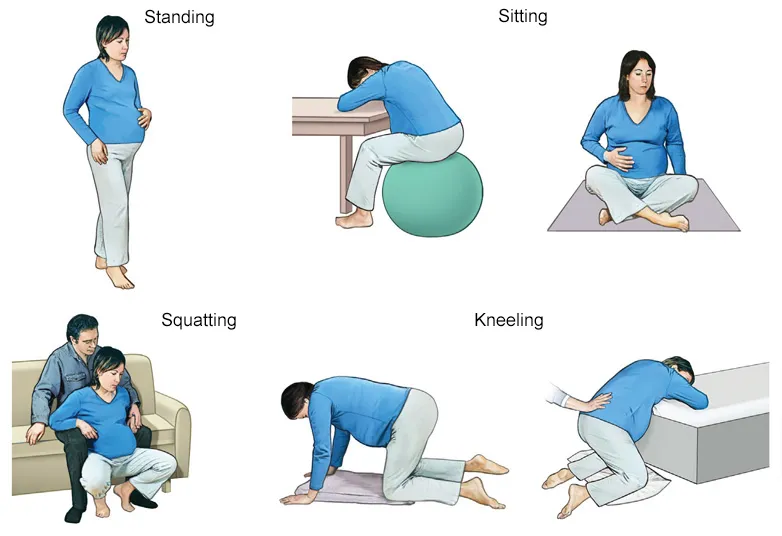
- Movement & Positioning: Encouraging walking, swaying, or using a birthing ball helps manage discomfort and can facilitate fetal descent.
- Other Modalities:
- Massage & Counterpressure: Particularly effective for back labor caused by fetal position.
- TENS: Transcutaneous electrical nerve stimulation; non-invasive with variable efficacy.
Systemic Soothers - Taking the Edge Off
| Feature | Systemic Opioids (e.g., Fentanyl, Remifentanil) | Nitrous Oxide (N₂O) |
|---|---|---|
| Mechanism | µ-opioid receptor agonist | NMDA receptor antagonist |
| Admin | IV/IM by staff | Self-administered via mask (50% N₂O/50% O₂) |
| Maternal SE | Sedation, nausea/vomiting, pruritus | Dizziness, nausea, lightheadedness |
| Fetal Effects | ↓ FHR variability, potential for neonatal respiratory depression | Minimal; rapidly cleared from neonatal circulation |
| Key Point | Crosses placenta; risk of neonatal sedation | Patient-controlled, rapid onset/offset |
Neuraxial Blockade - The Gold Standard
Provides superior pain relief compared to parenteral opioids. Choice depends on the stage of labor and clinical scenario.
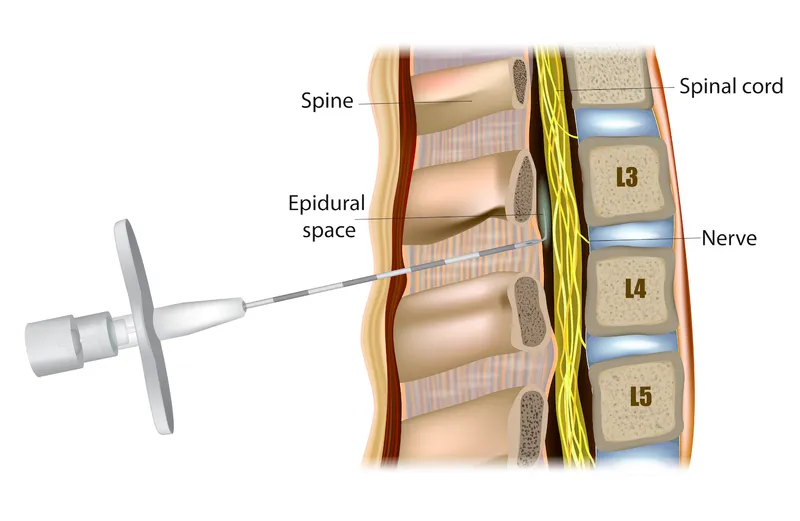
| Feature | Epidural Anesthesia | Spinal Anesthesia |
|---|---|---|
| Site | Epidural space (L2-L5) | Subarachnoid space (L2-L5) |
| Onset | Slower (10-20 min) | Rapid (2-5 min) |
| Agents | Bupivacaine, Ropivacaine + Fentanyl | Bupivacaine (hyperbaric) + Fentanyl |
| Use Case | Labor analgesia (continuous infusion) | Cesarean delivery (single shot) |
| Key Risk | Accidental dural puncture | Post-dural puncture headache (PDPH) |
- **Hypotension:** Most common side effect due to sympathetic blockade.
- **Pruritus:** Common with opioids (Fentanyl); treat with naloxone or diphenhydramine.
- **Inadequate block:** May require catheter replacement.
⭐ PDPH presents as a postural headache (worse when upright, better when supine) 1-3 days post-procedure. Treatment of choice is an epidural blood patch.
High‑Yield Points - ⚡ Biggest Takeaways
- Epidural analgesia is the most effective pain relief but risks maternal hypotension and a prolonged second stage of labor.
- Spinal anesthesia provides rapid, dense blockade for cesarean delivery but carries a risk of post-dural puncture headache.
- A pudendal nerve block is ideal for perineal pain during the second stage but does not relieve uterine contraction pain.
- IV opioids are a systemic option but pose a significant risk of neonatal respiratory depression.
- General anesthesia is reserved for emergent C-sections when regional methods are contraindicated.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

