Indications & Prerequisites - Green Light for Go-Time
-
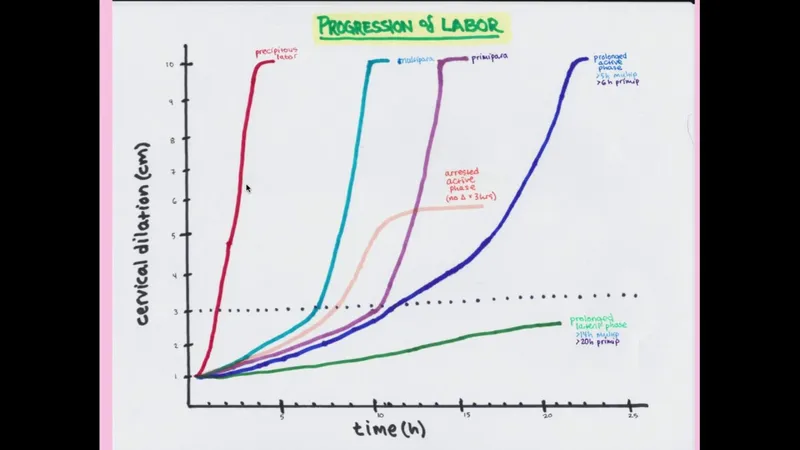
Primary Indication: Labor Dystocia (abnormally slow labor).
- Protraction Disorder: Cervical dilation slower than expected.
- Arrest Disorder: No cervical change for:
- ≥ 4 hours with adequate contractions.
- ≥ 6 hours with inadequate contractions.
-
Prerequisites:
- Confirmed, term, singleton, cephalic presentation.
- Reassuring fetal status (e.g., Category I FHR).
- No clinical signs of cephalopelvic disproportion (CPD).
⭐ The most common indication for labor augmentation is arrest of the active phase of labor.
The Augmentation Toolkit - Tools of the Trade
-
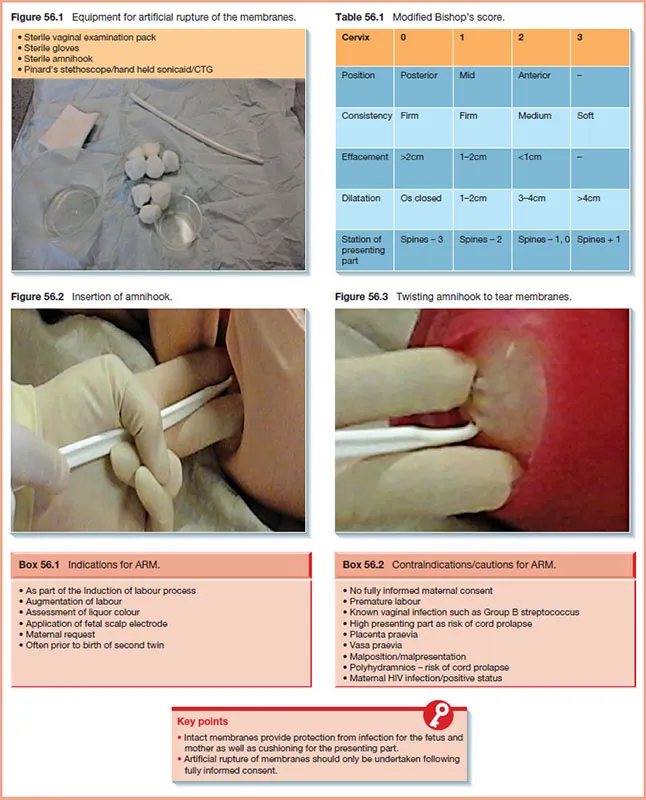
Amniotomy (AROM):
- Artificial rupture of membranes using a sterile amnihook.
- Releases prostaglandins, promoting contractions.
- Prerequisite: Cephalic presentation, head well-engaged to prevent cord prolapse.
- ⚠️ Risks: Chorioamnionitis, umbilical cord compression.
-
Oxytocin (Pitocin) Infusion:
- Synthetic hormone; ↑ frequency and strength of contractions.
- Administered via IV pump for precise dose control.
- Typical dose: Start 0.5-2 mU/min, titrate every 30-60 min.
- ⚠️ Risks: Uterine tachysystole (>5 contractions in 10 min), fetal distress, uterine rupture.
⭐ High doses of oxytocin can activate vasopressin (ADH) receptors, leading to water intoxication and hyponatremia.
Oxytocin Protocols - The Pitocin Playbook
-
Goal: Achieve adequate uterine contractions (≥200 Montevideo Units) to progress labor.
-
Administration: IV infusion, titrated to effect. Requires continuous fetal heart rate (FHR) and contraction monitoring.
-
Regimens:
- Low-Dose (Preferred): Start 0.5-2 mU/min; increase by 1-2 mU/min every 30-60 min.
- High-Dose: Start 6 mU/min; increase by 3-6 mU/min every 15-40 min. Faster, but higher risk.
-
⚠️ Risks:
- Uterine Tachysystole (>5 contractions in 10 min).
- Fetal distress (e.g., late decelerations).
- Water intoxication (hyponatremia).
⭐ Exam Favorite: Oxytocin is structurally similar to ADH. At high doses, it can exert an antidiuretic effect, causing water retention and dilutional hyponatremia.
Risks & Complications - Cautionary Tales

- Uterine Tachysystole: The most common complication, leading to reduced placental blood flow.
- Fetal Hypoxia & Acidosis: Consequence of tachysystole, visible as late decelerations on fetal heart rate (FHR) monitoring.
- Uterine Rupture: ⚠️ A catastrophic risk, particularly in patients with a history of uterine surgery (e.g., prior Cesarean section).
- Postpartum Hemorrhage (PPH): Can result from uterine atony after prolonged oxytocin exposure.
- Water Intoxication: Rare, due to the antidiuretic hormone (ADH) effect of oxytocin at high doses.
⭐ Tachysystole is defined as >5 contractions in 10 minutes, averaged over a 30-minute window.
High‑Yield Points - ⚡ Biggest Takeaways
- Labor augmentation addresses inadequate uterine contractions during the active phase of labor.
- Oxytocin is the primary pharmacologic agent used; it requires careful, continuous fetal and maternal monitoring.
- Amniotomy (AROM) can be used to augment labor, but only if the fetal head is well-engaged.
- A major risk is uterine tachysystole (>5 contractions in 10 minutes), which can cause fetal distress.
- Management of tachysystole includes stopping oxytocin and potential administration of a tocolytic.
- Prior to augmentation, ensure no contraindications to vaginal delivery exist, such as placenta previa.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

