Initial Management - The First Response
- Call for Help: Activate emergency response. Notify anesthesia, OR staff, and blood bank.
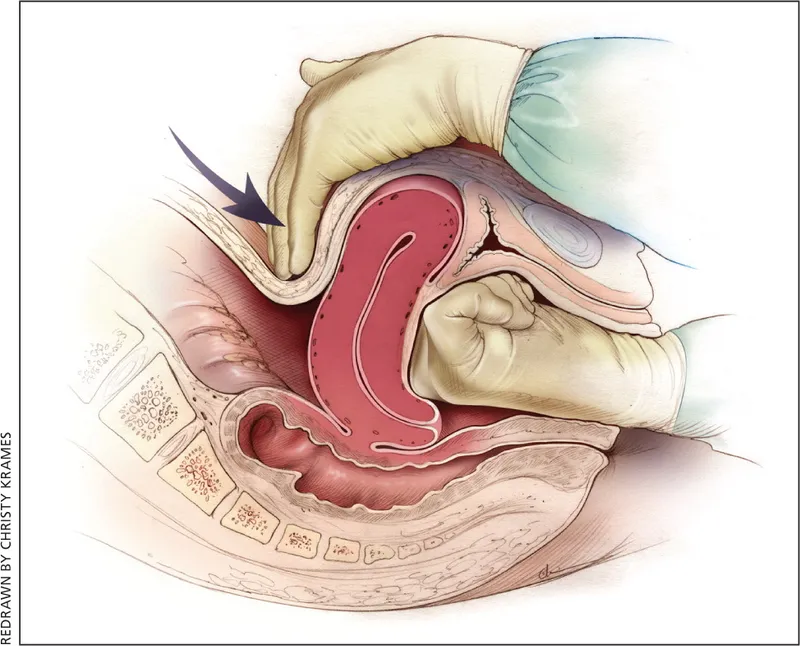
- Bimanual Uterine Massage: The cornerstone of initial management. One hand on the abdomen massages the fundus, while the other internally supports the uterus.
- Secure IV Access: Establish two large-bore IVs (≥18 gauge).
- Draw blood for CBC, type & crossmatch, and coagulation panel.
- Pharmacotherapy (Uterotonics):
- Oxytocin (Pitocin): First-line agent. Administer 20-40 units in 1L of crystalloid, run at a rate to control bleeding.
- Bladder Decompression: Insert a Foley catheter to empty the bladder, preventing interference with uterine contraction.
⭐ Tranexamic Acid (TXA): If initial measures are insufficient, administer 1g of TXA IV over 10 minutes. Must be given within 3 hours of delivery to be effective.
Uterotonic Agents - The Contraction Crew
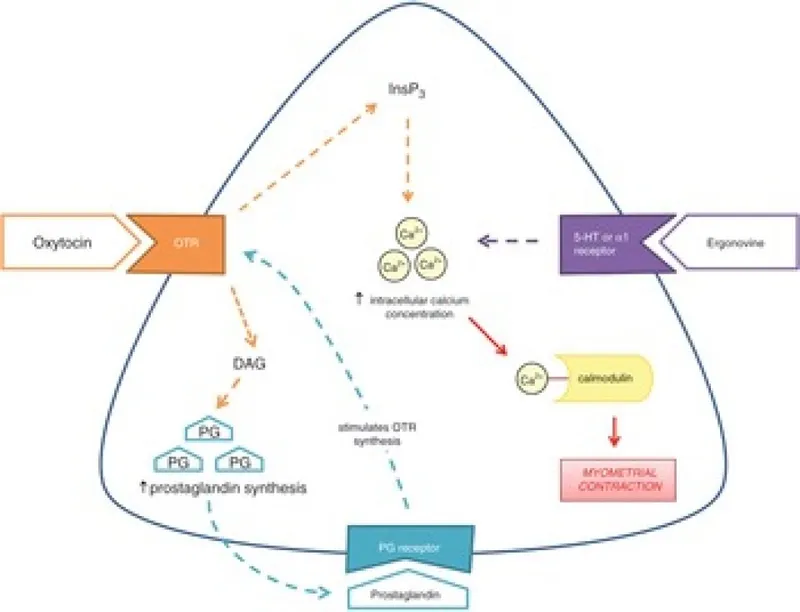
First-line therapy to ↑ uterine tone. Administer sequentially; assess response before adding next agent.
| Agent | Dose & Route | Contraindications (C/I) | Key Side Effects (S/E) |
|---|---|---|---|
| Oxytocin (Pitocin) | 10-40 units in 1L IV | None for PPH | Water intoxication, hypotension |
| Methylergonovine (Methergine) | 0.2 mg IM | Hypertension, preeclampsia, Raynaud's | ↑↑ BP (stroke risk) |
| Carboprost Tromethamine (Hemabate) | 250 mcg IM or intramyometrial | ⚠️ Asthma | Bronchospasm, N/V/D, fever |
| Misoprostol (Cytotec) | 800-1000 mcg rectally | None for PPH | Shivering, pyrexia, diarrhea |
⭐ Exam Favorite: Carboprost (a prostaglandin F2α analog) is a potent uterotonic but is absolutely contraindicated in patients with asthma due to its significant risk of inducing bronchospasm.
Refractory Hemorrhage - Escalation Steps
When initial uterotonic therapy fails to control bleeding, escalate management immediately. The goal is to achieve hemostasis while preserving fertility if possible.
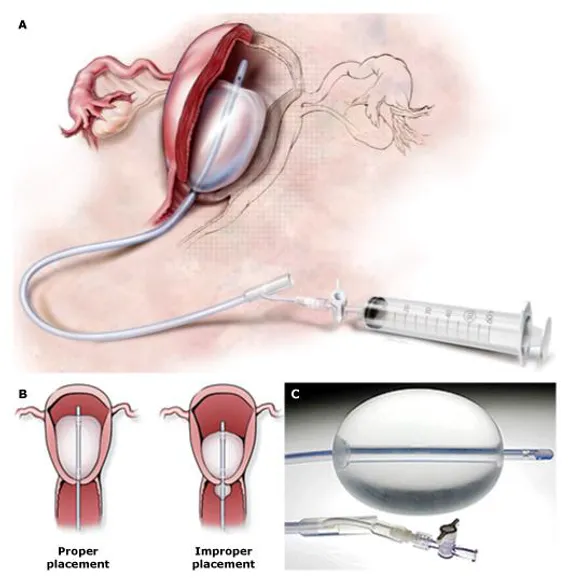
- Intrauterine Balloon Tamponade:
- A Bakri balloon is inserted into the uterus and inflated with ~500 mL of saline.
- Provides an internal stent, applying direct pressure to stop bleeding from the placental site.
- Surgical Intervention (Laparotomy):
- Uterine Compression Sutures: The B-Lynch suture is a common, effective technique.
- Vascular Ligation (Stepwise):
- Uterine artery ligation (O'Leary stitch).
- Internal iliac (hypogastric) artery ligation; reduces pulse pressure by ~85%.
- Hysterectomy: The definitive and final treatment when all other measures fail.
⭐ High-Yield: Internal iliac artery ligation is highly effective but carries a risk of ureteral injury due to anatomical proximity. It preserves uterine function.
High-Yield Points - ⚡ Biggest Takeaways
- Uterine atony is the most common cause of postpartum hemorrhage (PPH).
- First-line management is always bimanual uterine massage and a high-dose oxytocin infusion.
- If bleeding persists, administer second-line uterotonics like methylergonovine, carboprost, or misoprostol.
- Be aware of contraindications: avoid methylergonovine in hypertensive disorders and carboprost in asthma.
- Refractory cases may require intrauterine balloon tamponade, compression sutures (e.g., B-Lynch), or hysterectomy.
- Always ensure the bladder is empty to facilitate uterine contraction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

