Placenta Previa - Low-Lying Intruder
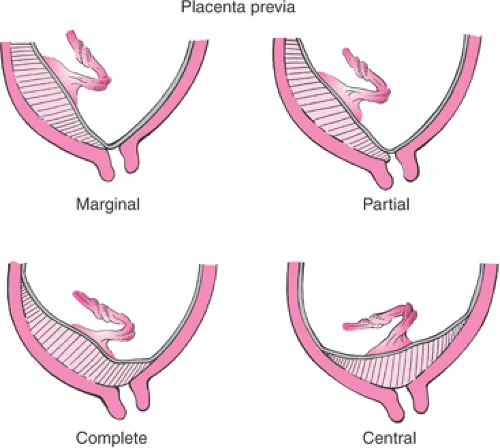
- Pathophysiology: Placenta implants over or near the internal cervical os. Types: complete, partial, marginal, or low-lying.
- Clinical Presentation: Sudden, painless, bright red vaginal bleeding, typically after 20 weeks gestation. Uterus is soft and non-tender.
- Risk Factors: Prior C-section, multiparity, advanced maternal age (>35), prior previa.
- Diagnosis & Management:
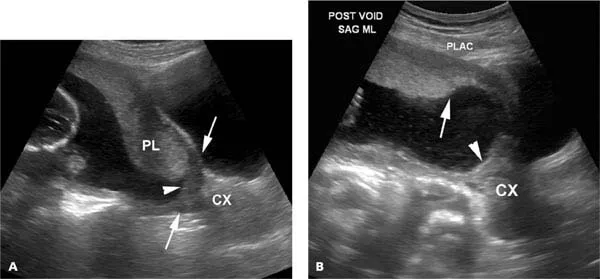
- Transvaginal ultrasound is the gold standard for diagnosis.
- ⚠️ NO digital vaginal or speculum exams.
- C-section delivery is indicated, usually at 36-37 weeks.
⭐ The classic triad is painless bleeding, a soft non-tender uterus, and reassuring fetal heart tones. Absence of pain is a key feature distinguishing it from placental abruption.
Risk Factors & Presentation - Red Alert Antepartum
-
Risk Factors:
- Prior C-section or other uterine surgery
- Multiparity & advanced maternal age (> 35 yrs)
- Cocaine use or smoking
- Prior placenta previa
-
Clinical Picture:
- Sudden, painless, bright red vaginal bleeding
- Typically occurs after 28 weeks gestation
- Uterus is soft, relaxed, and non-tender
- Fetal heart tones usually reassuring initially
⭐ Warning: Digital or speculum vaginal examination is absolutely contraindicated as it can provoke catastrophic hemorrhage. Diagnosis is made by ultrasound.
Diagnosis - Ultrasound Unveiling
- Initial Test: Transabdominal ultrasound.
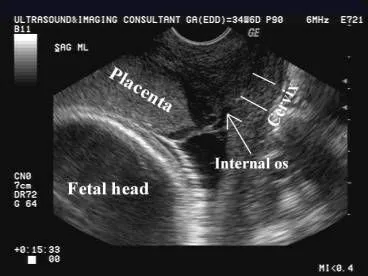
- Gold Standard: Transvaginal ultrasound (TVS) is safe & more accurate for precise localization.
- Follow-up: Repeat scan at ~32 weeks; many early previas resolve via "placental migration."
⭐ A digital vaginal exam is contraindicated if placenta previa is suspected until it has been ruled out by ultrasound.
Management - Watchful Waiting Game
- Indication: Preterm gestation (< 36-37 weeks) with a hemodynamically stable mother and reassuring fetal status.
- Core Strategy: Inpatient observation, especially after a bleeding episode.
- Key Interventions:
- Corticosteroids (Betamethasone): Administer if gestational age is < 34 weeks to promote fetal lung maturity.
- Strict Pelvic Rest: No vaginal exams (digital or speculum) and no intercourse.
- Tocolysis (e.g., Magnesium Sulfate): ⚠️ Used cautiously for short-term uterine quiescence, primarily to allow corticosteroids to take effect.
- Anemia Correction: Maintain maternal hematocrit > 30%.
⭐ Elective cesarean delivery is planned for 36 0/7 to 37 6/7 weeks, even in asymptomatic cases, to minimize the risk of hemorrhage from spontaneous labor.
Complications & Vasa Previa - Dangerous Liaisons
- Maternal: Risk of massive hemorrhage (may necessitate hysterectomy). Placenta accreta spectrum risk ↑ with prior C-sections.
- Fetal: Preterm birth, IUGR, and fetal anemia.
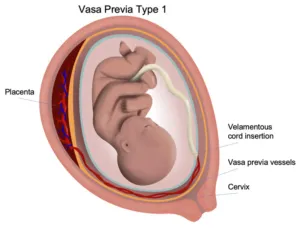
- Vasa Previa: A related emergency where unprotected fetal vessels run over the cervical os. Membrane rupture can tear these vessels, causing rapid fetal exsanguination.
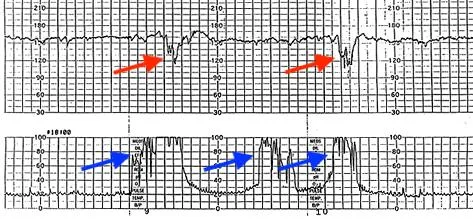
⭐ Vasa Previa Triad: Rupture of membranes, painless vaginal bleeding, and subsequent fetal bradycardia or a sinusoidal heart rate pattern.
High‑Yield Points - ⚡ Biggest Takeaways
- Painless, bright red vaginal bleeding in the third trimester is the classic presentation.
- The placenta implants over or near the internal cervical os.
- Major risk factors include prior cesarean delivery, multiparity, and advanced maternal age.
- Transvaginal ultrasound is the gold standard for diagnosis; transabdominal is used for initial screening.
- Digital vaginal examination is absolutely contraindicated due to the risk of catastrophic hemorrhage.
- Management is typically a planned cesarean delivery at 36-37 weeks.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

