Basics & Diagnosis - Two for One Deal
- Types:
- Dizygotic (Fraternal): 2 eggs, 2 sperm. Always dichorionic, diamniotic (Di-Di).
- Monozygotic (Identical): 1 egg, 1 sperm. Chorionicity depends on timing of division.
- Diagnosis: Ultrasound is key.
- Confirms number of fetuses.
- Determines chorionicity & amnionicity in 1st trimester.
- Di-Di: Twin peak / Lambda (λ) sign.
- Monochorionic-Diamniotic (Mo-Di): T-sign.
- Monochorionic-Monoamniotic (Mo-Mo): No separating membrane.
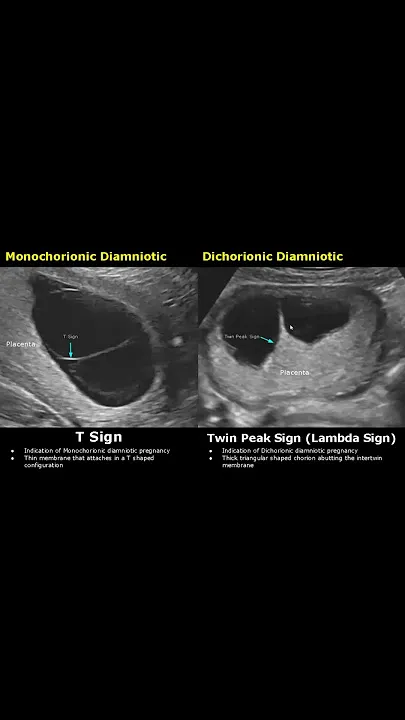
⭐ Determining chorionicity is the single most important factor in managing multiple gestations, as it predicts the risk of complications like Twin-Twin Transfusion Syndrome (TTTS).
Maternal Risks - More Than a Handful
- Systemic Overload: Nearly all pregnancy complications are more frequent and severe.
- Preeclampsia: Risk is 2-3x higher. Monitor BP and proteinuria closely.
- Gestational Diabetes (GDM): Increased placental mass ↑ human placental lactogen (hPL), leading to insulin resistance.
- Anemia: Exaggerated hemodilution. Requires higher iron/folate supplementation.
- Hemorrhage:
- Antepartum: ↑ risk of placenta previa & abruption.
- Postpartum (PPH): High risk from uterine atony due to overdistension.
- Preterm Labor: The single most common complication.
⭐ Uterine atony from overdistension is the leading cause of Postpartum Hemorrhage (PPH) in multiple gestation. Be prepared for active management of the third stage of labor.
Fetal Complications - Wombmate Woes
-
Universal Risks: Increased for all multiple gestations.
- Preterm birth (< 37 wks) & Low Birth Weight (LBW)
- Intrauterine Growth Restriction (IUGR)
- Congenital anomalies (2x baseline risk)
-
Monochorionic (MC) Syndromes: Due to placental vascular anastomoses.
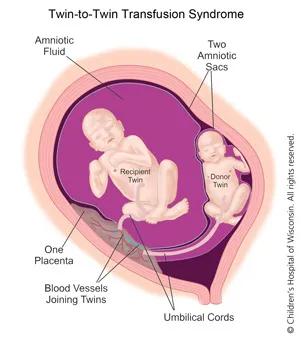
- Twin-Twin Transfusion (TTTS): Unbalanced blood flow.
- Donor: Anemic, oligohydramnios ("stuck" twin).
- Recipient: Polycythemic, polyhydramnios, hydrops.
- Twin Anemia-Polycythemia Sequence (TAPS): Slow flow causing large hemoglobin difference without fluid discrepancy.
- Selective IUGR (sIUGR): Unequal placental sharing → one twin <10th percentile.
- Twin Reversed Arterial Perfusion (TRAP): Acardiac twin perfused by pump twin; high mortality (>50%) for pump twin.
- Twin-Twin Transfusion (TTTS): Unbalanced blood flow.
⭐ TTTS Diagnosis: Requires monochorionic gestation + oligohydramnios (max vertical pocket [MVP] < 2 cm) in the donor's sac and polyhydramnios (MVP > 8 cm) in the recipient's sac.
Surveillance & Delivery - The Grand Exit
- Antepartum Surveillance:
- Serial growth US: q 4-6 wks (Di/Di), q 2 wks (Mo/Di & Mo/Mo).
- Antepartum testing (NST, BPP) weekly from 32-34 wks.
- Delivery Mode:
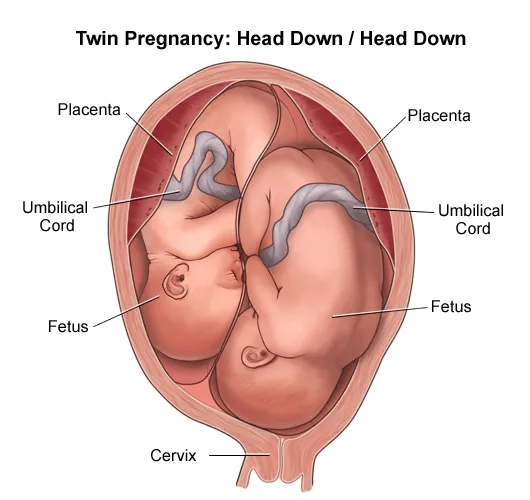
- Vaginal: Attempt if Twin A is vertex.
- Cesarean: Required for non-vertex Twin A, most Mo/Mo twins, and other standard OB indications.
⭐ Monochorionic-monoamniotic (Mo/Mo) twins require inpatient admission around 24-28 weeks for intensive fetal surveillance due to the high risk of cord entanglement, with a planned C-section at 32-34 weeks.
High-Yield Points - ⚡ Biggest Takeaways
- Chorionicity is the single most important prognostic factor; monochorionic twins are at unique risk for Twin-to-Twin Transfusion Syndrome (TTTS).
- Early ultrasound is critical to establish chorionicity and amnionicity, which dictates the entire surveillance schedule.
- Expect a higher incidence of maternal complications, especially pre-eclampsia, gestational diabetes, and anemia.
- Preterm labor is the most common complication; have a low threshold to administer antenatal corticosteroids.
- Delivery is planned earlier than singletons, with timing based on chorionicity and complications (32-38 weeks).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

