Systemic Lupus Erythematosus (SLE) - The Great Imitator
- Maternal Risks: Disease flares (especially postpartum), lupus nephritis, ↑ risk of preeclampsia, thromboembolism, and maternal mortality.
- Fetal Risks: Miscarriage, Intrauterine Growth Restriction (IUGR), preterm birth, and stillbirth.
- Neonatal Lupus Syndrome:
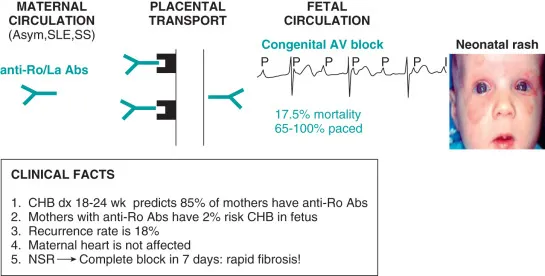
- Caused by passive placental transfer of maternal anti-Ro/SSA and/or anti-La/SSB antibodies.
- Manifests as transient skin rash, hematologic abnormalities, or permanent congenital heart block (CHB).
- Management:
- Pre-conception: Plan pregnancy during disease remission (ideally >6 months).
- Antepartum: Continue Hydroxychloroquine (HCQ) to prevent flares. Start low-dose aspirin (LDA) by 12 weeks to reduce preeclampsia risk.
⭐ The presence of anti-Ro/SSA antibodies carries a 1-2% risk for congenital heart block; this risk increases to ~20% in subsequent pregnancies if a prior child was affected.
Antiphospholipid Syndrome (APS) - Clots & Losses
- Pathophysiology: Prothrombotic autoimmune state where antibodies target cell membrane phospholipids, leading to hypercoagulability.
- Diagnostic Criteria (Sapporo):
- Clinical (≥1): Vascular thrombosis OR pregnancy morbidity (≥3 losses <10 wks; ≥1 loss >10 wks; premature birth <34 wks due to eclampsia/placental insufficiency).
- Lab (≥1, on 2 occasions >12 wks apart): Lupus anticoagulant, Anti-cardiolipin IgG/IgM, Anti-β2 glycoprotein I IgG/IgM.
- Management: Low-dose aspirin (LDA) + prophylactic heparin (LMWH).
⭐ Paradoxical Lab Finding: APS can cause a prolonged aPTT in vitro (due to interference by lupus anticoagulant) but causes thrombosis in vivo.
RA, Thyroid & More - Rogues' Gallery
-
Rheumatoid Arthritis (RA):
- Often improves during pregnancy.
- Safe meds: Hydroxychloroquine, Sulfasalazine.
- ⚠️ AVOID Methotrexate (teratogen).
-
Thyroid Disorders:
- Graves' (Hyper): Maternal TSH-receptor Abs (TSI) cross placenta → fetal thyrotoxicosis. Tx: PTU (1st tri), then Methimazole.
- Hashimoto's (Hypo): ↑ risk of miscarriage, preeclampsia. Monitor TSH; ↑ Levothyroxine dose is common.
-
Myasthenia Gravis:
- AChR-Abs can cause transient neonatal myasthenia.
- ⚠️ AVOID Magnesium Sulfate (can trigger myasthenic crisis).
-
Sjögren's Syndrome:
- Associated with Anti-Ro (SSA) & Anti-La (SSB) antibodies.
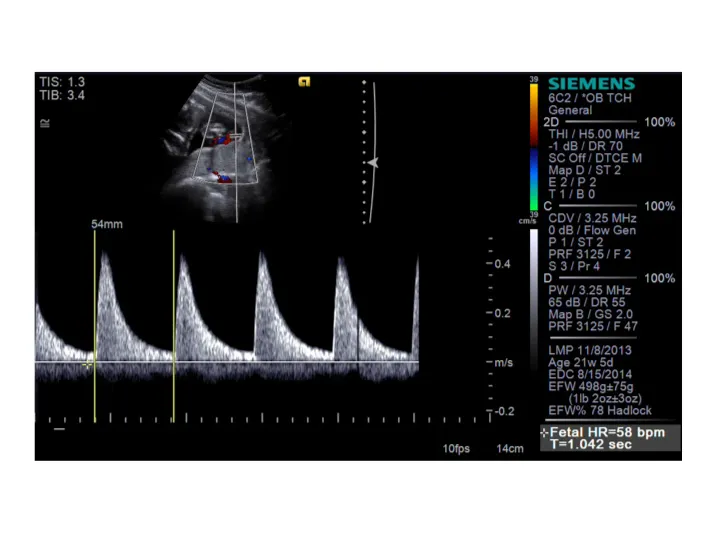
⭐ Presence of anti-Ro/SSA antibodies confers a 1-2% risk of fetal congenital heart block, which can be detected by fetal echocardiography.
Pregnancy Pharmacopoeia - Safe Meds Guide
- Goal: Use lowest effective dose; multidisciplinary management is key.
- Biologics (TNF-α inhibitors): Generally safe, but often stopped in the 3rd trimester to reduce neonatal infection risk.
⭐ Hydroxychloroquine is crucial and safe to continue in pregnant SLE patients; it reduces the risk of cardiac and cutaneous neonatal lupus and maternal flares.
High-Yield Points - ⚡ Biggest Takeaways
- SLE flares are common postpartum; hydroxychloroquine is protective and safe throughout pregnancy.
- Anti-Ro/SSA and Anti-La/SSB antibodies are linked to congenital heart block.
- Antiphospholipid syndrome (APS) requires low-dose aspirin and heparin to prevent thrombosis and pregnancy loss.
- Rheumatoid arthritis often improves during pregnancy, while SLE tends to worsen.
- Avoid magnesium sulfate in mothers with Myasthenia Gravis to prevent a myasthenic crisis.
- Maternal Graves' disease can cause fetal thyrotoxicosis via placental transfer of TSI antibodies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

