HPV Overview - The Viral Culprit
- Structure: Non-enveloped, circular dsDNA virus with an icosahedral capsid. Highly epitheliotropic, infecting basal keratinocytes.
- Transmission: Primarily via direct contact (sexual, skin-to-skin).
- Subtypes & Risk:
- High-Risk (Oncogenic): 16, 18, 31, 33. Associated with cervical, anogenital, and oropharyngeal squamous cell carcinoma.
- Low-Risk (Benign): 6, 11. Cause condylomata acuminata (anogenital warts).
- Key Oncoproteins:
- E6 → Degrades p53 (prevents apoptosis).
- E7 → Inhibits pRb (promotes cell cycle progression).
⭐ Integration of high-risk HPV DNA into the host genome is a key event in malignant transformation. This disrupts the viral E2 gene, which normally represses the E6/E7 oncogenes.
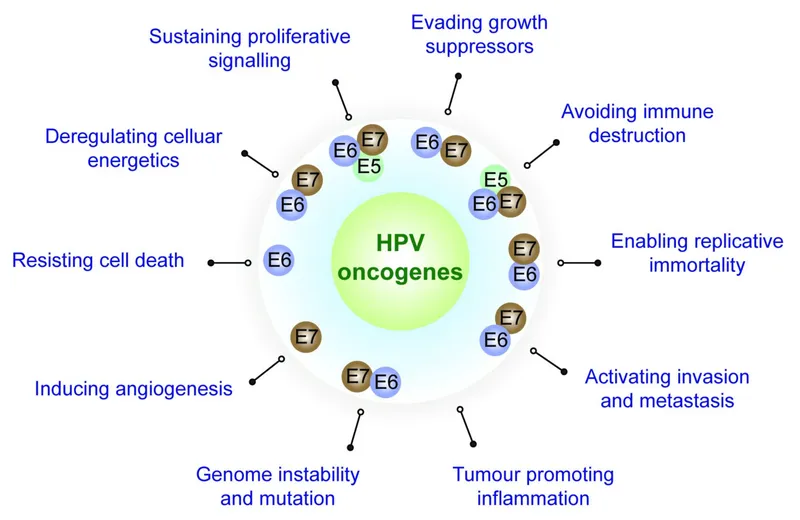
Oncogenesis - Hijacking the Cell
- Viral Proteins Drive Malignancy: High-risk HPV (hrHPV) integrates its DNA into the host genome, leading to persistent expression of oncoproteins E6 and E7.
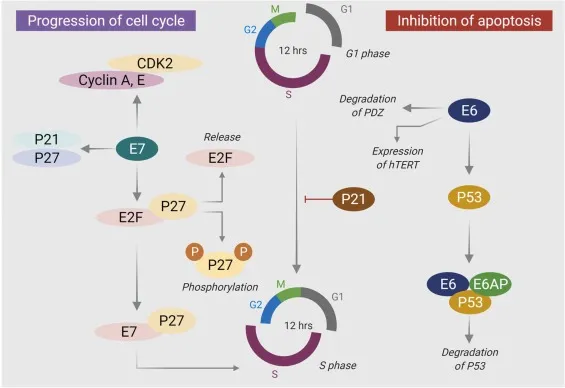
- E6 Protein Action:
- Binds to and promotes the degradation of the p53 tumor suppressor protein via the ubiquitin-proteasome pathway.
- This blocks apoptosis and cell cycle arrest, allowing damaged cells to proliferate.
- E7 Protein Action:
- Binds to and inactivates the retinoblastoma (Rb) tumor suppressor protein.
- This releases the E2F transcription factor, pushing the cell from G1 to S phase.
⭐ HPV types 16 and 18 are responsible for ~70% of all cervical cancers and a significant portion of other HPV-associated cancers.
Clinical Disease - Cancers & Warts
-
Malignancies (High-Risk Serotypes): Associated with HPV types 16, 18, 31, 33.
- Driven by oncoproteins: E6 (degrades tumor suppressor p53) and E7 (inhibits tumor suppressor Rb).
- Cervical Carcinoma: Most common HPV-associated cancer.
- Also causes squamous cell carcinoma of the anus, vagina, vulva, penis, and oropharynx.
-
Benign Lesions (Low-Risk Serotypes): Caused by HPV types 6 and 11.
- Condylomata acuminata: Anogenital warts with a cauliflower-like appearance.
- Laryngeal Papillomatosis: Benign tumors in the larynx, can cause airway obstruction.
⭐ The E6 protein from high-risk HPV promotes the degradation of p53, while the E7 protein inactivates the retinoblastoma (Rb) protein, leading to uncontrolled cell cycle progression.
Prevention & Screening - Guarding the Gates
-
Primary Prevention: Vaccination
- Gardasil 9 (9-valent HPV vaccine) is key.
- Routinely recommended at age 11-12; can be given from age 9 up to 45.
- Covers HPV types 6, 11 (genital warts) and high-risk types 16, 18, 31, 33, 45, 52, 58.
-
Secondary Prevention: Screening
- Detects precancerous lesions before they become invasive cancer.
- Methods: Pap test (cytology) & HPV DNA testing.
⭐ Pap smears begin at age 21, regardless of sexual activity onset. Co-testing (Pap + HPV DNA) is the preferred screening method for women aged 30-65.
High‑Yield Points - ⚡ Biggest Takeaways
- High-risk HPV types (16, 18) are the main cause of cervical, anogenital, and oropharyngeal cancers.
- The viral oncoprotein E6 degrades the p53 tumor suppressor, while E7 inactivates the retinoblastoma (Rb) protein.
- This disruption of key tumor suppressors bypasses cell cycle checkpoints, leading to malignant growth.
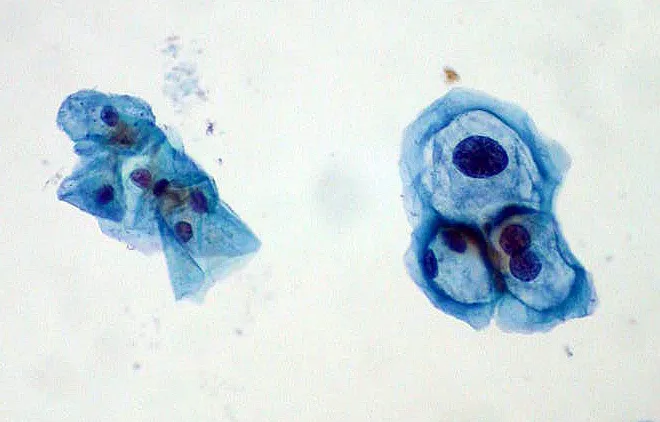
- Koilocytes-squamous epithelial cells with a wrinkled nucleus and a perinuclear halo-are pathognomonic on Pap smears.
- Primary prevention via the HPV vaccine is highly effective.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

