Prevention Pillars - Rogues' Gallery
- Primary Prevention (Vaccination): Pre-empts infection.
- HPV (Gardasil 9)
- HBV
- Secondary Prevention (Screening): Catches early changes.
- Pap smear (HPV)
- HCV antibody tests
- Risk Reduction & Treatment: Limits exposure & viral effects.
- Safe sex (HHV-8, HIV)
- Blood product screening (HCV, HTLV-1)
- Antivirals (HBV, HCV, HIV)
⭐ The HPV vaccine prevents over 90% of cervical cancers. It is ideally administered at ages 11-12, but approved for individuals up to age 45.
Vaccination - Prophylactic Power-ups
- Primary Prevention: Vaccines are a cornerstone strategy to prevent cancers caused by viruses, targeting them before they can establish chronic infection.
- Hepatitis B (HBV) Vaccine:
- Mechanism: Recombinant vaccine containing Hepatitis B surface antigen (HBsAg).
- Prevents: Hepatocellular carcinoma (HCC) by preventing chronic HBV infection.
- Schedule: Routinely administered to all infants in a 3-dose series starting at birth.
- Human Papillomavirus (HPV) Vaccine:
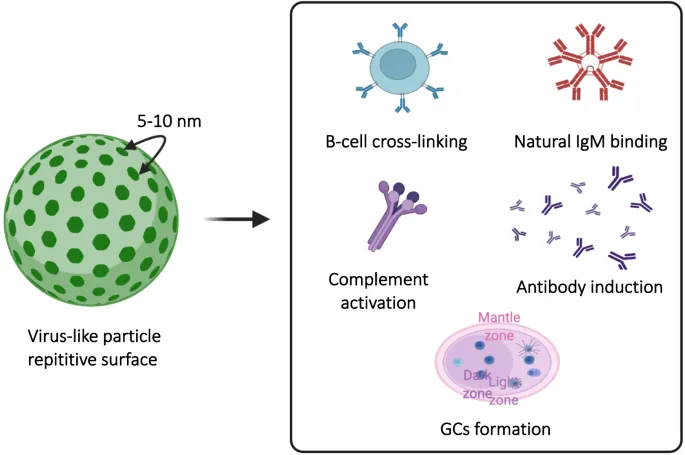
- Mechanism: Composed of L1 capsid proteins that self-assemble into non-infectious virus-like particles (VLPs).
- Spectrum: Gardasil 9 targets 9 types (high-risk 16, 18, 31, 33, 45, 52, 58; low-risk 6, 11).
- Prevents: Cancers of the cervix, anus, oropharynx, penis, vulva, and vagina.
- Schedule: Recommended for ages 11-12; can be given up to age 45 based on shared clinical decision-making.
⭐ High-Yield Pearl: HPV vaccines are prophylactic, not therapeutic. They are highly effective at preventing new infections but do not clear existing HPV infections or treat HPV-associated lesions.
Screening & Treatment - Damage Control
-
Human Papillomavirus (HPV):
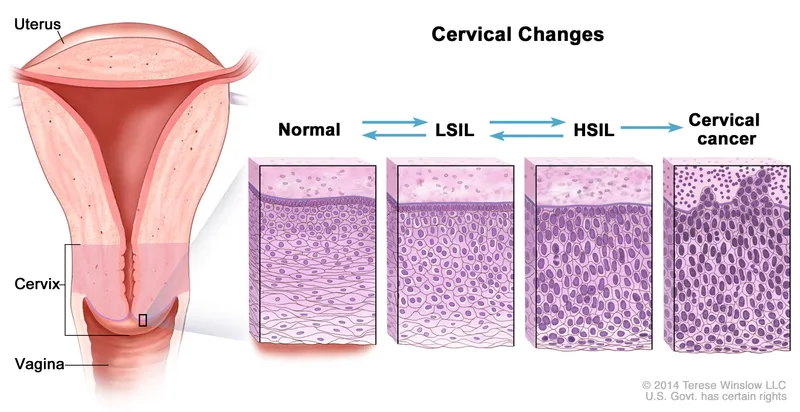
- Screening: Pap test (cervical cytology) & HPV DNA testing.
- Protocols: Begin at age 21. Pap test every 3 years, or HPV co-testing every 5 years for ages 30-65.
- Management: Abnormal results trigger colposcopy with biopsy. High-grade cervical intraepithelial neoplasia (CIN) is treated with Loop Electrosurgical Excision Procedure (LEEP) or ablation to prevent progression to invasive carcinoma.
-
Hepatitis B (HBV) & C (HCV):
- HCC Surveillance: In patients with chronic infection or cirrhosis, screen with liver ultrasound ± alpha-fetoprotein (AFP) every 6 months.
- Treatment: Antiviral therapy (e.g., Tenofovir for HBV, DAAs for HCV) suppresses viral replication, reduces hepatic inflammation, and significantly lowers the risk of developing hepatocellular carcinoma.
-
EBV & HHV-8:
- No routine screening protocols exist. Diagnosis relies on clinical presentation and tissue biopsy of suspected malignancies (e.g., Kaposi sarcoma, nasopharyngeal carcinoma).
⭐ Treatment of Hepatitis C with Direct-Acting Antivirals (DAAs) achieves a sustained virologic response (cure) in >95% of patients, dramatically reducing the long-term risk of hepatocellular carcinoma.
High‑Yield Points - ⚡ Biggest Takeaways
- HPV vaccination (Gardasil, Cervarix) is the primary prevention for cervical, anogenital, and oropharyngeal cancers.
- HBV vaccination is highly effective in preventing hepatocellular carcinoma (HCC).
- Treating chronic HCV with direct-acting antivirals (DAAs) cures the infection and dramatically reduces HCC risk.
- Cervical cancer screening using Pap smears and HPV testing is critical for secondary prevention.
- Managing immunosuppression is key to preventing EBV and HHV-8 associated malignancies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

