Vaginal Flora - Lactobacillus Land
- Primary Colonizers: Predominantly Lactobacillus species (L. crispatus, L. iners).
- Protective Acid Shield:
- Metabolize glycogen from epithelial cells to produce lactic acid ($C_3H_6O_3$).
- Maintains an acidic vaginal pH (< 4.5), which is hostile to most pathogens.
- Some strains also produce H₂O₂ to suppress anaerobic bacteria.
- Flora Disruption: A decrease in Lactobacillus can lead to:
- Bacterial Vaginosis (BV): Overgrowth of anaerobes (e.g., Gardnerella vaginalis).
- Candidiasis: Fungal overgrowth (e.g., Candida albicans).
⭐ High estrogen levels promote glycogen deposition in the vaginal epithelium, fostering a healthy Lactobacillus-dominant microbiome. This is why pre-pubertal and post-menopausal women are more susceptible to vaginal infections.
Hormonal Axis - Estrogen's Empire
-
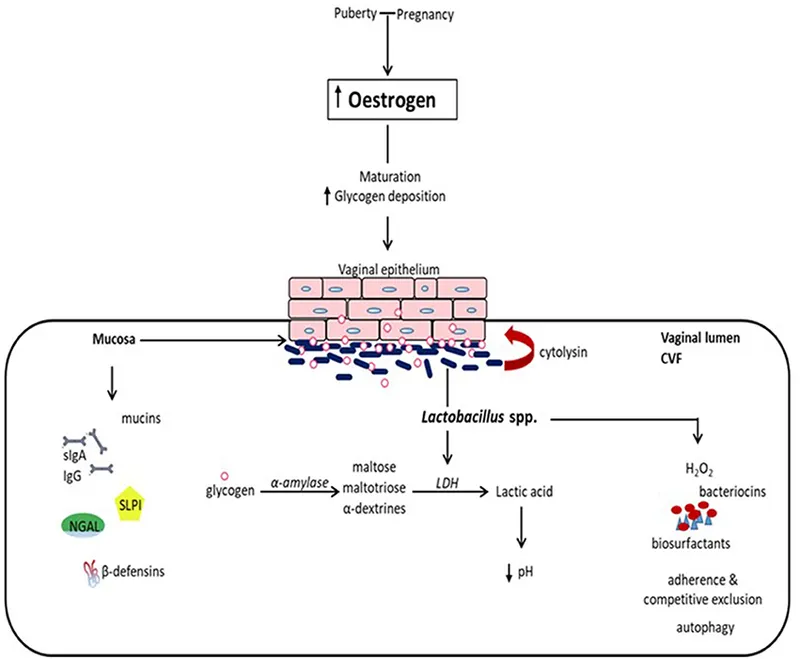
Estrogen's Role: The primary driver of a healthy vaginal ecosystem.
- ↑ Estrogen levels promote the maturation and glycogenation of the vaginal epithelium.
- Lactobacillus species metabolize this glycogen into lactic acid.
- This creates an acidic vaginal environment (pH < 4.5), which inhibits the growth of pathogenic microbes.
-
Hormonal Fluctuations:
- Pre-puberty & Post-menopause: ↓ Estrogen → ↓ glycogen → ↑ vaginal pH. This increases susceptibility to infections like bacterial vaginosis and atrophic vaginitis.
- Reproductive Years: Cyclical estrogen maintains a protective, acidic state.
⭐ High-Yield: In low-estrogen states (e.g., menopause), the vaginal pH rises >4.5, creating a favorable environment for pathogens like E. coli, leading to recurrent UTIs and vaginitis.
Dysbiosis Drama - When Guards Go Down
-
The Shift: A decline in protective Lactobacillus species is the central event, disrupting the vaginal ecosystem's balance.
-
Primary Triggers:
- Broad-spectrum antibiotics (e.g., clindamycin, amoxicillin)
- Douching, spermicides
- Hormonal shifts (menstruation, pregnancy, menopause)
-
The Cascade: ↓ Lactobacillus → ↓ Lactic acid production → ↑ Vaginal pH > 4.5 → Pathogen overgrowth.
- Key Conditions:
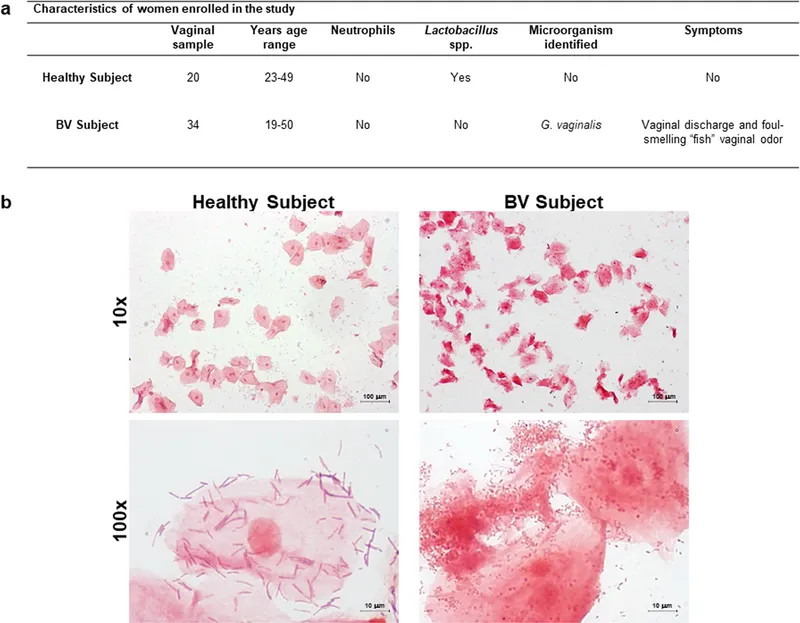
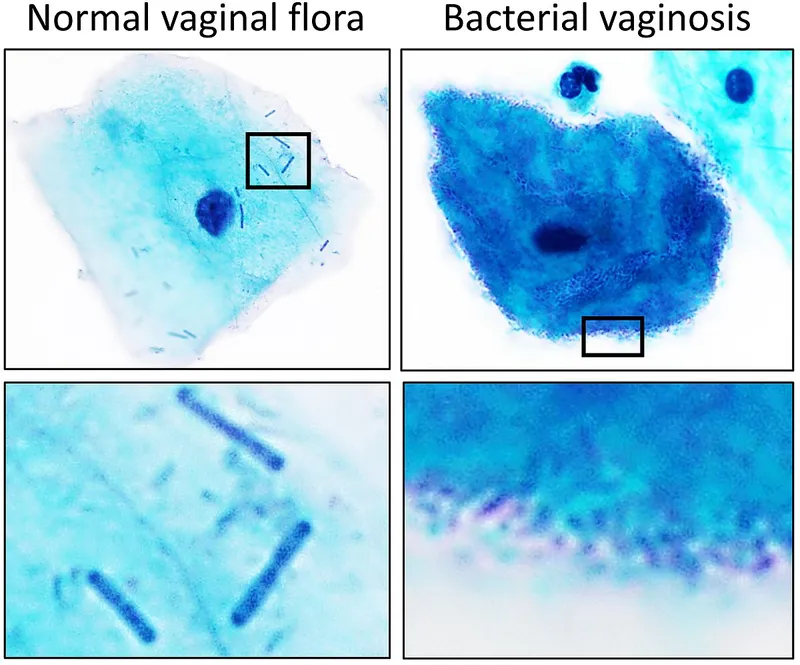
- Bacterial Vaginosis (BV): Polymicrobial overgrowth, primarily Gardnerella vaginalis. Presents with thin, grey-white discharge and a "fishy" odor. Diagnosed by clue cells on microscopy.
- Vulvovaginal Candidiasis (VVC): Overgrowth of Candida albicans. Thick, white, "cottage cheese" discharge and intense pruritus. Normal pH.
⭐ Exam Favorite: Diagnosis of Bacterial Vaginosis often relies on the Amsel Criteria. Requires 3 of 4:
- Thin, white, homogenous discharge.
- Vaginal pH > 4.5.
- Positive whiff-amine test.
- Clue cells on microscopy.
Male Microbiome - A Quick Tour
- Distal Urethra: Primarily skin & gut commensals.
- Staphylococcus epidermidis, Enterococcus faecalis, Corynebacteria, Lactobacilli.
- Coronal Sulcus (Uncircumcised): Rich in anaerobic bacteria (Prevotella, Porphyromonas).
- Semen: Generally low bacterial biomass, reflecting urethral flora.
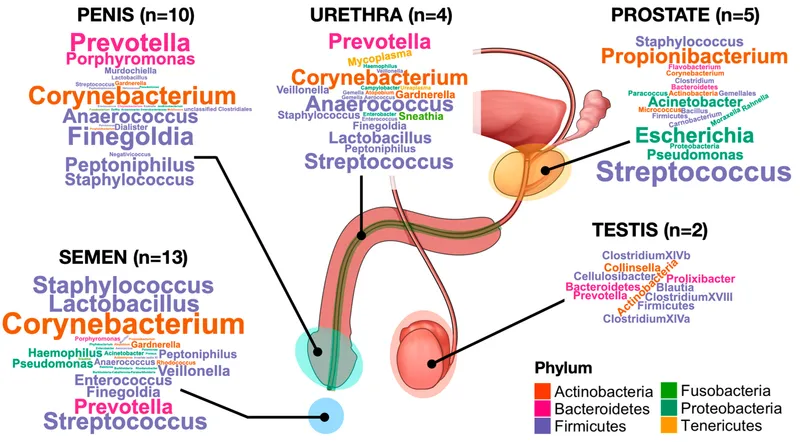
⭐ Circumcision significantly reduces anaerobic bacteria in the coronal sulcus. This microbial shift is linked to a lower risk for HIV and HPV acquisition.
High‑Yield Points - ⚡ Biggest Takeaways
- Lactobacillus is the dominant microbe in a healthy vagina, producing lactic acid to maintain an acidic pH (< 4.5).
- Estrogen promotes glycogen, which Lactobacillus metabolizes, linking hormonal status to vaginal health.
- Bacterial Vaginosis (BV) is a dysbiosis, a shift from Lactobacillus to anaerobes like Gardnerella vaginalis.
- An elevated vaginal pH (> 4.5) is a key indicator of BV or trichomoniasis.
- The upper urinary tract (bladder, kidneys) is normally sterile.
- Candida albicans overgrowth, often post-antibiotics, causes candidiasis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

