GI Microbiome - The Gut Garden

- Composition: Predominantly anaerobic bacteria. Key phyla: Bacteroidetes (G-), Firmicutes (G+). ↑Firmicutes/Bacteroidetes ratio linked to obesity.
- Core Functions:
- Metabolic: Ferments fiber into Short-Chain Fatty Acids (SCFAs). Synthesizes Vitamin K and B vitamins (biotin, folate).
- Immune: Competitively inhibits pathogens. Essential for maturing Gut-Associated Lymphoid Tissue (GALT).
- Dysbiosis (Imbalance):
- Antibiotics (e.g., clindamycin) risk Clostridioides difficile overgrowth.
- Associated with IBD, obesity, and allergies.
⭐ Butyrate, a key SCFA, is the primary fuel for colonocytes and has anti-inflammatory effects.
Core Functions - Microbial Metabolism
- Carbohydrate Fermentation:
- Anaerobic breakdown of indigestible dietary fiber (e.g., cellulose, pectin) into Short-Chain Fatty Acids (SCFAs).
- Key SCFAs:
- Butyrate: Preferred energy source for colonocytes; strengthens gut barrier.
- Propionate: Hepatic gluconeogenesis substrate.
- Acetate: Enters peripheral circulation; used in muscle & adipose tissue.
- Vitamin Synthesis:
- Production of essential vitamins unavailable from diet alone.
- Includes Vitamin K (crucial for coagulation factors) and B vitamins like Biotin (B7) and Folate (B9).
- Bile Acid Metabolism:
- Deconjugation and conversion of primary bile acids into secondary bile acids (e.g., deoxycholic acid).
⭐ Gut microbiota can metabolize and inactivate drugs, altering bioavailability. A classic example is the bacterial inactivation of Digoxin, reducing its therapeutic effect in susceptible individuals.

Dysbiosis - When Flora Fails
- Definition: Disruption of the normal gut microbial community's composition, function, or diversity, often triggered by antibiotics, diet, or illness.
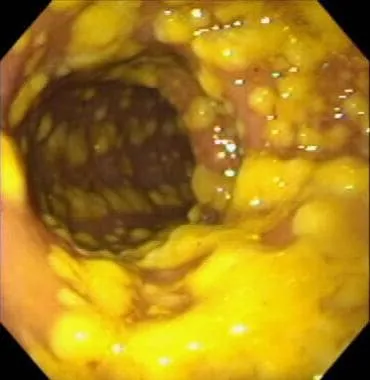
- Classic Example: Clostridioides difficile Infection
- Antibiotic use (esp. clindamycin, cephalosporins, fluoroquinolones) depletes protective flora, allowing C. diff overgrowth.
- Toxin A (enterotoxin) and Toxin B (cytotoxin) lead to mucosal injury, inflammation, and formation of pseudomembranes.
- Results in profuse, watery diarrhea, abdominal cramping, and potential toxic megacolon.
- Therapeutic Interventions
- Probiotics: Administration of live beneficial bacteria (e.g., Lactobacillus).
- Prebiotics: Substrates (e.g., inulin) that promote growth of beneficial bacteria.
- Fecal Microbiota Transplant (FMT): Highly effective for recurrent C. diff by restoring a healthy, diverse microbiome.
⭐ Diagnosis of C. difficile relies on detecting toxins A/B in the stool via enzyme immunoassay (EIA) or nucleic acid amplification tests (NAAT).
Therapeutics - Gut Reset Button
- Antibiotics: Broad-spectrum use disrupts flora → dysbiosis, ↑ risk of C. difficile infection (CDI).
- Probiotics: Live beneficial bacteria (Lactobacillus, Bifidobacterium) to restore balance. Limited efficacy for severe dysbiosis.
- Prebiotics: Dietary fibers (e.g., inulin) that fuel beneficial microbes, promoting a healthy gut environment.
- Fecal Microbiota Transplant (FMT): Infusion of stool from a healthy donor to restore a complex, healthy microbiome.
⭐ Fecal Microbiota Transplant (FMT) is a highly effective therapy for recurrent Clostridioides difficile infection, with cure rates often exceeding 90%.

- Anaerobes like Bacteroides and Clostridium are the most predominant organisms in the colon.
- Gut flora are a primary source of Vitamin K and several B vitamins.
- They are essential for the metabolism of bile acids and the breakdown of bilirubin.
- Provide colonization resistance against pathogens, most notably C. difficile.
- Crucial for the development and maturation of gut-associated lymphoid tissue (GALT).
- Antibiotic use disrupts this barrier, increasing infection risk.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

