HBV Virology & Transmission - The Viral Blueprint
- Virology: An enveloped virus from the Hepadnaviridae family. It has a unique partially double-stranded circular DNA genome and notably encodes a reverse transcriptase for its replication cycle.
- Transmission: Spread through parenteral (IV drug use, needlesticks), sexual, and perinatal (vertical) routes. 📌 Mnemonic: B for Blood, Birthing, and Bonking (sexual contact).
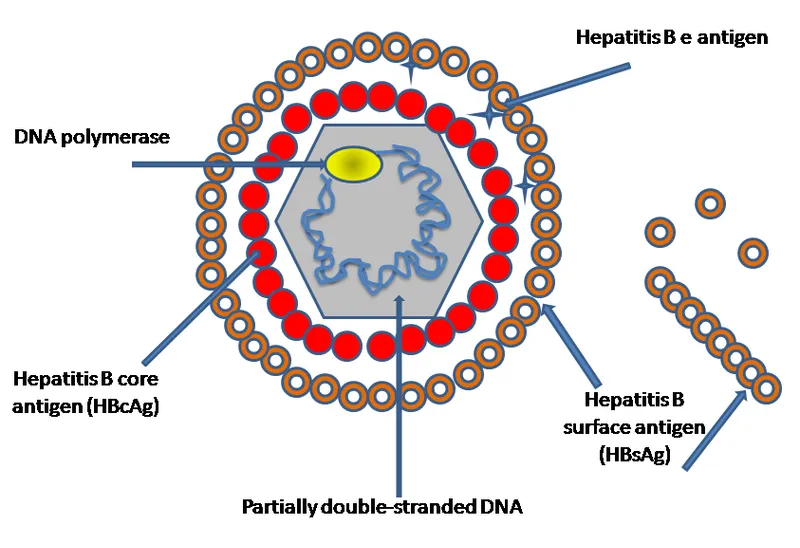
⭐ HBV is the only human DNA virus that replicates via a reverse transcriptase, a key target for antiviral therapy.
Clinical & Pathophysiology - The Host Response
- Incubation Period: 1-4 months.
- Clinical Phases:
- Prodrome (Serum Sickness-Like Syndrome): Fever, rash, and arthralgia often precede jaundice due to immune complex deposition.
- Icteric Phase: Jaundice, RUQ pain, hepatomegaly, dark urine (bilirubinuria), and pale stools (acholic stools).
- Pathophysiology: Liver injury is not directly cytopathic. It is immune-mediated by CD8+ T-cells attacking hepatocytes that express viral antigens.
⭐ The severity of acute illness reflects the vigor of the host's immune response, not the viral load. A strong response causes more damage but effectively clears the virus.
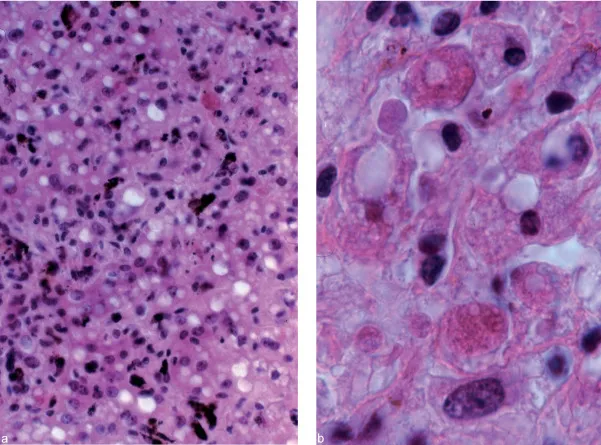
- Histology Findings:
- Acute: Panlobular inflammation, ballooning degeneration, and Councilman bodies (apoptotic hepatocytes).
- Chronic: "Ground-glass" hepatocytes (HBsAg accumulation in cytoplasm).
Serological Markers - Decoding the Blood
- HBsAg (Surface Antigen): The very first marker to appear in the blood. Its presence indicates an active, ongoing Hepatitis B infection.
- HBeAg (e Antigen): Appears shortly after HBsAg. A key indicator of active viral replication and high infectivity.
- Anti-HBc IgM (Core Antibody): The first antibody to become detectable. It is the most reliable marker for diagnosing an acute infection.
- Window Period: A critical diagnostic gap where HBsAg has disappeared, but the protective Anti-HBs has not yet formed. During this time, Anti-HBc IgM is the sole indicator of a recent infection.
- Anti-HBe: Appearance signifies seroconversion, marking a decrease in viral replication and infectivity.
- Anti-HBs (Surface Antibody): Its presence indicates recovery and protective immunity. This is the goal of vaccination.
- Anti-HBc IgG: Replaces Anti-HBc IgM and persists for life, serving as a marker of past infection.
⭐ The first and most reliable marker of acute Hepatitis B infection is Anti-HBc IgM.
Diagnosis & Management - The Game Plan
- Diagnosis: Suspect clinically; confirm with serology showing positive HBsAg and Anti-HBc IgM.
- Management: Primarily supportive care. Antivirals (e.g., tenofovir) are reserved for severe, fulminant hepatitis.
- Post-Exposure Prophylaxis (PEP): Administer Hepatitis B Immune Globulin (HBIG) and the HBV vaccine series.
- Prognosis: Excellent in adults, with >95% achieving complete recovery.
⭐ The risk of developing chronic HBV is inversely proportional to the age of infection: ~90% for neonates vs. <5% for immunocompetent adults.
High-Yield Points - ⚡ Biggest Takeaways
- Acute Hepatitis B is a DNA virus, primarily transmitted via parenteral, sexual, and perinatal routes.
- The hallmark of acute infection is the presence of HBsAg and anti-HBc IgM.
- HBeAg is a key indicator of active viral replication and high infectivity.
- The "window period" may show only anti-HBc IgM as positive.
- Anti-HBs without other markers signifies immunity from vaccination.
- Over 95% of infected adults achieve spontaneous recovery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

