Strep Pneumo - The Rusty Captain
- Identity: Gram-positive, lancet-shaped diplococcus.
- Lab ID: Catalase-negative, α-hemolytic, optochin-sensitive, and bile-soluble.
- Virulence: Key factor is its polysaccharide capsule, which is antiphagocytic.
- Clinical: Remember MOPS - most common cause of Meningitis, Otitis media (in children), Pneumonia, and Sinusitis.
⭐ Classic presentation of pneumococcal pneumonia includes the production of "rusty" (blood-tinged) sputum.
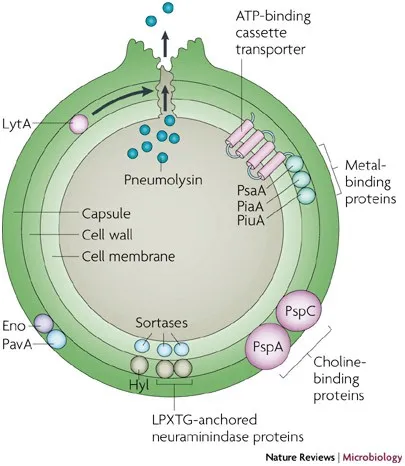
Virulence Factors - Armor & Dagger
- Polysaccharide capsule: Primary armor. Antiphagocytic, with over 90 serotypes. This is the basis for pneumococcal vaccines (PCV, PPSV).
- IgA protease: Dagger at mucosal sites. Cleaves secretory IgA, allowing epithelial attachment and invasion.
- Pneumolysin: A cytotoxin that creates pores in host cells, damages respiratory cilia, and suppresses phagocyte function.
⭐ The polysaccharide capsule is the basis of the Quellung reaction, where antisera cause the capsule to swell, making it visible under a microscope.
📌 Mnemonic: Pneumococcus Protects with Polysaccharide.
Clinical Disease - A MOPS of Trouble
📌 MOPS is the classic mnemonic for diseases caused by S. pneumoniae.
- Meningitis: Most common cause in adults.
- Otitis media: Most common cause in children.
- Pneumonia: Leading cause of community-acquired pneumonia (CAP).
- Presents as a typical lobar pneumonia.
- Characterized by "rusty" sputum.
- Sinusitis: A frequent bacterial cause.
Also a primary cause of life-threatening sepsis in asplenic patients.
⭐ Viral infections, especially influenza, are a major predisposing factor for subsequent S. pneumoniae pneumonia.
Diagnosis - The Telltale Signs
- Culture: α-hemolytic (partial, green hemolysis) colonies on blood agar.
- Quellung Reaction: Capsule swells upon adding specific antiserum.
- Rapid Diagnosis: Urine antigen test for pneumococcal pneumonia.
⭐ Optochin sensitivity is the key test to differentiate S. pneumoniae (Sensitive) from other α-hemolytic streptococci like S. viridans (Resistant).
Treatment & Prevention - The Counterattack
-
Treatment
- Empiric therapy: Ceftriaxone, macrolides.
- Penicillin-sensitive strains: Penicillin G.
- Meningitis: Vancomycin + Ceftriaxone.
- ⚠️ Note rising penicillin resistance due to altered penicillin-binding proteins (PBPs).
-
Prevention: Vaccination
| Vaccine | Type | Mechanism | Key Population |
|---|---|---|---|
| PCV13 | Conjugate | T-cell dependent; robust response | Infants, adults >65 |
| PPSV23 | Polysaccharide | T-cell independent; less immunogenic | Adults >65, high-risk individuals >2 |
High‑Yield Points - ⚡ Biggest Takeaways
- Lancet-shaped gram-positive diplococci; displays alpha-hemolysis.
- The major virulence factor is its polysaccharide capsule.
- It is optochin-sensitive and bile-soluble.
- The most common cause of MOPS: Meningitis, Otitis media, Pneumonia, and Sinusitis.
- Pneumonia classically presents with "rust-colored" sputum.
- Asplenic patients are at a significantly increased risk for sepsis.
- Prevention is primarily achieved through pneumococcal vaccination.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

