C. jejuni - The Gutsy Glider
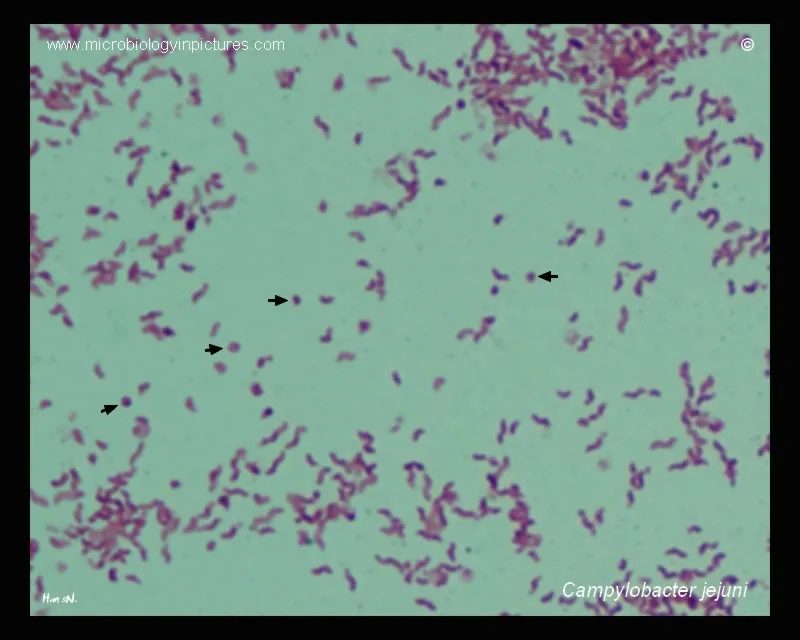
- Gram-negative, motile, curved (S-shaped or “gull-wing”) rod; oxidase ⊕.
- Thrives in heat (thermophilic) at 42°C and low oxygen (microaerophilic).
- Source: Undercooked poultry, unpasteurized milk, pets (puppies).
- Clinical: Common cause of invasive, inflammatory, bloody diarrhea.
⭐ Guillain-Barré Syndrome (GBS): Ascending paralysis triggered by autoimmune cross-reactivity with lipooligosaccharides. A major post-infectious sequela.
Pathogenesis - Invasion Games
- Adhesion & Motility: Utilizes adhesin protein CadF to bind to fibronectin and polar flagella for corkscrew motility to penetrate intestinal mucus.
- Invasion: Invades enterocytes in the jejunum, ileum, and colon via endocytosis, surviving within vacuoles.
- Toxin-Mediated Damage: Releases Cytolethal Distending Toxin (CDT), an A-B toxin.
- CDT's B subunit binds to the cell.
- CDT's A subunit (CdtB) acts as a DNase, causing dsDNA breaks, leading to cell cycle arrest in G2/M phase and apoptosis.
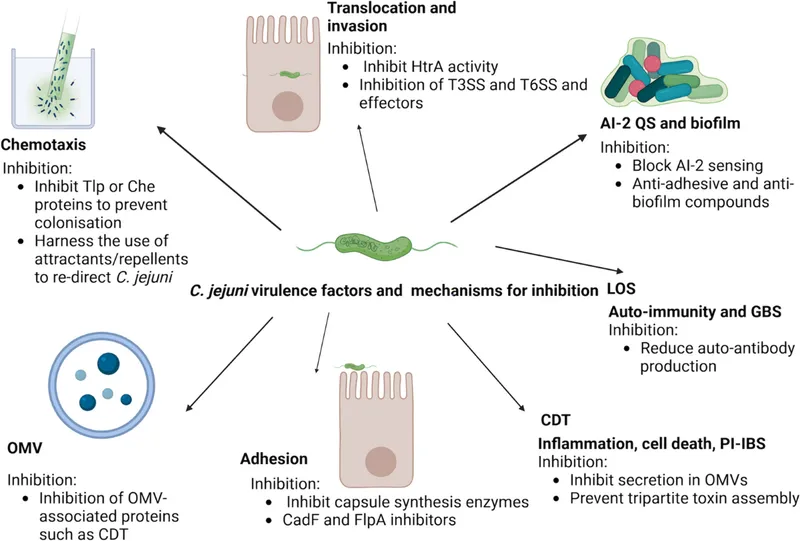
⭐ Molecular Mimicry: C. jejuni's lipooligosaccharide (LOS) can mimic human gangliosides (e.g., GM1), triggering autoimmune cross-reactivity that leads to Guillain-Barré syndrome (GBS).
Clinical Features - Gut Punch & Nerve Pinch
-
Gastroenteritis (Acute Enteritis):
- Incubation: 1-3 days.
- Prodrome: Fever, headache, myalgias.
- Main symptoms: Severe, crampy abdominal pain (can mimic appendicitis) followed by profuse, watery, and frequently bloody diarrhea (≥10 stools/day).
- Usually self-limiting within one week.
-
Post-Infectious Sequelae (1-3 weeks post-infection):
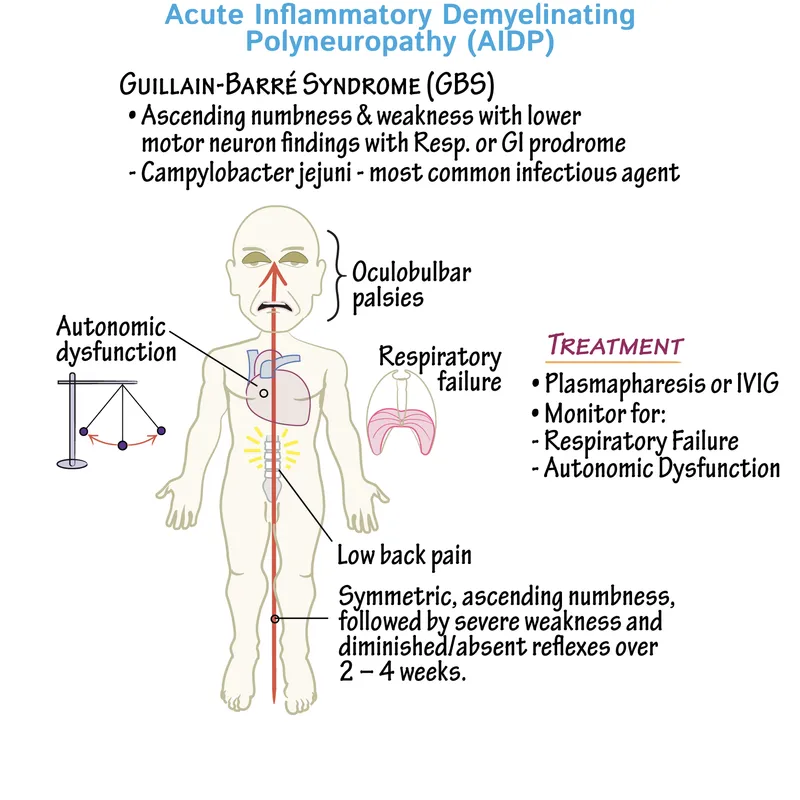
⭐ Campylobacter jejuni is the most common infectious precipitant of Guillain-Barré syndrome (GBS). The mechanism involves molecular mimicry between bacterial lipooligosaccharides and peripheral nerve gangliosides (anti-GM1 antibodies).
- Guillain-Barré Syndrome: Acute, ascending, symmetric flaccid paralysis with ↓ or absent deep tendon reflexes (areflexia).
- Reactive Arthritis: Asymmetric oligoarthritis, urethritis, conjunctivitis. Strong HLA-B27 association. 📌 "Can't see, can't pee, can't climb a tree."
Diagnosis & Treatment - Lab Hunt & Drug War
- Lab Diagnosis
- Stool Culture: Gold standard, requires special conditions.
- Grows at 42°C (thermophilic).
- Microaerophilic (↑CO₂, ↓O₂).
- Media: Skirrow's agar, Campy BAP.
- Microscopy: Gram-negative, motile, S-shaped or "gull-wing" rods.
- Biochemical: Oxidase-positive.
- Stool Culture: Gold standard, requires special conditions.
- Treatment
- Mainstay: Supportive care (rehydration).
- Severe Disease: Macrolides (e.g., Azithromycin).
- ⚠️ High rates of fluoroquinolone resistance.
⭐ Campylobacter jejuni is the most common infectious antecedent to Guillain-Barré syndrome (GBS).
High‑Yield Points - ⚡ Biggest Takeaways
- Most common bacterial cause of gastroenteritis in developed countries, frequently from undercooked poultry.
- A curved, Gram-negative rod that is oxidase-positive and thrives at 42°C (thermophilic).
- Presents with fever, cramping abdominal pain, and inflammatory bloody diarrhea.
- Strongly associated with post-infectious Guillain-Barré syndrome (GBS) due to molecular mimicry.
- Can also lead to reactive arthritis as a long-term complication.
- Usually self-limited; macrolides are reserved for severe or prolonged illness.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

