Treatment Principles - Fungal Drug Fight Club
- Severity dictates the weapon: Treatment hinges on disease severity and host immune status.
- Main Event:
- Mild-to-Moderate Disease: Itraconazole (oral).
- Severe/Disseminated Disease: Amphotericin B (IV), often lipid formulation to ↓ toxicity, followed by a step-down to oral itraconazole for >1 year.
- Specialty Match:
- Fluconazole is key for Coccidioidal meningitis due to excellent CNS penetration.
⭐ CNS Coccidioidomycosis requires lifelong suppressive therapy with fluconazole to prevent relapse.
Histoplasma & Blastomyces - Midwest Mycosis Mayhem
-
Treatment by Severity:
- Mild-to-Moderate (Pulmonary): Itraconazole for 6-12 months. Many acute cases are self-limiting; treatment can shorten symptom duration.
- Severe/Progressive Disseminated/CNS:
- Induction: Liposomal Amphotericin B (IV) for 1-2 weeks.
- Consolidation: Oral Itraconazole for ≥12 months.
-
Key Considerations:
- Immunocompromised: Always treat, even if disease appears mild.
- CNS Infection: Requires longer therapy duration and careful monitoring for relapse.
-
📌 Mnemonic: Use Ampho-"terrible" for terrible, severe disease; then Itraconazole to ensure it's "gone-azole".
⭐ In severe disseminated histoplasmosis, initial therapy with Amphotericin B is critical to reduce fungal load before transitioning to long-term itraconazole for maintenance and prevention of relapse.
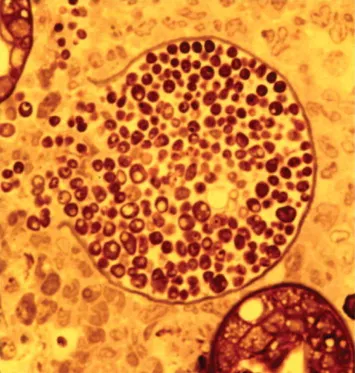
Coccidioides & Paracoccidioides - Desert & Jungle Jivers
-
Coccidioides immitis (Valley Fever)
- Asymptomatic/Mild Pulmonary: Generally no treatment; supportive care.
- Symptomatic/Progressive Lung Disease: Itraconazole or Fluconazole for 3-6 months.
- Disseminated Disease:
- Non-meningeal: Amphotericin B, followed by long-term azole (e.g., fluconazole).
- Meningitis: Lifelong high-dose fluconazole.
-
Paracoccidioides brasiliensis (South American Blastomycosis)
- Drug of Choice: Itraconazole for 6-12 months.
- Severe/Disseminated: Amphotericin B induction, then switch to itraconazole.
⭐ Coccidioidal meningitis is a severe complication requiring lifelong suppressive therapy with high-dose fluconazole to prevent relapse.
Sporothrix & Talaromyces - Gardener's & Traveler's Troubles
-
Sporothrix schenckii (Rose Gardener's Disease)
- Lymphocutaneous: Oral itraconazole for 3-6 months.
- 📌 Mnemonic: "Itra-conazole for a thorny-conundrum."
- Disseminated/Pulmonary: Lipid formulation of Amphotericin B, followed by a long course of oral itraconazole.
- Lymphocutaneous: Oral itraconazole for 3-6 months.
-
Talaromyces marneffei (formerly Penicillium marneffei)
- Primarily seen in HIV-positive individuals in Southeast Asia.
- Severe/Disseminated: Amphotericin B for 2 weeks, then itraconazole for 10 weeks.
- Mild/Step-down: Itraconazole.

⭐ In HIV patients from Southeast Asia, disseminated Talaromyces marneffei infection is considered an AIDS-defining illness, mimicking tuberculosis or histoplasmosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Itraconazole is the drug of choice for mild-to-moderate disease for most dimorphic fungi.
- Amphotericin B is used for severe, rapidly progressing, or disseminated infections.
- Treat any infection in immunocompromised patients aggressively, often starting with Amphotericin B.
- Fluconazole is preferred for coccidioidal meningitis due to its high CNS penetration.
- Lymphocutaneous sporotrichosis is uniquely treated with itraconazole.
- Coccidioidal meningitis requires lifelong fluconazole suppressive therapy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

