Innate Immunity - The Body's First Stand
- Physical & Chemical Barriers: Intact skin and mucous membranes are the first line. Low pH, fatty acids on the skin, and cilia in the respiratory tract prevent fungal settlement.
- Key Cellular Players:
- Macrophages (especially Alveolar): Engulf inhaled spores/conidia. Recognize fungal PAMPs (e.g., β-glucan, chitin) via Pattern Recognition Receptors (PRRs) like TLRs and Dectin-1.
- Neutrophils: Rapidly recruited to sites of infection. Kill fungi via phagocytosis, degranulation (releasing antifungal peptides), and formation of Neutrophil Extracellular Traps (NETs).
- Natural Killer (NK) Cells: Provide early defense by directly killing fungal cells and secreting cytokines like IFN-γ to potentiate macrophage activity.
⭐ Exam Favorite: Histoplasma capsulatum famously survives and replicates within the phagolysosome of inactivated macrophages, using this as a "Trojan horse" to disseminate systemically.

Adaptive Immunity - T-Cell Titans Take Charge
- Cell-Mediated Immunity (CMI) is Paramount: The host's primary defense against dimorphic fungi relies on a robust T-cell response, not antibodies.
- Key Player: CD4+ Th1 cells orchestrate the entire defense.
- Mechanism: Upon recognizing fungal antigens, Th1 cells release Interferon-gamma (IFN-γ).
- Action: IFN-γ super-activates macrophages, boosting their ability to kill the intracellular yeast forms.
- Clinical Significance of Immunodeficiency:
- Conditions with ↓ T-cell function (e.g., AIDS with CD4 < 200 cells/μL, lymphoma, TNF-α inhibitors) cripple this defense.
- Leads to uncontrolled fungal replication and severe, disseminated disease.
⭐ High-Yield: Patients on TNF-α inhibitors (e.g., infliximab) are at high risk for reactivating latent histoplasmosis. TNF-α is critical for forming and maintaining the granulomas that contain the fungi.
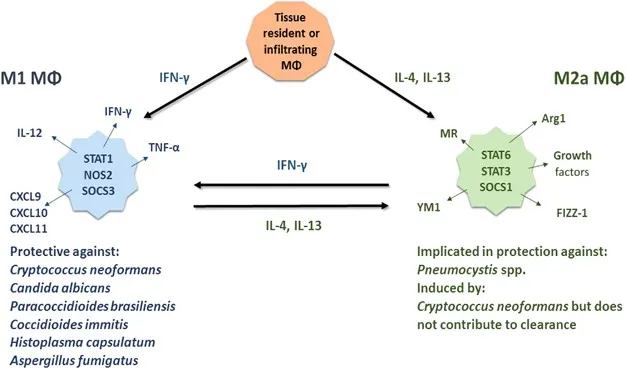
Immunodeficiency - When Defenses Crumble
-
Cell-Mediated Immunity (CMI) is Paramount: T-cell (especially CD4+ helper T-cells) and macrophage function are critical for containing dimorphic fungi in their yeast form within granulomas.
- Failure leads to: Disseminated, life-threatening disease instead of localized, asymptomatic infection.
-
Key Immunocompromised States & Associated Risks:
- HIV/AIDS: Risk of dissemination ↑ significantly with CD4+ count < 150 cells/μL. Common with Histoplasma and Coccidioides.
- Pharmacologic Immunosuppression:
- TNF-α inhibitors (e.g., infliximab, etanercept): Impair granuloma formation and maintenance.
- High-dose corticosteroids & Calcineurin inhibitors: Broadly suppress T-cell activation.
- Primary Immunodeficiencies:
- Chronic Granulomatous Disease (CGD): Defective NADPH oxidase impairs phagocyte killing of fungi.

⭐ TNF-α is essential for maintaining granulomas that contain latent Histoplasma capsulatum. Starting a TNF-α inhibitor can lead to reactivation and severe, disseminated histoplasmosis, often mimicking miliary tuberculosis.
High‑Yield Points - ⚡ Biggest Takeaways
- Cell-mediated immunity, driven by Th1-lymphocytes, is the primary host defense against dimorphic fungi.
- Immunocompromised hosts, especially those with impaired T-cell function (e.g., AIDS, lymphoma), are highly susceptible to disseminated disease.
- Use of TNF-alpha inhibitors is a major risk factor for reactivation of latent infections like Histoplasmosis.
- The thermal dimorphism (mold-to-yeast transition) is a key virulence factor that helps evade host defenses.
- Most infections in immunocompetent individuals are asymptomatic or self-limiting, conferring future immunity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

