Biofilm Basics - Slime City Genesis
- Biofilm: A structured community of microorganisms encased in a self-produced Extracellular Polymeric Substance (EPS) matrix, primarily composed of polysaccharides, proteins, and eDNA. This "slime layer" facilitates adherence to surfaces (e.g., heart valves, catheters), creating a sessile colony.
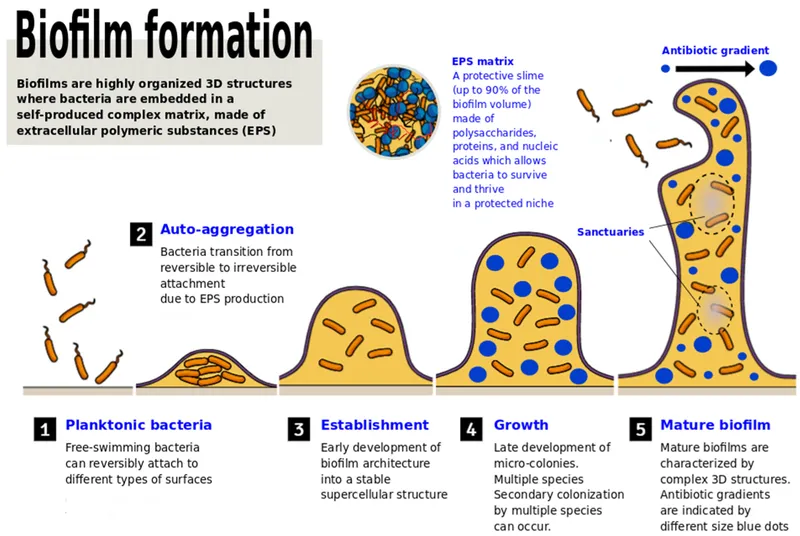
⭐ Biofilms exhibit extreme resistance to antibiotics (up to 1000x more) and host immune responses. The dense EPS matrix acts as a physical barrier, preventing antibiotic penetration and shielding microbes from phagocytosis.
Pathogenesis - Heart Valve Hijack
- Initiation: Endothelial injury on a heart valve leads to a sterile thrombus of platelets and fibrin (Non-Bacterial Thrombotic Endocarditis - NBTE).
- Adhesion: During bacteremia, bacteria adhere to the NBTE via adhesins (e.g., FimA, EbpA).
- Maturation: Bacteria proliferate and form a biofilm matrix, creating a vegetation. This shield protects from host immunity and antibiotics.
- Complications:
- Vegetation growth → valvular damage, heart failure.
- Detachment → septic emboli → infarction/abscess in brain, spleen, kidneys.
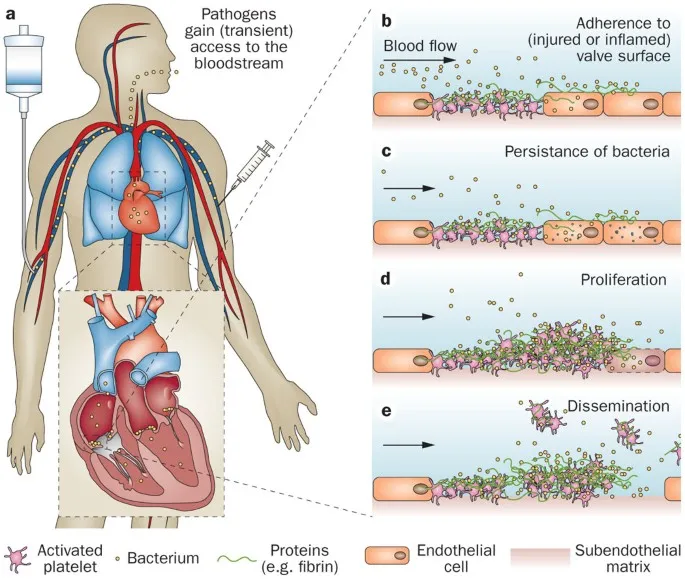
⭐ Streptococcus viridans produces dextran, a key biofilm component that facilitates strong adherence to the fibrin-platelet aggregates on damaged heart valves.
Etiology & Presentation - The Usual Suspects
- Key Pathogens & Associations:
| Pathogen | Clinical Context |
|---|---|
| Staphylococcus aureus | Acute IE, most common cause. High virulence. Often affects normal valves, common in IV drug use (tricuspid). |
| Viridans streptococci | Subacute IE. Lower virulence. Colonizes oropharynx; associated with dental procedures and damaged native valves. |
| Staphylococcus epidermidis | Prosthetic valve endocarditis (PVE), especially within 1 year of surgery. |
| Enterococci | Nosocomial infections, common after GU/GI procedures in older men. |
| HACEK Group | Slow-growing, gram-negative organisms; can lead to large vegetations. |
- **F**ever (most common symptom)
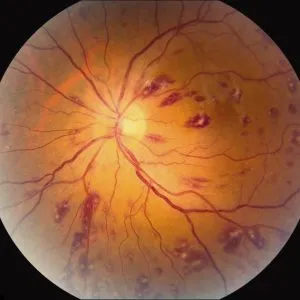
- **R**oth spots
- **O**sler nodes (painful)
- **M**urmur (new or changing)
- **J**aneway lesions (painless)
- **A**nemia
- **N**ail-bed (splinter) hemorrhages
- **E**mboli
⭐ In IV drug users, endocarditis most commonly affects the tricuspid valve, often presenting with septic pulmonary emboli rather than systemic signs.
Diagnosis & Treatment - Detect & Destroy
- Diagnosis:
- Blood Cultures: ≥3 sets from different sites.
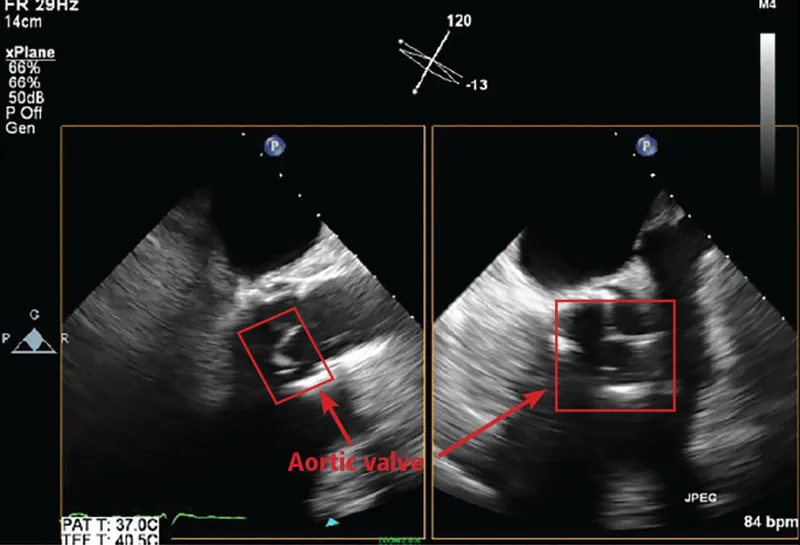
- Echocardiography: TTE first, then TEE for higher sensitivity.
- Duke Criteria: Integrates clinical, microbiological, & imaging findings.
- Treatment:
- Challenge: Biofilm's EPS matrix impairs antibiotic penetration.
- Meds: Prolonged, high-dose bactericidal agents (e.g., Penicillin + Gentamicin).
- Surgery Indicated for: Valve destruction, persistent bacteremia, large vegetations (>10 mm), recurrent emboli.
⭐ Culture-Negative Endocarditis: Suspect fastidious organisms (e.g., HACEK, Coxiella, Bartonella). Requires special culture techniques or serology.
High‑Yield Points - ⚡ Biggest Takeaways
- Biofilms are bacterial communities encased in a self-produced polysaccharide matrix, shielding them from host immunity and antibiotics.
- They are crucial in endocarditis, forming on damaged native valves or prosthetic heart valves.
- Key pathogens include S. aureus, S. epidermidis (especially on prosthetics), and Viridans streptococci.
- The biofilm matrix is a major reason for antibiotic treatment failure and persistent infection.
- Leads to large, friable vegetations that can embolize, causing strokes or systemic infarcts.
- Effective treatment often requires prolonged, high-dose antibiotics and frequently surgical valve replacement.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

