Biofilms & CF - The Slimy Setup
- Foundation: Defective CFTR protein → thick, dehydrated airway mucus. This static mucus layer is a perfect breeding ground for bacteria, especially Pseudomonas aeruginosa.
- Mechanism: Bacteria colonize the mucus, communicate via quorum sensing, and form a protective extracellular polysaccharide matrix (EPS).
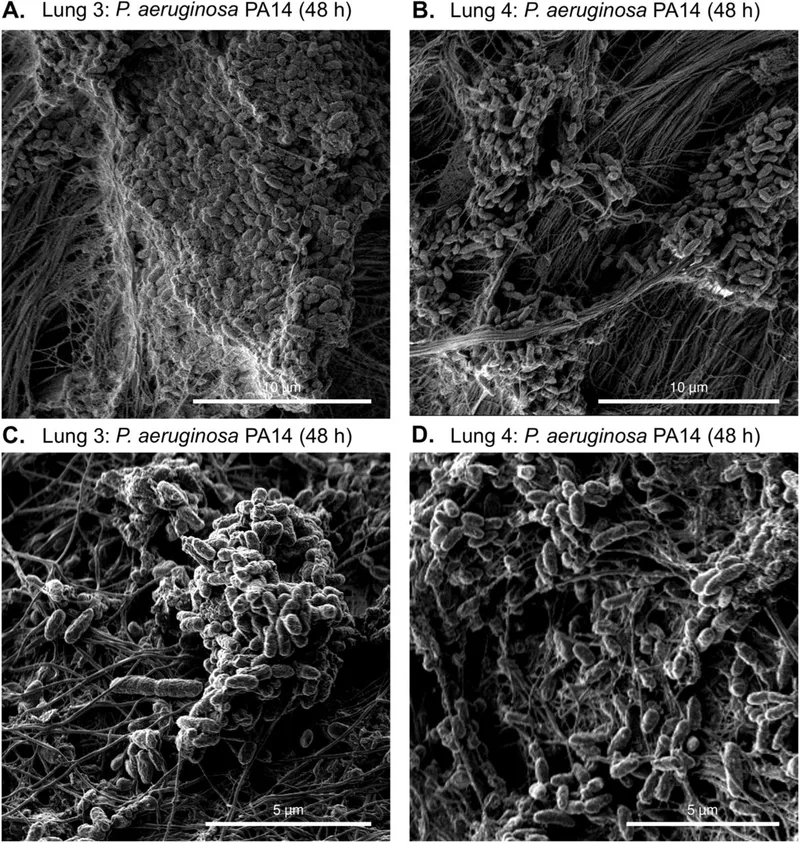
- Consequences:
- ↑ Antibiotic resistance (physical barrier).
- Chronic, difficult-to-eradicate infections.
- Persistent inflammation & progressive lung damage.
⭐ High-Yield: The mucoid phenotype of P. aeruginosa in CF is due to alginate overproduction, a key component of the biofilm matrix that shields the bacteria from host defenses and antibiotics.
Key Pathogens - The Usual Suspects
-
Pseudomonas aeruginosa: The classic CF pathogen, notorious for forming biofilms.
- Transitions from non-mucoid to a mucoid phenotype by overproducing alginate, a key biofilm component.
- This conversion marks the shift to chronic, persistent infection.
-
Staphylococcus aureus: A common early colonizer, often preceding Pseudomonas.
- Methicillin-resistant S. aureus (MRSA) is a growing concern.
-
Burkholderia cepacia complex: Less common but associated with severe necrotizing pneumonia ("cepacia syndrome") and poor outcomes.
-
Other significant pathogens:
- Haemophilus influenzae (non-typeable)
- Aspergillus fumigatus (fungal)
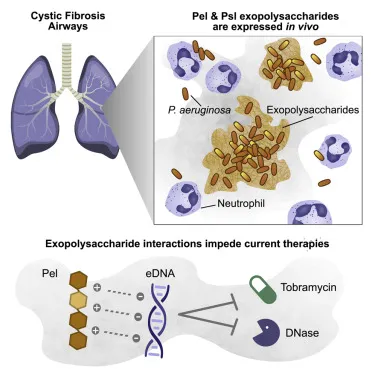
⭐ The mucoid, alginate-producing phenotype of P. aeruginosa is a major virulence factor, conferring significant resistance to both antibiotics and host immune clearance.
Pathogenesis - The Vicious Cycle
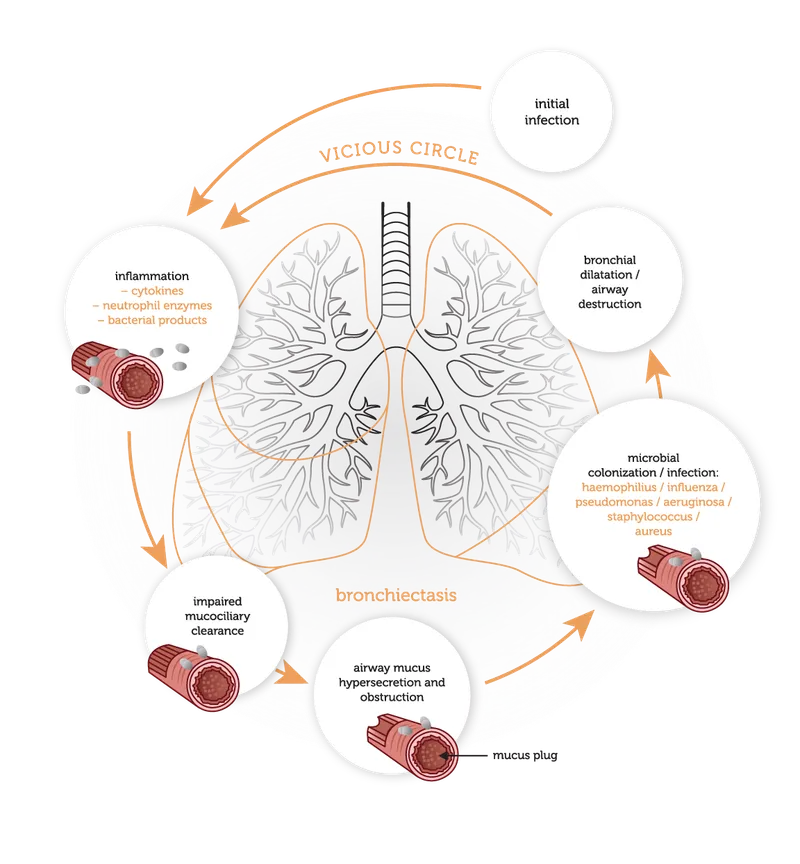
- A cycle of infection, inflammation, and tissue damage perpetuates lung disease in CF.
- Initial colonization (often P. aeruginosa) → Biofilm formation → Chronic inflammation.
- Host response is dominated by a massive, ineffective influx of neutrophils.
- Neutrophils undergo necrosis/NETosis, releasing DNA, proteases (elastase), and oxidants that damage airways and contribute to the biofilm matrix.
⭐ The DNA released from necrotic neutrophils is a key structural component of the biofilm matrix. Dornase alfa (DNase) therapy targets this extracellular DNA, cleaving it to reduce sputum viscosity.
Management - The Uphill Battle
- Aggressive Antibiotic Therapy:
- Primary strategy involves high-dose, prolonged, and often cyclical courses targeting P. aeruginosa.
- Inhaled antibiotics (e.g., tobramycin, aztreonam) are crucial for delivering high concentrations directly to the lung with minimal systemic toxicity.
- Combination therapy is standard during exacerbations.
- Biofilm & Mucus Disruption:
- Dornase alfa (DNase): An enzyme that cleaves extracellular DNA in the biofilm matrix, reducing sputum viscosity.
- Hypertonic saline: Improves airway surface hydration and facilitates mucociliary clearance.
⭐ Azithromycin is used chronically not for its bactericidal effect, but for its anti-inflammatory properties and its ability to inhibit bacterial quorum sensing, a key process in biofilm maintenance.
High‑Yield Points - ⚡ Biggest Takeaways
- Cystic Fibrosis (CF), from CFTR gene mutations, features thick mucus that fosters biofilm growth.
- Pseudomonas aeruginosa is the hallmark pathogen, switching to a mucoid phenotype by overproducing alginate.
- The biofilm matrix provides a shield, leading to high antibiotic resistance and immune evasion.
- Quorum sensing orchestrates gene expression, controlling virulence factors within the biofilm.
- Chronic biofilm presence drives persistent inflammation, bronchiectasis, and progressive lung function decline.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

