Stroke Unit Care - The Stroke Squad Hub
- Multidisciplinary Team: Coordinated care from neurologists, nurses, physio/occupational/speech therapists.
- Core Principles (📌 SQUAD):
- Swallowing screen (early) to prevent aspiration.
- Quick & early mobilization to reduce complications.
- Unified protocols for vitals & neuro checks.
- Assessment for DVT/PE risk.
- DVT prophylaxis (mechanical ± pharmacological).
- Continuous Monitoring: Cardiac rhythm, BP, O₂ saturation.
⭐ Stroke unit care is one of the few interventions proven to reduce mortality, long-term disability, and the need for institutionalization, regardless of patient age, sex, or stroke severity.
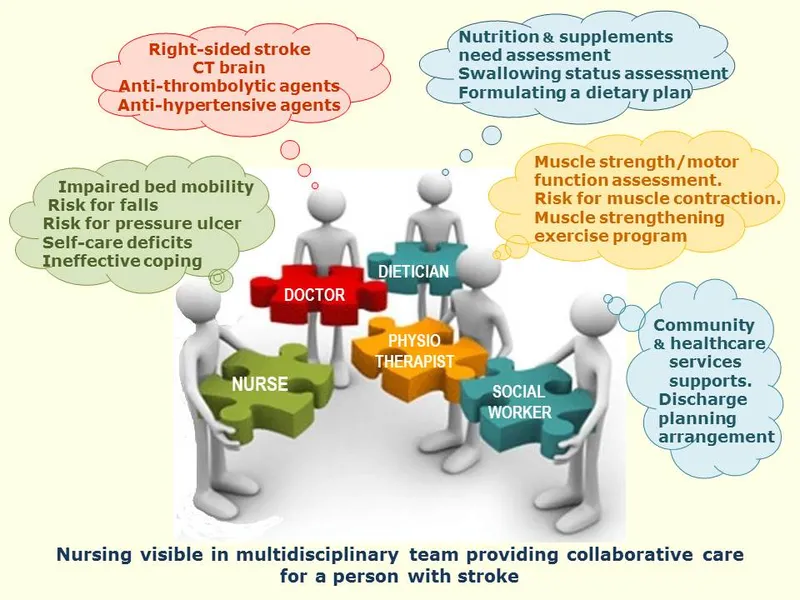
Multidisciplinary Team - Avengers Assemble!
Coordinated care in a specialized stroke unit is crucial for recovery. The team collaborates on a patient-centered plan to maximize functional outcomes and prevent recurrence.
- Core Members: Neurologists, specialized nurses, physiatrists.
- Rehabilitation: Physical & Occupational Therapists (PT/OT), Speech-Language Pathologists (SLP).
- Support: Social workers, case managers, dietitians.
⭐ Coordinated stroke unit care is the most critical intervention, proven to reduce mortality and long-term disability by up to 20% compared to general medical ward care.
Key Protocols - The Stroke Playbook
- Hemodynamic: Maintain BP <180/105 mmHg post-tPA; otherwise, permissive hypertension (goal <220/120 mmHg) is acceptable.
- Metabolic: Target glucose 140-180 mg/dL. Treat fever aggressively to maintain normothermia.
- VTE Prophylaxis: Start intermittent pneumatic compression (IPC) on admission. Delay pharmacologic prophylaxis for 24h post-tPA.
- Aspiration Risk: Patient remains NPO until a formal swallow screen is passed.
- Rehabilitation: Mobilize within 24-48 hours; consult PT, OT, and speech therapy early.
⭐ Coordinated stroke unit care is the single most effective intervention for reducing post-stroke mortality and long-term disability, benefiting a broader patient population than thrombolysis.
Complication Management - Dodging Dangers
- VTE Prophylaxis:
- Immediate intermittent pneumatic compression (IPC).
- Start LMWH/heparin after 24-48h if stable; hold for 24h post-tPA.
- Aspiration & Pneumonia:
- Strict NPO until passing a bedside swallow screen.
- Keep head of bed elevated >30°.
- Cerebral Edema (Malignant Infarct):
- Peaks at 3-5 days.
- Treat with hyperosmolar therapy (mannitol, hypertonic saline).
- Consider decompressive hemicraniectomy.
- Other Complications:
- Seizures: Treat if they occur; no prophylaxis.
- UTI: Avoid indwelling catheters.
⭐ Post-stroke depression is common (~33%) and impairs recovery. Routinely screen and treat with SSRIs (Sertraline, Escitalopram).
Rehabilitation & Discharge - The Road to Recovery
- Early start: Initiate rehab within 24-48 hours if medically stable to maximize recovery.
- Core team: Coordinated effort by Physical Therapy (PT), Occupational Therapy (OT), and Speech-Language Pathology (SLP).
- Primary goals: Improve mobility, restore Activities of Daily Living (ADLs), and prevent complications (e.g., DVT, contractures).
- Discharge planning: Begins on admission, evaluating home safety and social support.
⭐ The most significant motor and functional gains are typically seen within the first 3-6 months post-stroke.
High-Yield Points - ⚡ Biggest Takeaways
- Stroke unit care is superior to general ward care, utilizing a multidisciplinary team (physicians, nurses, PT, OT, speech therapy).
- Early mobilization and DVT prophylaxis are critical to prevent venous thromboembolism and other complications of immobility.
- Perform a swallowing assessment before initiating oral intake to reduce aspiration pneumonia risk.
- Maintain permissive hypertension in acute ischemic stroke (if no thrombolysis) to ensure cerebral perfusion.
- Aggressively treat fever and hyperglycemia, as both are associated with worse neurological outcomes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

