Stroke Recognition - FAST & Furious Onset
- Sudden onset of a focal neurologic deficit. Ascertaining "last known normal" time is critical.
- 📌 Use the FAST mnemonic for rapid prehospital and ED screening:
- Face: Unilateral drooping (ask patient to smile).
- Arm: Unilateral weakness or drift (ask to hold arms out).
- Speech: Slurred (dysarthria) or abnormal language (aphasia).
- Time: Time is brain! Immediate transport.
⭐ Stroke mimics are frequent. Hypoglycemia can perfectly replicate focal stroke signs; always perform a fingerstick glucose test immediately on arrival.
ED Arrival & Triage - Door to Needle Dash
Immediate goal: Rapidly assess for thrombolysis eligibility. The clock starts from symptom onset or the patient's last known well time.
- Door to Physician (<10 min)
- Assess ABCs, vitals, establish IV access.
- Perform NIH Stroke Scale (NIHSS).
- Check finger-stick glucose to rule out hypoglycemia.
- Door to Stroke Team (<15 min)
- Activate stroke team for parallel processing.
- Door to CT Scan (<25 min)
- Immediate non-contrast head CT is crucial.
- Door to Needle (<60 min)
⭐ The single most important initial test is a non-contrast head CT. It is essential to differentiate between ischemic and hemorrhagic stroke, as this fundamentally dictates all subsequent management decisions.
Clinical Evaluation - Scoring the Deficit
- NIH Stroke Scale (NIHSS): Standardized tool to quantify stroke-related neurological deficits.
- Assesses 11 items including consciousness, language, motor strength, and sensation.
- Score ranges from 0 (no deficit) to 42 (most severe).
- Guides treatment decisions (e.g., tPA, thrombectomy).
- Severity:
- <5: Mild
- 5-14: Moderate
- 15-24: Severe
- >24: Very Severe
⭐ An NIHSS score >22 is strongly associated with a high likelihood of death or severe disability and may predict malignant cerebral edema and hemorrhagic transformation.
- Modified Rankin Scale (mRS): Measures degree of disability in daily activities post-stroke, from 0 (no symptoms) to 6 (dead). Assesses long-term outcome.
Initial Imaging - Code Gray Matter
-
Primary Goal: Immediate non-contrast CT (NCCT) to rapidly exclude intracranial hemorrhage (ICH) before thrombolysis. Ischemic changes may not be visible in the first few hours.
-
Key NCCT Findings:
- Hemorrhage: Appears hyperdense (bright).
- Early Ischemia: Subtle signs like loss of grey-white differentiation, the insular ribbon sign, or a hyperdense MCA sign.
-
Advanced Imaging:
- CTA (Angiography): Identifies large vessel occlusion (LVO).
- CTP (Perfusion): Differentiates infarct core from the penumbra (salvageable tissue).
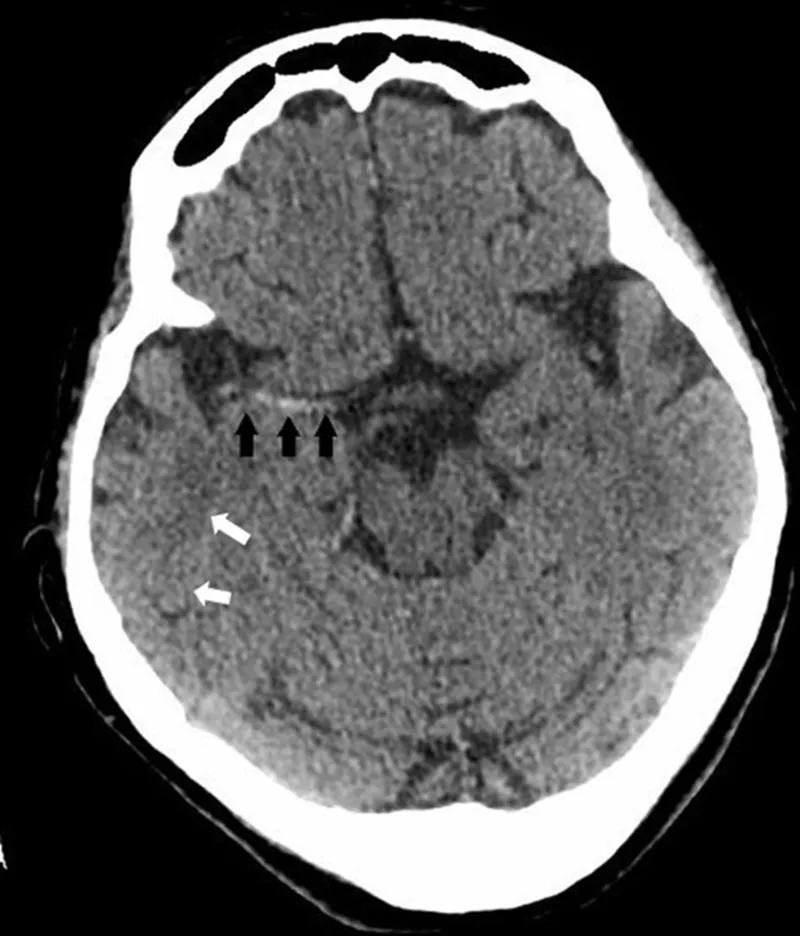
⭐ The ASPECTS score on NCCT quantifies early ischemic changes in the MCA territory. A score < 6 suggests a large, established infarct and may be a relative contraindication for thrombectomy.
Stroke Mimics - The Great Pretenders
- Conditions presenting with focal neurologic deficits that are not due to cerebral ischemia.
- Rapid identification is key to avoid misdiagnosis and inappropriate tPA administration.
- Common mimics include:
- Seizures (post-ictal Todd's paralysis)
- Hypoglycemia (< 50 mg/dL)
- Migraine with aura
- CNS tumor or abscess
- Conversion disorder
- Hypertensive encephalopathy
⭐ Hypoglycemia is a critical mimic. Always check a finger-stick glucose on arrival; it's rapidly reversible.
- BE-FAST (Balance, Eyes, Face, Arm, Speech, Time) is the key to rapid stroke recognition.
- Immediate non-contrast head CT is essential to distinguish ischemic vs. hemorrhagic stroke.
- Always check blood glucose to rule out hypoglycemia, a common stroke mimic.
- The NIH Stroke Scale (NIHSS) is the standard for quantifying neurological deficit.
- "Time is brain" - the therapeutic window for tPA is extremely limited, typically <4.5 hours.
- Suspect hemorrhagic stroke with a "thunderclap" headache and early vomiting.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

