Rehab Principles - Get Moving, Brain!
- Core Goal: Harness neuroplasticity-the brain's ability to rewire. Early and intensive therapy is key.
- Multidisciplinary Team: Physical Therapy (PT) for motor function, Occupational Therapy (OT) for Activities of Daily Living (ADLs), and Speech-Language Pathology (SLP) for communication/swallowing.
- Key Principles: Task-specific, repetitive, high-intensity, and goal-oriented training to prevent "learned non-use."
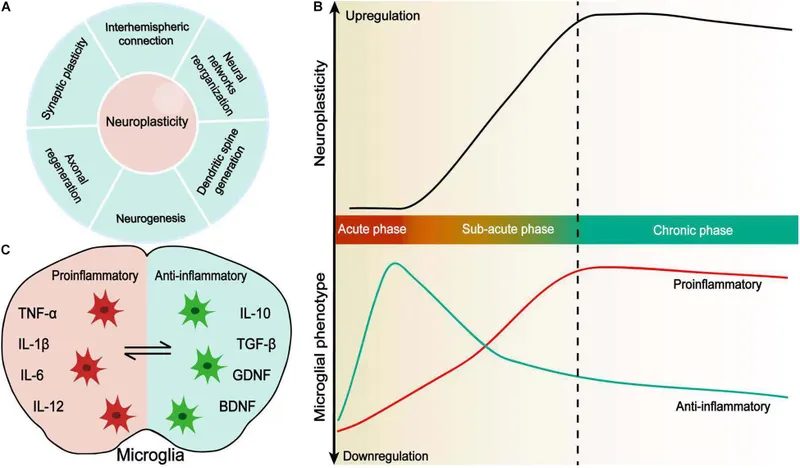
⭐ Critical Window: The most significant motor recovery typically occurs within the first 3-6 months post-stroke, emphasizing the urgency of early, intensive rehabilitation.
The Rehab Team - Meet the Crew
- Physiatrist (Rehab Physician): Team leader; creates the overall rehab plan.
- Physical Therapist (PT):
- Focus: Gross motor skills (walking, balance, transfers).
- Occupational Therapist (OT):
- Focus: Fine motor skills & Activities of Daily Living (ADLs).
- Tasks: Dressing, eating, bathing, adaptive equipment.
- 📌 Mnemonic: OT = Occupations of daily living.
- Speech-Language Pathologist (SLP):
- Manages aphasia (language) and dysphagia (swallowing).
- Social Worker/Case Manager:
- Coordinates discharge planning, insurance, and community resources.
⭐ The SLP's swallow evaluation is critical. Aspiration pneumonia from unrecognized dysphagia is a major cause of post-stroke mortality.
Deficit Management - Fixing the Glitches
-
Core Principle: Neuroplasticity
- Brain's ability to reorganize by forming new neural connections.
- Harness through repetitive, task-specific practice.
-
Motor Deficits (Hemiparesis/Hemiplegia)
- Physical Therapy (PT): Focus on gait, balance, strength, and mobility.
- Occupational Therapy (OT): Activities of Daily Living (ADLs) retraining (e.g., dressing, eating).
- Constraint-Induced Movement Therapy (CIMT): Restrain unaffected limb to force use of the affected limb.
-
Speech & Language (Aphasia)
- Speech-Language Pathologist (SLP) consult is key.
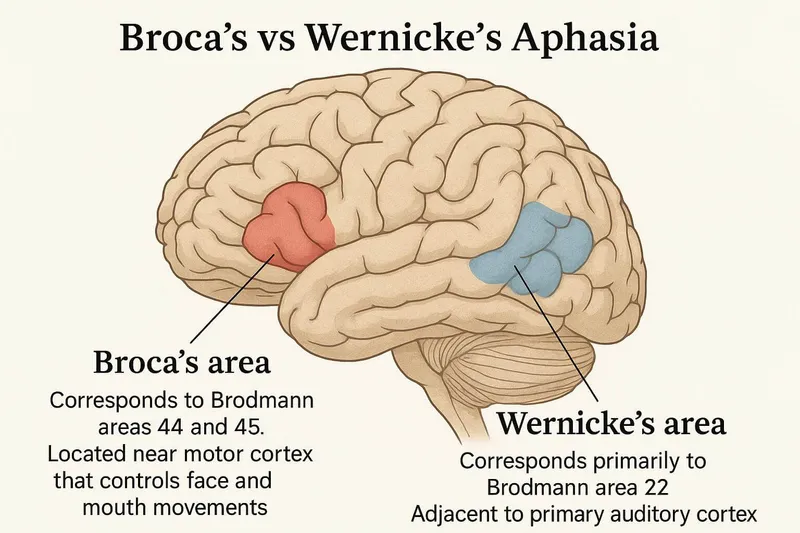
- 📌 BEAM Mnemonic: Broca's Expressive Aphasia (Broken speech), Motor; Wernicke's Receptive Aphasia (Word salad), Sensory.
-
Cognitive & Perceptual
- Neglect Syndrome: (Usually right parietal lobe) Patient ignores one side of space. Address with visual scanning exercises.
- Apraxia: Inability to perform learned movements on command.
⭐ High-Yield Fact: Post-stroke depression is common (~33% of survivors) and can significantly impede rehabilitation progress. Screen and treat aggressively.
Complication Prevention - Dodging Dangers
- VTE Prophylaxis:
- Early mobilization is crucial.
- Pharmacologic prevention (LMWH/heparin) for non-ambulatory patients.
- Aspiration Pneumonia:
- Perform a bedside swallow screen before any oral intake.
- Consult speech therapy for diet modification.
- Pressure Ulcers:
- Reposition patient every 2 hours.
- Utilize pressure-reducing mattresses.
- Contractures:
- Initiate passive and active range-of-motion exercises.
- Apply splints in functional positions.
⭐ In immobile stroke patients, deep vein thrombosis (DVT) prophylaxis is a priority and should be started immediately unless active hemorrhage is present.
High-Yield Points - ⚡ Biggest Takeaways
- Early and intensive mobilization is crucial to prevent complications and improve functional outcomes.
- Task-specific training, like Constraint-Induced Movement Therapy (CIMT), promotes neuroplasticity.
- Manage spasticity with physical modalities, botulinum toxin, or baclofen to improve motor function.
- Speech and language therapy is essential for aphasia; address both expressive and receptive deficits.
- For hemispatial neglect, encourage visual scanning exercises and environmental modifications.
- Screen for and treat post-stroke depression as it significantly impacts recovery.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

