Initial Resuscitation - The Golden Hour
- Recognition: Use SOFA or qSOFA (quick SOFA) for early identification. Suspect sepsis with organ dysfunction signs.
- Key Markers: Measure lactate level; remeasure if initial lactate is > 2 mmol/L.
⭐ The Surviving Sepsis Campaign 'Hour-1 Bundle' emphasizes the urgency of completing key resuscitation tasks within the first hour of recognition of septic shock.
- Fluid Resuscitation: Begin rapid administration of 30 mL/kg crystalloid for hypotension or lactate ≥4 mmol/L.
- Vasopressors: If hypotension persists during or after fluid resuscitation, initiate vasopressors to maintain a mean arterial pressure (MAP) of ≥65 mmHg.
Vasopressors & Inotropes - The Pressure Push
-
Primary Goal: Achieve and maintain Mean Arterial Pressure (MAP) ≥65 mmHg. Continuous monitoring via an arterial line is crucial.
-
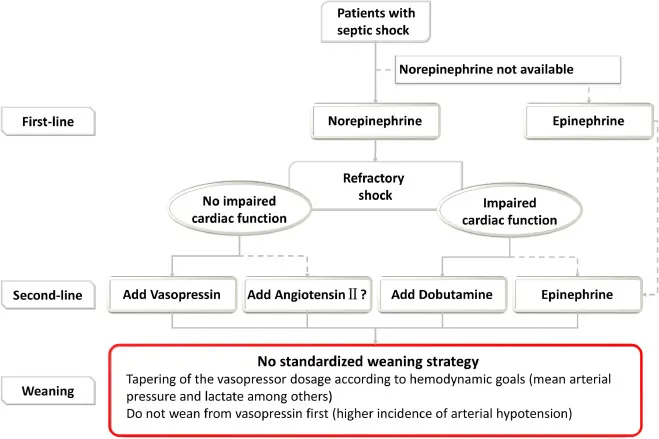
Vasopressor Sequence:
- Norepinephrine (Levophed): First-line agent. Potent vasoconstrictor (alpha-1) with modest inotropic effects (beta-1).
- Vasopressin: Adjunctive agent, added to norepinephrine to decrease its required dose. Acts on V1 receptors.
- Epinephrine: Second-line for refractory shock despite norepinephrine and vasopressin.
-
Inotrope for Cardiac Support:
- Dobutamine: Consider if signs of myocardial dysfunction (e.g., low cardiac output) or persistent hypoperfusion exist despite achieving MAP goal.
⭐ Norepinephrine is the first-choice vasopressor for septic shock due to its potent alpha-adrenergic effects (vasoconstriction) with less risk of tachyarrhythmias compared to dopamine.
Source Control & Antibiotics - Find It, Fight It
- Goal: Eradicate the infection source while providing immediate antimicrobial coverage.
- 📌 Mnemonic: C-A-S-D
- Cultures: Obtain blood cultures (x2) + other relevant sites (e.g., urine, sputum) before antibiotics. Crucially, do not delay antibiotic administration.
- Antibiotics: Start empiric broad-spectrum IV antibiotics ASAP.
- Source Control: Aggressively identify and manage the infection origin (e.g., drain abscess, remove infected lines/devices, debride tissue).
- De-escalate: Narrow antibiotic coverage once sensitivities are known.
⭐ Empiric antimicrobial therapy should be initiated as soon as possible, ideally within one hour of septic shock recognition, as delays are associated with increased mortality.
Adjunctive Therapies - Supporting Cast
- IV Corticosteroids:
- Use IV hydrocortisone for refractory septic shock (hypotension unresponsive to fluids/vasopressors).
⭐ Intravenous corticosteroids are recommended only for adult patients with septic shock and refractory hypotension (persistently low blood pressure despite adequate fluid and vasopressor therapy).
- Glycemic Control:
- Target blood glucose <180 mg/dL with an insulin infusion; prevent hypoglycemia.
- Prophylaxis:
- DVT: Low-molecular-weight heparin (LMWH) or unfractionated heparin.
- Stress Ulcer: Proton pump inhibitors (PPIs) or H2 blockers if risk factors for GI bleed are present.
- Ventilatory Support:
- For ARDS, use low tidal volume ventilation to prevent further lung injury.
- Bicarbonate Therapy:
- Controversial; consider if severe acidemia ($pH$ <7.15) persists.
High‑Yield Points - ⚡ Biggest Takeaways
- Septic shock = Sepsis + persistent hypotension requiring vasopressors to maintain MAP ≥ 65 mmHg AND serum lactate > 2 mmol/L despite adequate volume resuscitation.
- Initial management: 30 mL/kg IV crystalloid bolus within the first 3 hours.
- First-line vasopressor is norepinephrine for persistent hypotension.
- Administer broad-spectrum antibiotics within 1 hour of recognition, after obtaining blood cultures.
- Consider IV hydrocortisone for refractory shock unresponsive to fluids and vasopressors.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

