Initial Resuscitation - The First Hour Flood
- Goal: Rapidly restore tissue perfusion & reverse hypotension (MAP < 65 mmHg). Time is tissue!
- Fluid of Choice: Isotonic crystalloids (Lactated Ringer's > Normal Saline).
- Initial Bolus: Administer 30 mL/kg of actual body weight as an IV bolus. Aim to complete within the first 1-3 hours.
⭐ Lactated Ringer's is often favored over Normal Saline to prevent non-anion gap hyperchloremic metabolic acidosis, especially with large volume resuscitation.
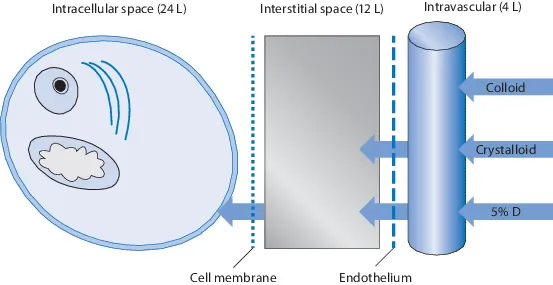
Fluid Choice - Crystal Clear Choices
- Crystalloids: First-line therapy for sepsis and septic shock.
- Balanced crystalloids (Lactated Ringer's, Plasma-Lyte) are preferred over normal saline.
- Normal Saline (0.9% NaCl): Associated with ↑ risk of hyperchloremic metabolic acidosis and acute kidney injury (AKI).
- Albumin (Colloid): Not a first-line agent.
- Consider if substantial amounts of crystalloids have been administered and hemodynamic goals are not met.
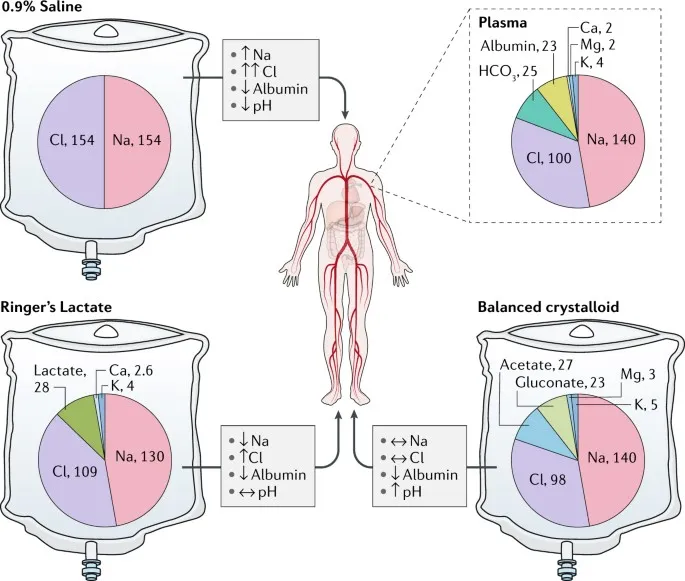
⭐ The SMART trial demonstrated that using balanced crystalloids over saline led to a lower incidence of major adverse kidney events within 30 days (MAKE30) in critically ill adults.
Assessing Response - Reading the River
- Dynamic > Static: Prioritize dynamic measures to predict fluid responsiveness.
- Passive Leg Raise (PLR): Autotransfusion of ~300mL blood.
- Pulse Pressure/Stroke Volume Variation (PPV/SVV): For intubated patients.
- Key Perfusion Markers:
- MAP: Target >65 mmHg.
- Urine Output: Target >0.5 mL/kg/hr.
- Lactate Clearance: ↓ indicates improved tissue oxygenation.
- Capillary Refill Time: Normalize.
⭐ Lactate clearance is a key prognostic marker. Failure to decrease lactate by 10-20% within the first few hours is a poor prognostic sign.
Dynamic Assessment - Will More Fluid Float?
Static measures (e.g., CVP) are poor predictors of fluid responsiveness. Dynamic methods assess if the heart is on the steep part of the Frank-Starling curve and will respond to a fluid challenge.
- Passive Leg Raise (PLR): A reversible, "internal" fluid bolus (~300mL). A positive test is a >10% increase in cardiac output or stroke volume.
- Pulse Pressure Variation (PPV) / Stroke Volume Variation (SVV): For mechanically ventilated patients (no arrhythmias, regular rhythm). Variation >12-15% suggests fluid responsiveness.
- IVC Ultrasound: Measures respiratory variation in IVC diameter.
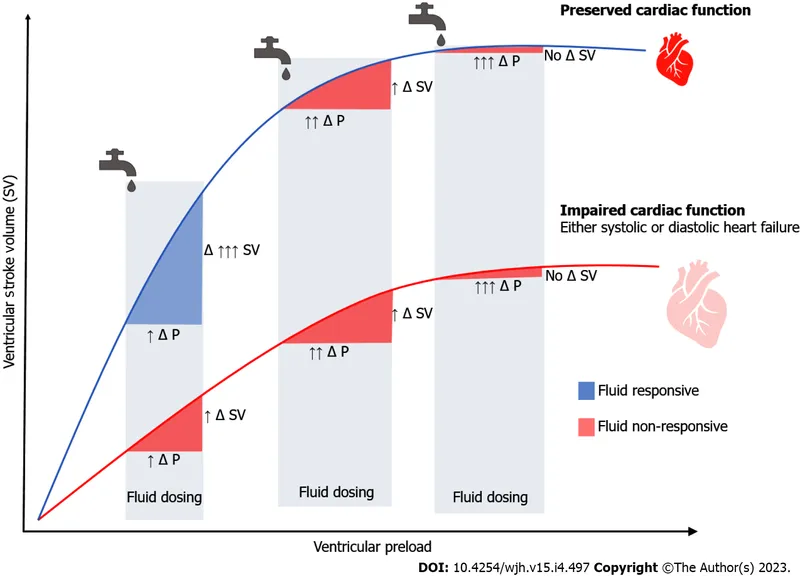
⭐ Most dynamic assessments are unreliable in patients with spontaneous respiratory efforts, arrhythmias (especially atrial fibrillation), or low tidal volume ventilation.
High‑Yield Points - ⚡ Biggest Takeaways
- Initial resuscitation begins with a rapid 30 mL/kg bolus of isotonic crystalloids (Normal Saline or Lactated Ringer's).
- Reassess fluid responsiveness using dynamic measures like passive leg raise, not just static pressures like CVP.
- If hypotension persists despite fluids, initiate vasopressors; norepinephrine is the first-line agent.
- Target a Mean Arterial Pressure (MAP) of ≥65 mmHg.
- Guide therapy to normalize serum lactate, indicating improved tissue perfusion.
- Use caution in heart or renal failure to prevent iatrogenic volume overload.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

