Initial Dx - When Hearts Break
- Timeline: Acute (<24 hrs) to 2 weeks post-MI.
- Presentation: Sudden hemodynamic collapse, new murmur, shock.
- Key to Dx: Urgent bedside echocardiogram is crucial.

⭐ A palpable thrill with a new harsh holosystolic murmur at the left lower sternal border strongly suggests a ventricular septal defect. This is often accompanied by a "step-up" in oxygen saturation from the right atrium to the right ventricle.
VSD - The Septal Breach
- Timeline: Acute, catastrophic event 3-5 days post-MI.
- Exam: New, loud, harsh holosystolic murmur at the left lower sternal border (LLSB), often with a palpable thrill.
- Pathophysiology: Rupture of the interventricular septum creates a left-to-right shunt, leading to acute RV overload and cardiogenic shock.
⭐ Key Diagnostic Finding: A significant O₂ saturation “step-up” from the right atrium to the right ventricle confirms the diagnosis during catheterization.
Acute MR - Snapped Cords
- Timeline: Acute onset 2-7 days post-MI.
- Pathophysiology: Ischemic rupture of a papillary muscle, causing torrential mitral regurgitation.
- 📌 PPM: Posteromedial muscle, supplied only by the PDA, is more Prone to rupture.
- Clinical Findings:
- Sudden hemodynamic collapse with severe pulmonary edema.
- New, soft (or loud) holosystolic murmur at the apex.
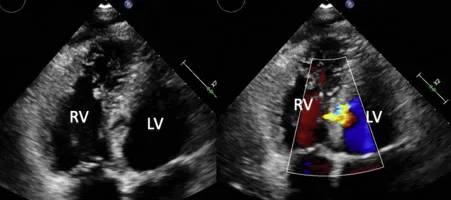
- Diagnosis: Echo shows a flail, mobile leaflet.
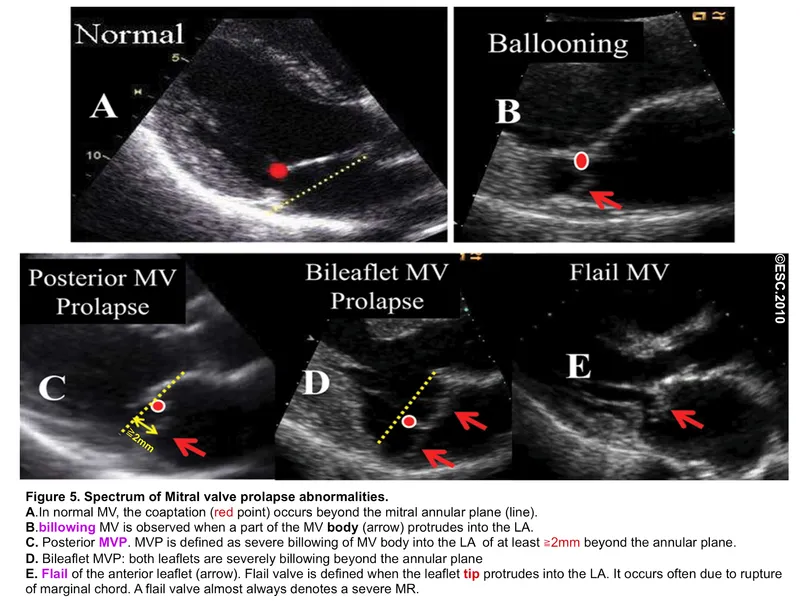
⭐ Unlike chronic MR, the left atrium is normal-sized and non-compliant, leading to a dramatic backup of pressure into the pulmonary circulation.
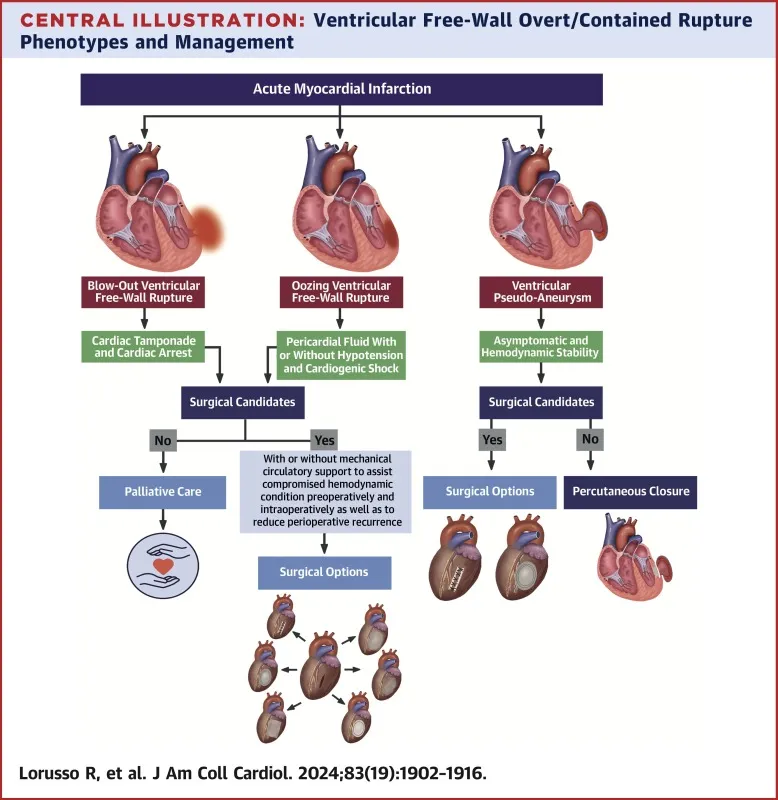
Free Wall Rupture - The Final Blowout
- Timeline: Occurs 5 days to 2 weeks post-MI, when macrophage-mediated collagen degradation weakens the necrotic myocardium.
- Pathophysiology: A full-thickness tear leads to acute hemopericardium and cardiac tamponade.
- Presentation: Sudden onset of chest pain, cardiogenic shock, and often pulseless electrical activity (PEA), leading to rapid deterioration and death.
- Classic signs include Beck's triad (hypotension, JVD, muffled heart sounds).
⭐ A pseudoaneurysm is a contained free wall rupture, where the pericardium adheres to the myocardium, preventing a full blowout.
Aneurysms - True vs. False Pouch
- Occur weeks to months post-MI. Presents with heart failure, arrhythmias, or mural thrombus.
| Feature | True Aneurysm | Pseudoaneurysm (False) |
|---|---|---|
| Wall | All 3 layers (infarcted) | Contained rupture (pericardium) |
| Neck | Wide | Narrow |
| Rupture Risk | Low | High (surgical emergency) |
| ECG | Persistent ST elevation | Non-specific changes |
⭐ Persistent ST elevation several weeks post-MI suggests a ventricular aneurysm. It's a classic exam clue, distinguishing it from acute ischemia.
High‑Yield Points - ⚡ Biggest Takeaways
- Ventricular septal rupture presents with a new, loud holosystolic murmur and requires urgent surgical repair.
- Papillary muscle rupture causes acute severe mitral regurgitation, also necessitating emergency surgery.
- Free wall rupture is the most fatal, leading to cardiac tamponade and PEA; requires emergent pericardiocentesis and surgery.
- Initial stabilization for septal and papillary rupture involves afterload reduction and an intra-aortic balloon pump (IABP) as a bridge to surgery.
- Echocardiography is the essential first step for diagnosing all post-MI mechanical complications.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

