Pathophysiology - The Clot Thickens
- Adhesion: Endothelial damage exposes von Willebrand Factor (vWF), which binds to platelet glycoprotein (Gp) Ib receptors.
- Activation: Platelets change shape and release pro-thrombotic factors:
- Thromboxane A₂ ($TXA_2$) from arachidonic acid via COX-1.
- Adenosine diphosphate (ADP) from dense granules.
- Aggregation: $TXA_2$ and ADP activate other platelets, leading to conformational change in GpIIb/IIIa receptors, which bind fibrinogen to cross-link platelets.
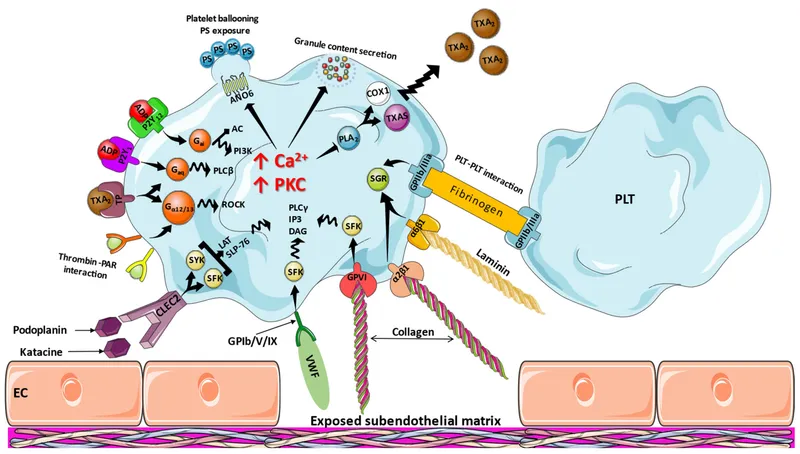
⭐ The GpIIb/IIIa receptor is the final common pathway for platelet aggregation, making it a potent target for antiplatelet therapy (e.g., abciximab, eptifibatide, tirofiban).
Antiplatelet Agents - The Platelet Punchers
-
Aspirin (ASA): Irreversibly inhibits COX-1, preventing Thromboxane A₂ ($TXA_2$) synthesis. The effect lasts for the platelet's lifespan (7-10 days).
-
P2Y₁₂ Receptor Blockers: Prevent ADP-mediated platelet activation and aggregation.
- Irreversible: Clopidogrel, Prasugrel.
- Reversible: Ticagrelor, Cangrelor.
⭐ Clopidogrel is a prodrug activated by hepatic CYP2C19. Genetic polymorphisms can cause variable efficacy and treatment failure.
-
Glycoprotein (GP) IIb/IIIa Inhibitors: Directly block the final common pathway of aggregation.
- Abciximab, Eptifibatide, Tirofiban.
- Primarily used in high-risk patients during percutaneous coronary intervention (PCI).
-
Phosphodiesterase (PDE) Inhibitors: Increase cAMP, which inhibits platelet function.
- Dipyridamole, Cilostazol.
- Cilostazol also acts as a direct arterial vasodilator, used for intermittent claudication.

Treatment Algorithm - DAPT Decision Dash
- Core Principle: Balance ischemic risk vs. bleeding risk.
- Default Duration (Post-ACS or Elective PCI): Aspirin + P2Y12 inhibitor for 6-12 months.
⭐ The DAPT Score predicts risk/benefit of continuing therapy. A score ≥2 favors extending DAPT, while a score <2 favors stopping after the initial period due to bleeding risk outweighing ischemic benefit.
Complications & Caveats - Bleeding & Beyond
- Bleeding: Most common complication. Risk ↑ with age, CKD, low body weight, and invasive procedures.
- Sites: GI (most frequent), intracranial (most feared), access site.
- Management: Varies by severity; may involve holding therapy, transfusion, or reversal agents (rarely).
- Other Adverse Effects:
- Ticagrelor: Dyspnea (common, usually transient), ↑uric acid, ventricular pauses.
- Clopidogrel/Prasugrel: ⚠️ Thrombotic Thrombocytopenic Purpura (TTP).
⭐ TTP is a rare but life-threatening complication associated with thienopyridines, especially clopidogrel, typically occurring within the first 2 weeks of therapy.
High-Yield Points - ⚡ Biggest Takeaways
- Dual antiplatelet therapy (DAPT) with Aspirin and a P2Y12 inhibitor is the cornerstone of ACS management.
- Administer Aspirin immediately; it irreversibly inhibits COX-1, blocking thromboxane A2 production.
- P2Y12 inhibitors like Clopidogrel, Prasugrel, and Ticagrelor prevent ADP-mediated platelet aggregation.
- Prasugrel is contraindicated in patients with a history of stroke or TIA.
- Ticagrelor is reversible and a common side effect is dyspnea.
- Continue DAPT for at least 12 months post-ACS, particularly after stenting.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

