Nephritic Essentials - Inflamed & Leaky Filters
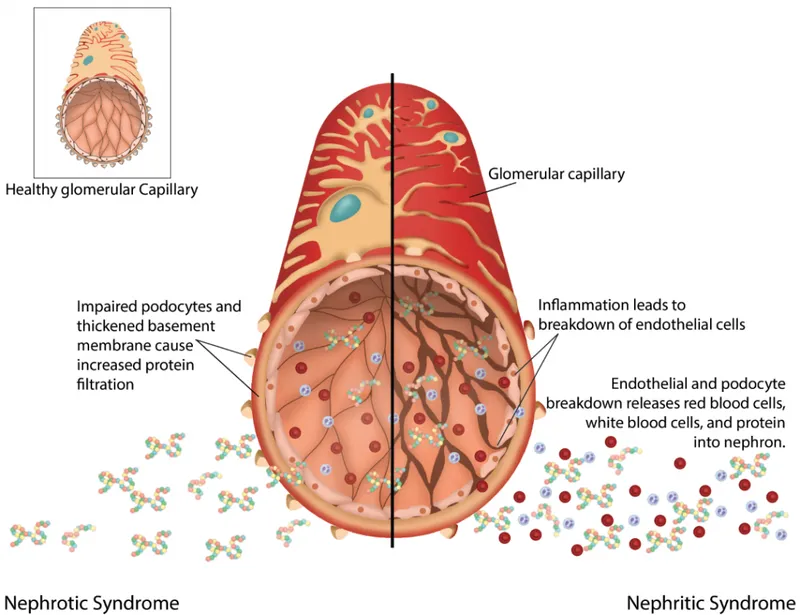
- Pathophysiology: Glomerular inflammation (proliferative changes) damages the capillary wall, creating pores that allow RBCs and some protein to leak into the urine.
- Clinical Hallmarks:
- Hypertension (salt/water retention)
- Oliguria (↓ GFR)
- Hematuria (cola-colored urine)
- Edema (periorbital)
- Urinalysis: The key diagnostic finding is RBC casts. Also shows dysmorphic RBCs and hematuria. Proteinuria is present but sub-nephrotic (< 3.5 g/day).
⭐ Post-streptococcal glomerulonephritis (PSGN) is the classic example, typically developing 1-3 weeks after a streptococcal pharyngitis or impetigo. Look for low C3 levels.
Etiology - A Cast of Characters
-
Post-Infectious Glomerulonephritis (PIGN)
- Most common: Post-streptococcal (PSGN), typically 1-3 weeks after pharyngitis or impetigo.
- Others: Endocarditis, shunt nephritis, abscesses.
-
IgA Nephropathy (Berger's Disease)
- Most common primary glomerulonephritis worldwide.
- Often follows URI/GI infection (synpharyngitic).
-
Rapidly Progressive Glomerulonephritis (RPGN) - Crescentic
- Type I (Anti-GBM): Goodpasture's syndrome.
- Type II (Immune Complex): Complication of PIGN, IgA, Lupus Nephritis, MPGN.
- Type III (Pauci-Immune): ANCA-associated vasculitis (GPA, MPA).
-
Hereditary Nephritis
- Alport Syndrome: Defect in Type IV collagen.
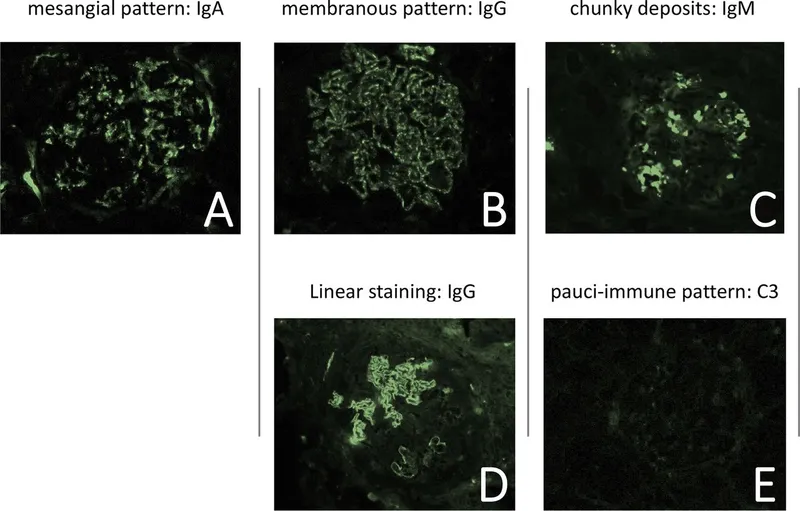
⭐ Exam Favorite: PSGN classically shows a "lumpy-bumpy" granular pattern on immunofluorescence due to subepithelial immune complex deposits.
Workup & Dx - The Clinical Detective
- Urinalysis (UA) First:
- Hematuria (>3 RBCs/hpf)
- RBC casts & dysmorphic RBCs are hallmark findings.
- Sub-nephrotic proteinuria (<3.5 g/day)
- Bloodwork:
- ↑ BUN & Creatinine (azotemia)
- ↓ Complement levels (C3, C4) suggest post-strep, lupus, or MPGN.
- Serology: ASO (post-strep), anti-dsDNA (SLE), ANCA (vasculitis).
- Kidney Biopsy: Gold standard for definitive diagnosis & guiding therapy.
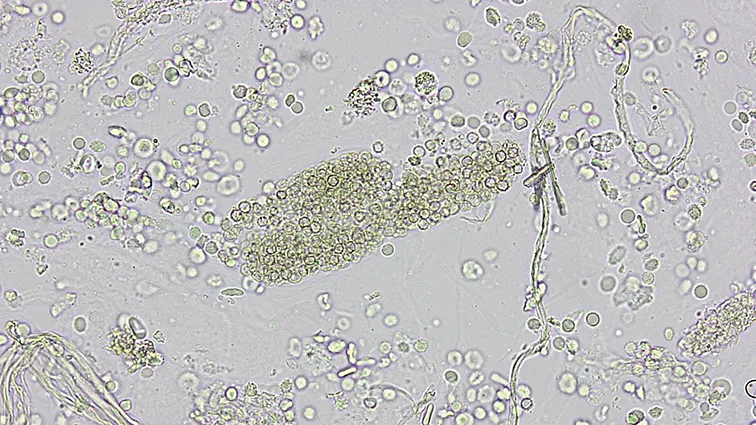
⭐ RBC casts are pathognomonic for glomerular hematuria, essentially confirming glomerulonephritis as the cause of bleeding.
Management - Damage Control
- Goal: Control hypertension, edema, and hypervolemia to prevent immediate complications (e.g., hypertensive encephalopathy, pulmonary edema).
- Core Interventions:
- Salt & Water Restriction: Foundational first step.
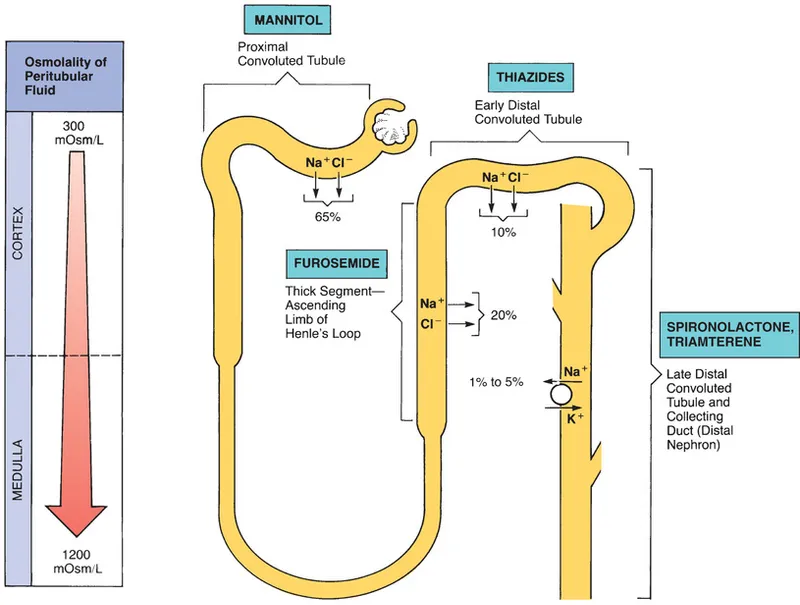
- Loop Diuretics: Furosemide is first-line for managing volume overload and hypertension.
- Vasodilators: Add if blood pressure remains uncontrolled (e.g., CCBs, hydralazine).
- Severe/Refractory Cases:
- Dialysis for unresponsive fluid overload, severe hyperkalemia, or uremic symptoms.
⭐ In rapidly progressive glomerulonephritis (RPGN), treatment is urgent: initiate high-dose pulse corticosteroids (e.g., methylprednisolone) ± cyclophosphamide or rituximab.
High-Yield Points - ⚡ Biggest Takeaways
- Nephritic syndrome is an inflammatory process causing hematuria (RBC casts), oliguria, azotemia, and hypertension.
- Post-streptococcal glomerulonephritis (PSGN) is the classic prototype, typically affecting children 1-3 weeks after a GAS infection.
- Key labs show low C3 levels and elevated anti-streptolysin O (ASO) or anti-DNase B titers.
- Biopsy in PSGN reveals "lumpy-bumpy" granular immunofluorescence and characteristic subepithelial humps on electron microscopy.
- Management is primarily supportive.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

