Pathophysiology - Leaky Gut, Angry Bug
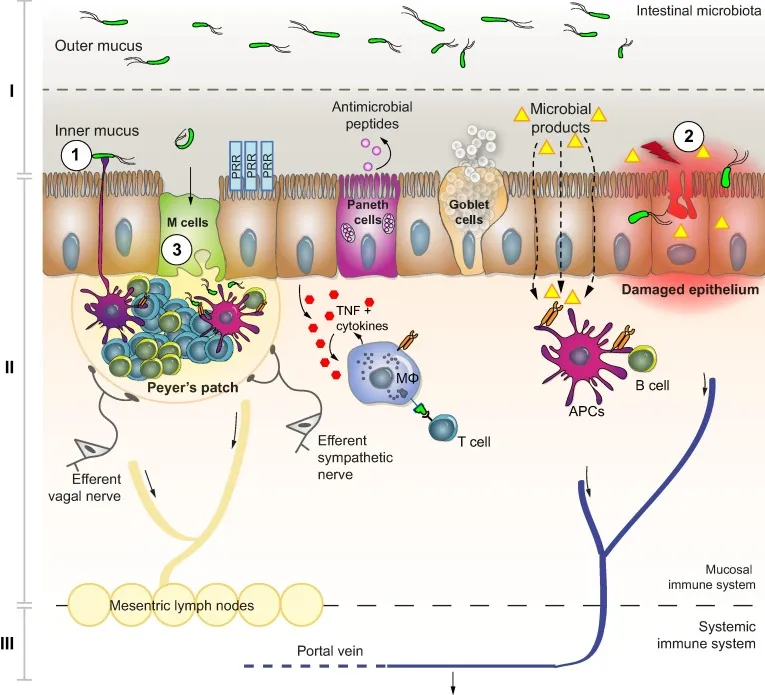
- Portal Hypertension & Cirrhosis → Gut edema, ↓ motility, & small intestinal bacterial overgrowth (SIBO).
- "Leaky Gut": ↑ Intestinal permeability allows bacteria to cross the gut wall (translocation).
- "Angry Bug" is a misnomer: The host is compromised, not the bug more virulent.
- Most common organisms: E. coli (~70%), Klebsiella, Strep. pneumo.
⭐ Ascitic fluid with low total protein (< 1 g/dL) has poor opsonic activity (↓ opsonins like complement), significantly increasing SBP risk.
Diagnosis - Tapping the Abdomen
- Indication: Perform diagnostic paracentesis in any patient with cirrhosis and ascites upon hospital admission, or with signs of infection (fever, pain) or clinical deterioration.
- Core Analysis:
- Cell Count: An ascitic fluid absolute polymorphonuclear (PMN) leukocyte count of ≥250 cells/mm³ is the primary diagnostic criterion.
- Culture: Essential for pathogen identification and sensitivity testing. Gram stain is low-yield.
- SAAG: Serum-Ascites Albumin Gradient. A value > 1.1 g/dL is consistent with portal hypertension.
⭐ High-Yield: Inoculating ascitic fluid into blood culture bottles at the bedside significantly increases the culture yield (~80%) compared to conventional sterile containers.
Management - Bug Juice Cocktails
- Empiric Antibiotics: Initiate immediately after paracentesis if SBP is suspected. Do not wait for culture results.
- Primary targets: E. coli, Klebsiella pneumoniae, Streptococcus pneumoniae.
- IV Albumin Adjunct: Co-administer with antibiotics.
- Dosing: 1.5 g/kg on day 1, then 1.0 g/kg on day 3.
- Prophylaxis (Secondary): To prevent recurrence.
- Daily Norfloxacin, Ciprofloxacin, or TMP-SMX.
⭐ IV albumin co-administration is critical; it significantly reduces the incidence of hepatorenal syndrome and improves short-term survival in patients with SBP.
Prophylaxis - Keeping Bugs at Bay
-
Primary Prophylaxis: For high-risk patients without prior SBP.
- Indicated if ascitic fluid protein is < 1.5 g/dL, plus either:
- Advanced liver failure (Child-Pugh score ≥ 9 & bilirubin ≥ 3 mg/dL)
- Renal dysfunction (Cr ≥ 1.2, BUN ≥ 25, or Na ≤ 130)
- Indicated if ascitic fluid protein is < 1.5 g/dL, plus either:
-
Secondary Prophylaxis: Lifelong prevention for any patient who has survived an episode of SBP.
-
Common Regimens:
- Daily oral ciprofloxacin or norfloxacin.
- Daily trimethoprim-sulfamethoxazole (TMP-SMX).
⭐ Patients with cirrhosis and an upper GI bleed are given short-term (e.g., 7 days) ceftriaxone prophylaxis due to a very high risk of developing SBP.
- SBP is an infection of pre-existing ascitic fluid without an evident intra-abdominal source, typically in patients with cirrhosis.
- Suspect in any patient with cirrhosis and ascites presenting with fever, abdominal pain, or altered mental status.
- Diagnosis is confirmed by paracentesis showing an ascitic fluid PMN count ≥ 250 cells/mm³.
- The most common pathogens are gram-negative bacteria, especially E. coli.
- Third-generation cephalosporins (e.g., cefotaxime, ceftriaxone) are the empiric treatment of choice.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

