Pathophysiology - Brain Under Siege
-
Ammonia ($NH_3$) Hypothesis: Central to HE. Gut bacteria produce $NH_3$, which bypasses the failing liver's urea cycle.
-
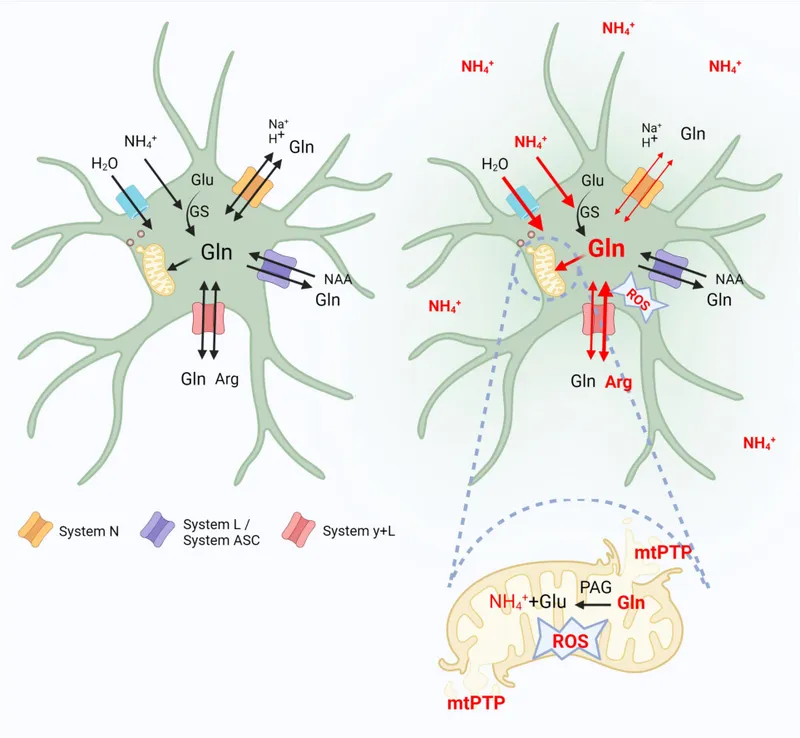
Astrocyte Injury: Brain astrocytes detoxify $NH_3$ by converting it to glutamine ($NH_3$ + glutamate → glutamine).
- This accumulation is osmotic, causing astrocyte swelling, cerebral edema, and ↑ intracranial pressure.
-
Other Factors:
- ↑ GABAergic Tone: Increased activity at the GABA-A receptor complex leads to neural inhibition.
- Inflammation: Systemic inflammatory response (e.g., from SBP) worsens HE.
- Manganese: Chronic deposition in basal ganglia contributes to motor symptoms.
⭐ Ammonia levels do not always correlate with the severity of hepatic encephalopathy, but a normal level can help rule it out.
Clinical Features & Staging - The Wobbly Patient
- Core Manifestations:
- Reversible neuropsychiatric syndrome, from subtle changes to deep coma.
- Early signs: Inverted sleep-wake cycle, shortened attention span, irritability.
- Asterixis: Bilateral "flapping" tremor of outstretched, dorsiflexed hands.
- Fetor Hepaticus: Sweet, musty odor on the breath (due to mercaptans).
- Staging (West Haven Criteria):
- Grade 1: Mild confusion, sleep disturbance.
- Grade 2: Lethargy, disorientation, obvious asterixis.
- Grade 3: Somnolent but arousable, marked confusion, incoherent speech.
- Grade 4: Coma, unresponsive to stimuli.
⭐ Asterixis is a form of negative myoclonus-an intermittent loss of postural tone. While classic for HE, it's not specific and can also be seen in uremia and CO₂ narcosis.
Diagnosis & Precipitating Factors - Unmasking the Culprit
- Diagnosis: Primarily clinical; a diagnosis of exclusion. Check serum ammonia (often ↑, but level doesn't correlate with severity). EEG may show classic triphasic waves.
- Precipitating Factors: Focus on identifying the trigger. Common culprits include GI bleed, infection (e.g., SBP), dehydration/diuretics, constipation, electrolyte disturbances (↓K+), and sedating drugs.
⭐ Serum ammonia levels do not correlate with the severity of hepatic encephalopathy and are not required for diagnosis or management.
Management - Taming the Toxins
Core goal: ↓ Ammonia ($NH_3$) production and absorption.
-
Identify & Treat Precipitating Factors:
- Infection (esp. SBP), GI bleed, electrolyte imbalance (↓K, metabolic alkalosis), constipation, renal failure, sedatives.
-
Primary Medical Therapy:
- Lactulose: First-line. Titrate to 2-3 soft stools/day.
- Rifaximin: Add-on if no improvement after 48 hrs or for secondary prophylaxis.
- Zinc: Consider supplementation, as deficiency can impair the urea cycle.
⭐ Hypokalemia worsens HE by increasing renal ammonia production. Always correct potassium levels, as it facilitates the conversion of $NH_3$ to $NH_4^+$ in the kidneys.
High‑Yield Points - ⚡ Biggest Takeaways
- Hepatic encephalopathy is a neuropsychiatric syndrome caused by ammonia accumulation from liver failure.
- The hallmark sign is asterixis (flapping tremor), alongside altered mental status and confusion.
- Always look for precipitating factors like GI bleeding, infection, or constipation.
- Diagnosis is primarily clinical; serum ammonia levels can support but are not always reliable.
- First-line treatment is lactulose, which traps ammonia in the colon.
- Rifaximin, a non-absorbable antibiotic, is often added as a second-line agent.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

