AMS Fundamentals - The Right Drug, Dose, Duration
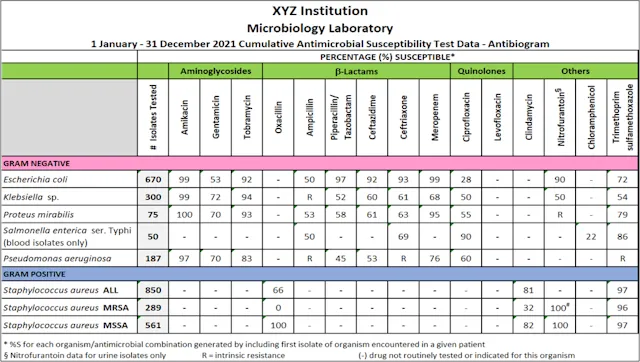
- Right Drug: Base empiric choices on local antibiogram. De-escalate to the narrowest effective agent based on culture results.
- Right Dose: Optimize using pharmacokinetics/pharmacodynamics (PK/PD).
- Time-dependent (e.g., β-lactams): More frequent dosing or prolonged infusions.
- Concentration-dependent (e.g., aminoglycosides): Higher doses, less frequent intervals.
- Adjust for renal and hepatic function.
- Right Duration: Use the shortest effective course. Procalcitonin can help guide cessation for respiratory tract infections.
⭐ A cornerstone of AMS is de-escalation: narrowing antibiotic spectrum and/or switching from IV to an equivalent oral agent once the patient is clinically stable. This reduces selective pressure for resistance.
Sepsis Stewardship - Hit Hard, Then Focus
- Initial Management (Hour-1 Bundle): Act fast. Upon suspicion of sepsis (e.g., qSOFA ≥2), immediately draw blood cultures, administer broad-spectrum antibiotics, measure lactate, and begin fluid resuscitation (30 mL/kg crystalloid for hypotension).
- De-escalation Principle: The cornerstone of sepsis stewardship. Re-evaluate therapy at 48-72 hours.
- Narrow antibiotic coverage based on culture and sensitivity results.
- Stop antibiotics if infection is unlikely.
⭐ Procalcitonin (PCT) levels can guide antibiotic de-escalation. A significant drop (>80% from peak) supports stopping antibiotics, reducing duration and resistance risk.
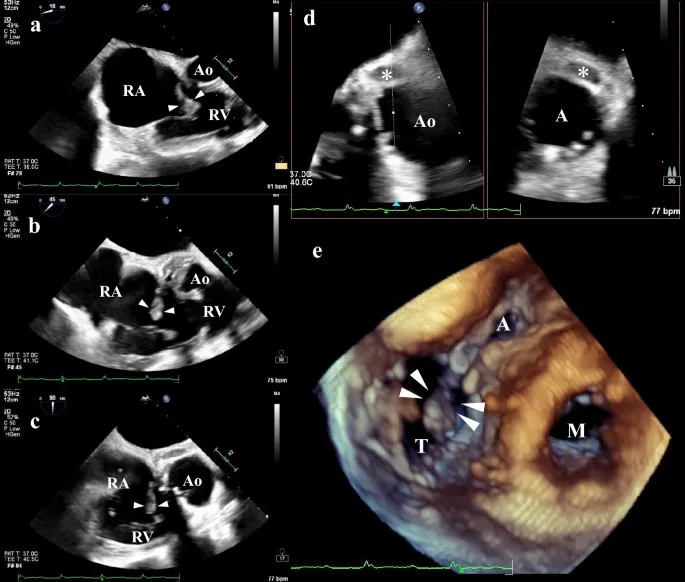
Endocarditis Endgame - Target the Tiny Terrors
- Core Goal: Prolonged, bactericidal, IV therapy tailored to the specific pathogen. Stewardship focuses on narrowing therapy once sensitivities are known.
- Culture is Critical: Always obtain ≥3 sets of blood cultures before starting empiric antibiotics. Diagnosis relies on modified Duke Criteria.
- Common Pathogens & De-escalation Targets:
- S. aureus: Nafcillin/Oxacillin (MSSA); Vancomycin (MRSA).
- Viridans Streptococci: Penicillin G or Ceftriaxone.
- Enterococcus: Ampicillin + Gentamicin (synergy).
- S. gallolyticus (bovis): See below!
- Therapy Duration: Typically 4-6 weeks. Monitor for drug toxicity (e.g., aminoglycoside nephrotoxicity) and clinical response.
⭐ Streptococcus gallolyticus endocarditis warrants a colonoscopy to screen for underlying colorectal cancer.
📌 FROM JANE: Fever, Roth spots, Osler nodes, Murmur, Janeway lesions, Anemia, Nail-bed hemorrhage, Emboli.
The Stewardship Toolkit - Measure What You Manage
- Core Principle: Track both processes & outcomes to demonstrate value and guide interventions.
- Process Measures (The "How"):
- Adherence to local/national guidelines.
- Antibiotic "timeout" completion rates at 48-72 hrs.
- Formulary restriction & pre-authorization compliance.
- Outcome Measures (The "What"):
- Financial: ↓ Antimicrobial acquisition costs.
- Microbiological: ↓ Rates of C. difficile, MRSA, VRE.
- Utilization Metrics: Days of Therapy (DOT), Defined Daily Doses (DDD).
⭐ A key success marker for stewardship programs is a significant reduction in hospital-onset Clostridioides difficile infection (CDI) rates.
High‑Yield Points - ⚡ Biggest Takeaways
- Sepsis management hinges on early recognition, prompt broad-spectrum antibiotics after blood cultures, and aggressive fluid resuscitation.
- Infective Endocarditis diagnosis relies on Duke criteria; empiric treatment often involves vancomycin to cover Staph/Strep.
- Antimicrobial stewardship focuses on the 4 D's: right Drug, Dose, Duration, and crucial De-escalation.
- De-escalation based on culture sensitivities is key to minimizing resistance.
- Procalcitonin (PCT) levels can guide stopping antibiotics, particularly in sepsis.
- Always prioritize source control (e.g., draining abscesses, removing infected lines).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

