Pathophysiology - The Gut's Uphill Battle
- Chronic Inflammation: The primary driver, causing mucosal damage and systemic catabolism.
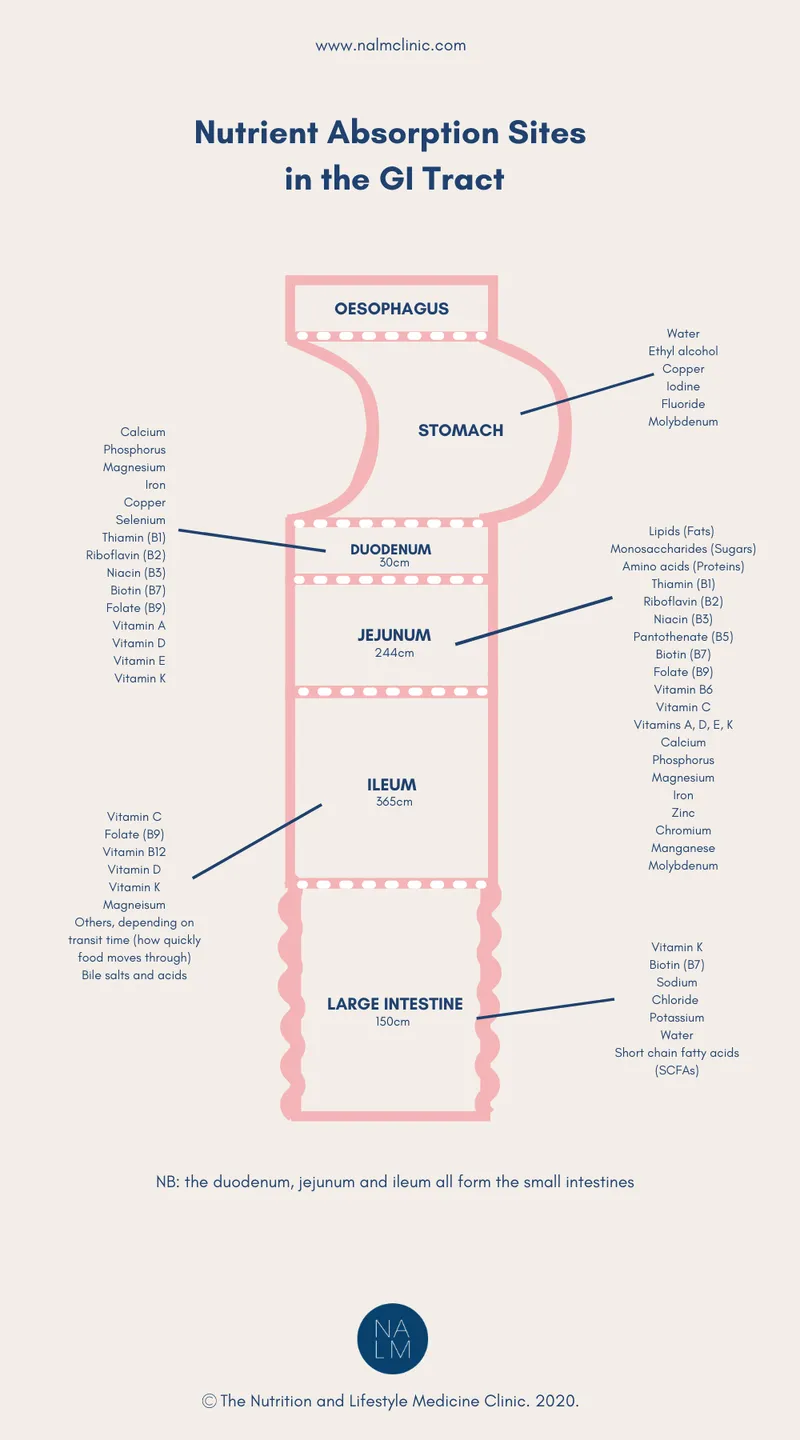
- Malabsorption: Reduced absorptive surface area from ulceration and villous atrophy. Specific sites matter (e.g., terminal ileum in Crohn's).
- Increased Gut Permeability: "Leaky gut" allows translocation of bacterial products, fueling inflammation.
- Increased Energy Expenditure:
- Systemic inflammation (↑ cytokines) and fever raise the basal metabolic rate.
- Protein-losing enteropathy from inflamed mucosa.
- Decreased Oral Intake:
- Anorexia, nausea, abdominal pain, and fear of eating (sitophobia).
⭐ Crohn's disease of the terminal ileum classically impairs the absorption of Vitamin B12 and bile salts, leading to megaloblastic anemia and fat-soluble vitamin deficiencies.
Micronutrient Deficiencies - The Nutrient Lineup
IBD disrupts nutrient absorption, leading to key deficiencies.
- Iron: Most common deficiency. Caused by chronic blood loss and inflammation (anemia of chronic disease).
- Vitamin B12: Classic in Crohn's disease due to terminal ileitis or resection.
- Folate: Malabsorption; also impaired by medications like sulfasalazine and methotrexate.
- Fat-Soluble Vitamins (A, D, E, K): Bile salt malabsorption in ileal disease impairs absorption.
- Vitamin D & Calcium: Risk of osteoporosis is high, exacerbated by corticosteroid use. Monitor bone density.
- Zinc: Lost through diarrhea and fistulas; essential for mucosal healing.
- Selenium: Reduced levels due to inflammation and poor intake.
⭐ Always suspect Vitamin B12 deficiency in a Crohn's patient with megaloblastic anemia and neurological symptoms, especially with a history of ileal resection.
Dietary Therapy - Food as Pharmacy
- Goal: Induce/maintain remission, correct nutritional deficiencies, & manage symptoms (e.g., bloating, pain).
- Exclusive Enteral Nutrition (EEN):
- First-line induction therapy in pediatric & adult Crohn's Disease.
- Provides 100% of caloric needs as a liquid formula for 6-8 weeks.
- Symptom-Targeted Diets:
- Low-FODMAP: For functional symptoms like gas & bloating.
- Low-Residue/Fiber: For patients with strictures to minimize obstruction risk.
⭐ Exclusive Enteral Nutrition (EEN) is as effective as corticosteroids for inducing remission in Crohn's disease, with superior mucosal healing and an improved safety profile, especially in children.
- Emerging Therapies: Crohn's Disease Exclusion Diet (CDED) and Specific Carbohydrate Diet (SCD) are being studied as maintenance options.
Nutritional Support - Pipeline Power
- Enteral Nutrition (EN): Preferred "gut-first" route for moderate-severe disease or malnutrition. Polymeric formulas are standard.
- Aims to correct deficits, support healing, and can be a primary therapy to induce remission (especially in pediatric Crohn's).
- Parenteral Nutrition (PN): Used only when the GI tract is non-functional.
- Indications: Complete bowel obstruction, high-output fistulas, severe short bowel syndrome.
- ⚠️ Higher risk of line sepsis, cholestasis, and metabolic issues.
⭐ Exclusive Enteral Nutrition (EEN) is a first-line therapy for inducing remission in pediatric Crohn's disease, rivaling corticosteroids with a better safety profile and promoting superior mucosal healing.
High-Yield Points - ⚡ Biggest Takeaways
- Malnutrition is a universal concern in IBD, stemming from poor intake, malabsorption, and inflammation-driven catabolism.
- Enteral nutrition can induce remission in Crohn's disease, particularly in pediatric patients; less effective in UC.
- Total Parenteral Nutrition (TPN) is reserved for severe disease, obstruction, or short bowel syndrome.
- Routinely screen for deficiencies, especially iron, B12, vitamin D, and zinc.
- Folic acid supplementation is crucial with sulfasalazine or methotrexate use.
- Low-residue/low-fiber diets are for symptom control during active flares only.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

